Session Information
Session Type: Poster Session A
Session Time: 8:30AM-10:30AM
Background/Purpose: The presence of anti-citrullinated protein antibodies (ACPAs) is a highly specific hallmark of rheumatoid arthritis (RA), that is present also in early disease. However, 20% of RA subjects test negative for ACPA and thus their early diagnosis and treatment may be delayed. Furthermore, despite the high specificity of the cyclic citrullinated tests, their low sensitivity indicates that a negative result does not rule out the disease. Therefore, an increased knowledge about the presence of other circulating biomarkers related with early RA is needed to improve its diagnosis and to better understand the pathogenic mechanisms underlying the different RA subsets. In this study, we aimed to search for plasma autoantibodies associated with ACPA status that could be useful to assist the early diagnosis of RA.
Methods: We firstly profiled the plasma IgG and IgA repertoire of 80 ACPA positive and 80 ACPA negative subjects entering the Epidemiological Investigation of Rheumatoid Arthritis (EIRA) early RA cohort. To this end, we employed an antigen suspension bead array built with 260 protein fragments within Human Protein Atlas and selected from an initial untargeted screening on planar arrays. A validation phase using a suspension bead array including 27 antigens was carried out on another set of samples from EIRA which included 386 ACPA positive, 358 ACPA negative and 372 age and sex-matched control subjects. A sample-specific threshold was selected to determine the reactivity of all the samples. The Wilcoxon rank sum test and Fisher’s test were applied for the comparison of autoantibody levels and reactivity frequencies between the sample groups.
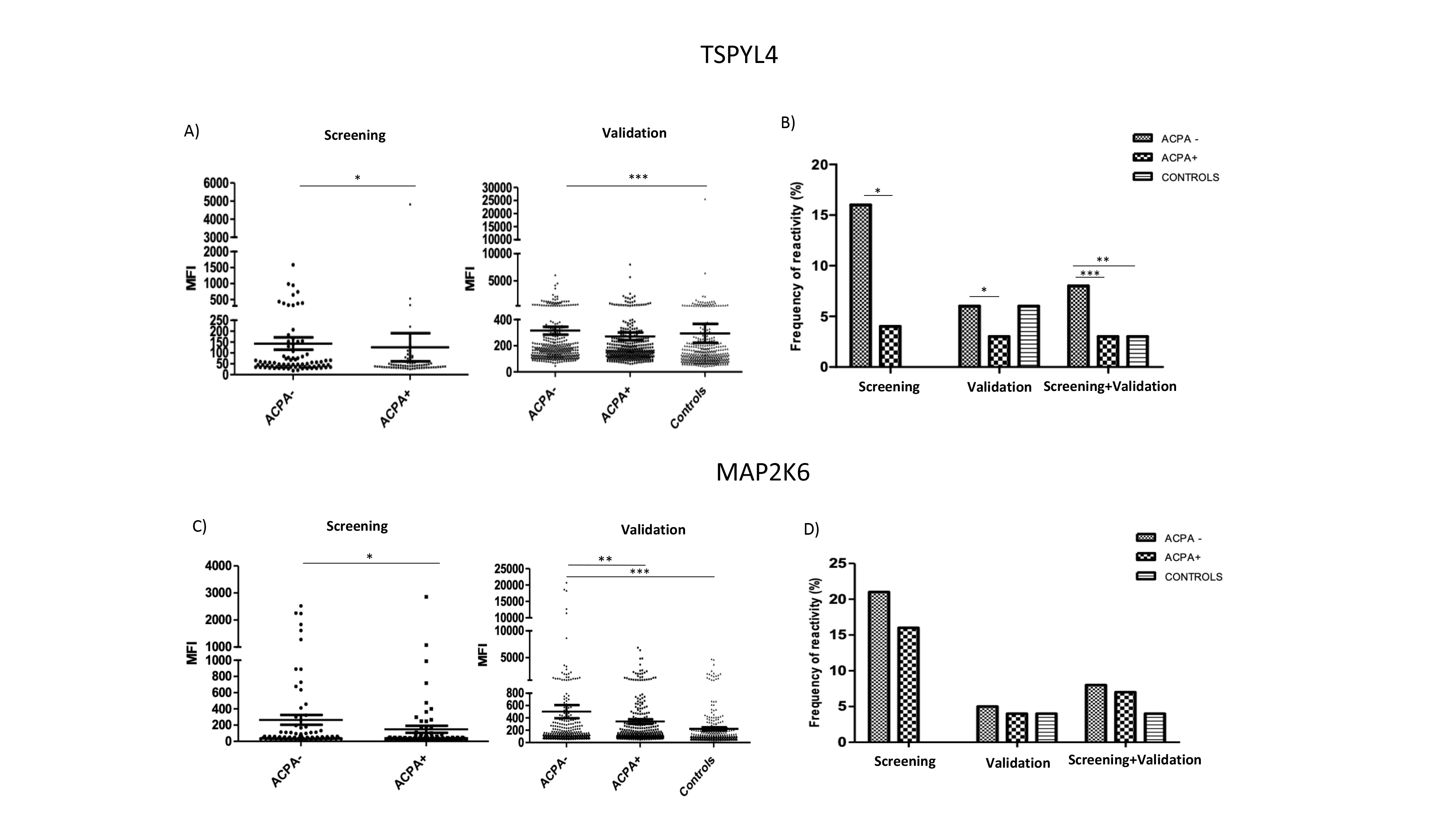
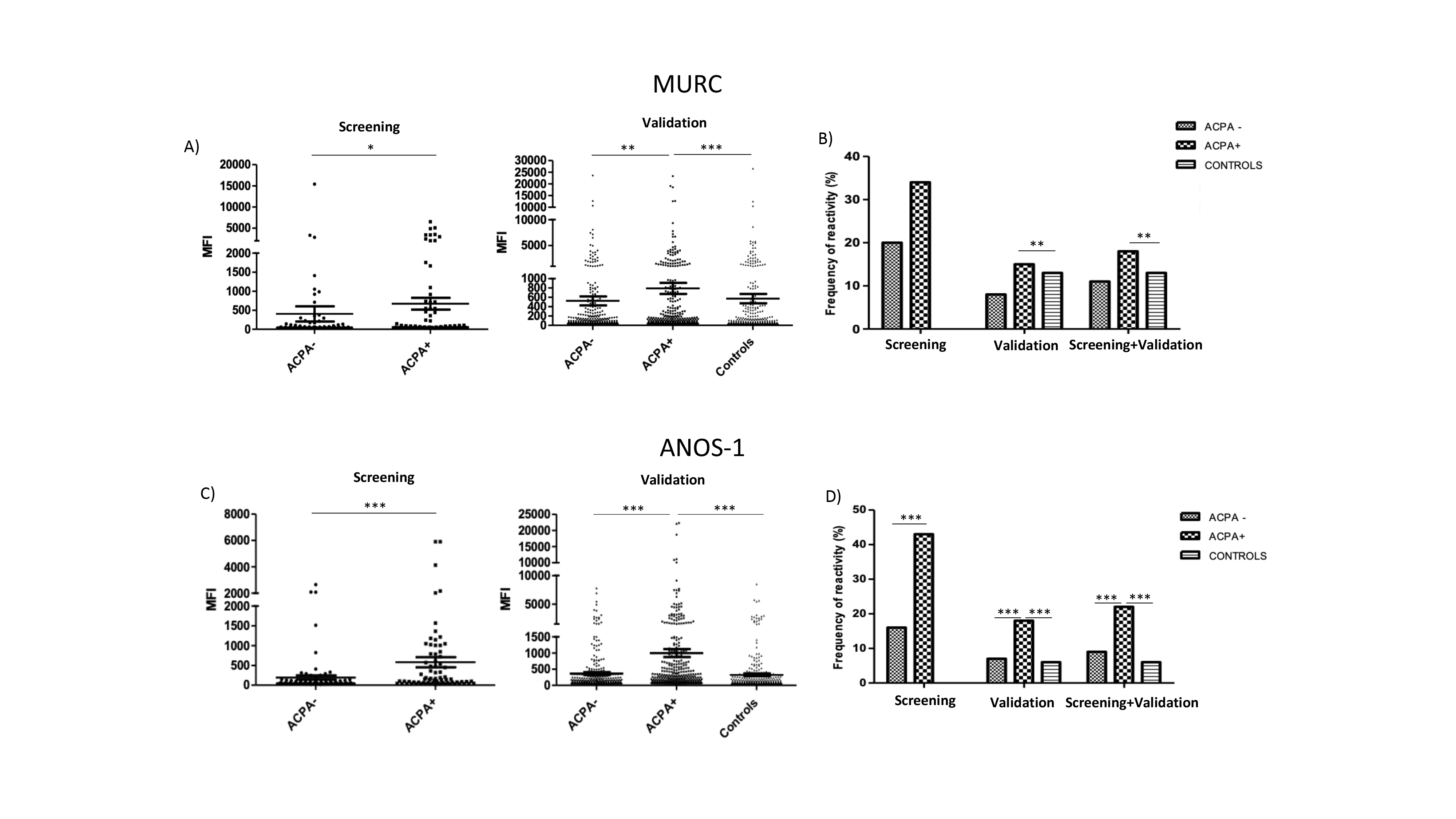
Results: Reactivities towards four different antigens were significantly associated to ACPA status (Figure 1 and Figure 2). IgG autoantibody levels towards Testis-specific Y-encoded-like protein 4 (TSPYL4) were higher in ACPA negative subjects compared to controls (Figure 1A). The prevalence of IgG autoantibodies towards TSPYL4 was also higher in ACPA negative compared to ACPA positive (8% vs. 3%) (Figure 1B). Higher IgG autoantibody levels towards dual specificity mitogen-activated protein kinase kinase 6 (MAP2K6), were also observed in ACPA negative subjects compared to ACPA positive and controls, but no differences were observed on their prevalence (Figure 1C,1D). In contrast, higher IgG autoantibody levels towards muscle related coiled-coil protein (MURC) and Anosmin-1 (ANOS-1) were observed in ACPA positive individuals compared to ACPA negative and controls (Figure 2A, 2C). The prevalence of IgG autoantibodies towards ANOS-1 was also higher in ACPA positive subjects compared with ACPA negative and controls (22%, 9% and 6% respectively) (Figure 2D). Interestingly, three out of the four antigens discovered are highly expressed in lungs and heart, two of the extraarticular sites affected in RA. No significant differences were validated at IgA reactivity levels for any of the antigens analyzed.
Conclusion: Although further validation in other early RA sample cohorts is needed, our data suggest the measurement of these four autoantibodies might be useful to assist the early diagnosis of RA and give insight into its pathogenesis.
To cite this abstract in AMA style:
Lourido L, Ruiz-Romero C, Collado L, Hansson M, Klareskog L, Sjöberg R, Pin E, Nilsson P, Blanco-García F. Identification and Validation of Four Circulating Autoantibodies Associated with the ACPA Status in Early Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/identification-and-validation-of-four-circulating-autoantibodies-associated-with-the-acpa-status-in-early-rheumatoid-arthritis/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/identification-and-validation-of-four-circulating-autoantibodies-associated-with-the-acpa-status-in-early-rheumatoid-arthritis/