Session Information
Date: Friday, November 6, 2020
Title: SLE – Diagnosis, Manifestations, & Outcomes Poster I: Clinical Manifestations
Session Type: Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: Cutaneous lupus erythematosus (CLE) is a photosensitive skin disorder that can occur with systemic lupus erythematosus. As CLE often fluctuates in disease activity, little is known about the rates of disease remission and recurrence in patients with CLE. In this retrospective study, we assessed the rates of remission and recurrence in a longitudinal cohort study of 97 CLE patients, and identified clinical factors associated with each of these outcomes.
Methods: Inclusion criteria included CLE patients with at least three study visits spanning at least six months. The primary outcomes were remission and recurrence of disease activity. The secondary outcomes were time to remission from the baseline visit, and time to recurrence from documented remission. Disease remission was defined as reaching Cutaneous Lupus Erythematosus Activity and Severity Index activity (CLASI-A) equal to 0. Disease recurrence was defined as having a CLASI-A≥1 after remission. Univariate and multivariable analyses were performed to identify clinical and demographic risk factors associated with disease remission and recurrence. Time to remission and recurrence of activity was calculated by survival curve analyses. Significant variables associated with disease remission based on survival curve analyses were then used to perform a Cox proportional hazards model to identify variables that are predictive of shorter time to remission.
Results: 46 patients (48%) reached remission of CLE activity. Median time to remission was 5.45 years from the initial visit. Patients who achieved remission less likely to have discoid lupus erythematosus (DLE) (OR:0.20 (95% CI: 0.05-0.70), p=0.01) and more likely to have milder baseline disease activity (OR:1.75 (1.30-2.38), p< 0.001). Cox proportional hazards regression model showed that the absence of DLE (HR:4.20 (1.98-8.92) and lifetime non-smoker history (HR:2.57 (1.22-5.43)) were predictors of shorter time to remission (Figure 1). 29 patients (63%) of participants experienced disease recurrence within a median of 2.1 years from their remission date. Univariate analyses showed patients with recurrence of CLE activity had a longer disease duration prior to their baseline visit (p=0.002), and were more likely to have DLE (72% v. 29%, p=0.005), but were not significant in the multivariable analyses.
Conclusion: We found that CLE patients with mild baseline disease activity and do not have DLE are more likely to attain disease remission. The presence of discoid lesions and positive smoking history are associated with longer time to remission on standard-of care therapies. These findings can be helpful for clinicians to guide CLE patients on their potential disease course.
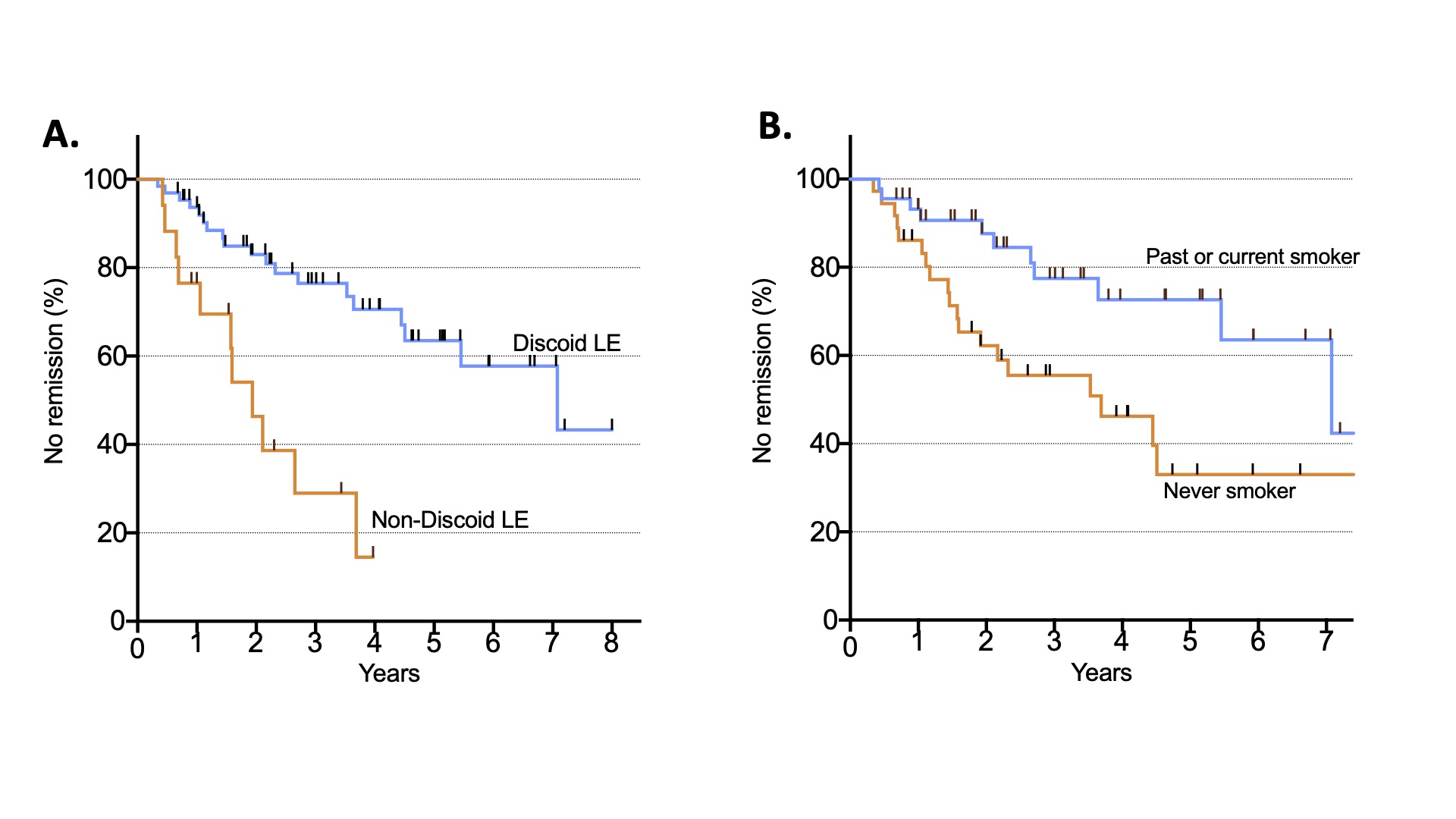 Factors associated with remission of disease activity in patients with cutaneous lupus. Patients without discoid rash (A) (HR:4.20 (1.98-8.92) and without a smoking history (HR:2.57 (1.22-5.43) (B) have a significantly shorter time to disease remission.
Factors associated with remission of disease activity in patients with cutaneous lupus. Patients without discoid rash (A) (HR:4.20 (1.98-8.92) and without a smoking history (HR:2.57 (1.22-5.43) (B) have a significantly shorter time to disease remission.
To cite this abstract in AMA style:
Florez-Pollack S, Rizvi S, Chong B, Hynan L. Factors Associated with Disease Activity Remission and Recurrence in Cutaneous Lupus Erythematosus [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/factors-associated-with-disease-activity-remission-and-recurrence-in-cutaneous-lupus-erythematosus/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/factors-associated-with-disease-activity-remission-and-recurrence-in-cutaneous-lupus-erythematosus/
