Session Information
Date: Monday, November 9, 2020
Title: Pediatric Rheumatology – Clinical Poster III: SLE, Vasculitis, & JDM
Session Type: Poster Session D
Session Time: 9:00AM-11:00AM
Background/Purpose: Kawasaki disease (KD), a well described vasculitis of childhood, is the leading cause of acquired heart disease in developed countries. Kawasaki disease shock syndrome (KDSS) has been described in a limited number of small single center cohorts and case reports but its incidence and prognosis are poorly understood. Here we aim to add to the existing body of knowledge by describing patients with the diagnoses of KD and shock at our institution.
Methods: With IRB approval, the electronic medical record was used to retrospectively identify a total of 9286 PICU admissions between March 2012 and February 2016, 269 of whom had rheumatology consult. Of those 269, 30 patients (11 %) had KD and 27 (90%) had the specific diagnosis of KDSS. Five patients were excluded whose hypotension was documented after IVIG initiation and seven patients were excluded who did not have documented evidence of shock. The diagnosis of shock was confirmed by the combination of clinical concern requiring PICU admission and objective evidence, defined by hypotension for age or laboratory evidence of impaired perfusion (lactate > 2.0 mmol/L or mixed venous sat < 70%). The 18 remaining patients’ charts were reviewed for the features presented in tables and results.
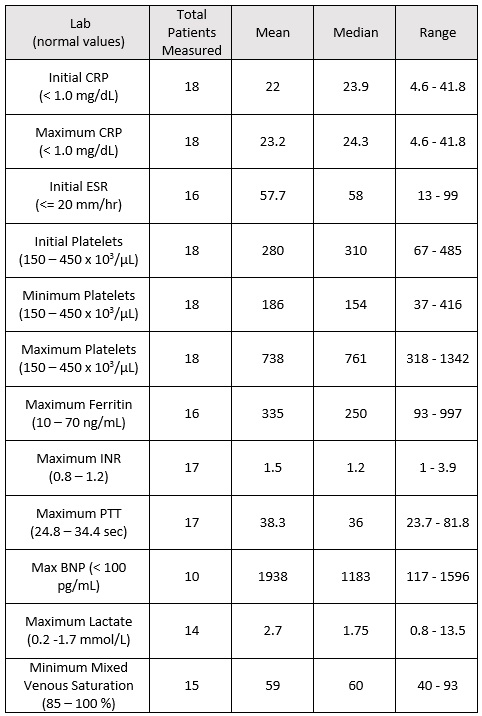
Results: The patients described in our cohort were predominantly African American (39%) and Hispanic (44%) and mostly male (61%) (table 1). The median age was 3.9 years and the median duration of fever was 8 days (table 2). Laboratory values are provided in table 3. Eight (44%) patients required inotropic support for their shock with one requiring extracorporal membrane oxygenation (ECMO). The shock was mostly distributive in nature with only one patient presenting with isolated cardiogenic shock with pulmonary edema. Fifteen patients (83%) received pulse dose steroids, 11 (61%) received daily steroids and 3 (17%) received no steroids. Steroids were given an average of 2 days after the first IVIG. Five patients (28%) received a second IVIG. Two patients received infliximab after fever resolution. On initial echocardiograms, six patients (33%) had systolic dysfunction and two (11%) had coronary dilation with z-score > 2.5. On the 6-8 week echocardiogram, three (17%) had coronary dilation with z-score > 2.5 but this had resolved by recent follow-up in all but one patient (6%). The prevalence of shock in KD was 1 in 27 patients, while prevalence of KDSS in the PICU was 1 in 550 admissions.
Conclusion: All of our KDSS patients had good coronary outcomes except one patient who required ECMO. Our coronary outcomes at last echo were better than previously published data and the majority of our patients received steroids. However, there were 3 patients who received no steroids and also had good coronary outcomes. The steroids were not typically given immediately as distinguishing KDSS from sepsis without blood cultures can be challenging. The true utility of steroids is limited by the small cohort size and variety of dosing regimens. KDSS is an uncommon diagnosis in the PICU and it is important for the intensivist to consider this diagnosis in patients presenting with shock.
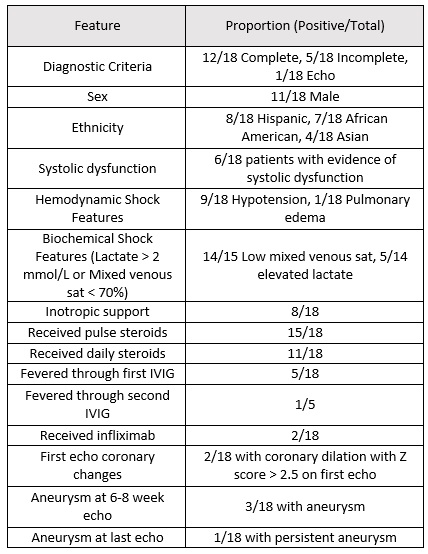 Table 1: Patient Characteristics, Shock Features, Coronary Outcome
Table 1: Patient Characteristics, Shock Features, Coronary Outcome
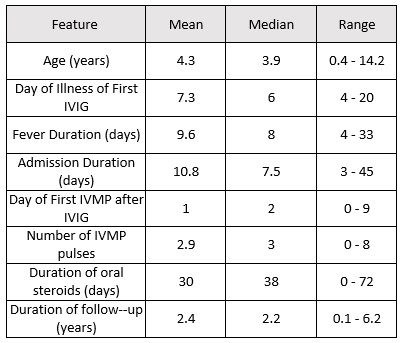 Table 2: Patient Age and Therapy
Table 2: Patient Age and Therapy
To cite this abstract in AMA style:
Bray M, Rammel J, Ramirez A, Sexson K, Lam F, Muscal E, DeGuzman M. Kawasaki Disease Shock Syndrome in the Intensive Care Unit: A Single Center Cohort [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/kawasaki-disease-shock-syndrome-in-the-intensive-care-unit-a-single-center-cohort/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/kawasaki-disease-shock-syndrome-in-the-intensive-care-unit-a-single-center-cohort/