Session Information
Date: Sunday, November 8, 2020
Title: Sjögren’s Syndrome Poster
Session Type: Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: Juvenile Sjögren’s Syndrome (jSS) is a perplexing systemic autoimmune disease in children presenting with positive autoantibodies, glandular, and/ or extraglandular symptoms. In pediatric practice, the diagnosis has relied upon the positivity of ANA and SSA/ SSB antibodies, so-called classic Sjögren antibodies (cSjA). Children with negative cSjA autoantibodies or exclusively extraglandular symptoms become a diagnostic challenge. Early Sjögren antibodies (eSjA) including IgG, IgA and IgM autoantibodies to salivary protein 1 (SP-1), carbonic anhydrase 6 (CA6), and parotid secretory protein (PSP), are 9 novel salivary gland autoantibodies. The eSjA were found to be early biomarkers in adults, especially in negative cSjA cases. The roles of ANA, cSjA, and eSjA as biomarkers and predictors for abnormal minor labial salivary gland biopsy (MSGB) have been unknown in jSS. The goal of this study is to determine if ANA, cSjA, and eSjA can serve as biomarkers and predictors for abnormal minor salivary gland biopsy (MSGB) in the University of Florida (UF) cohort with jSS.
Methods: Forty children with a new-onset jSS diagnosed at the UF Health Shands Children’s hospital and the UF Health Oral Medicine between January 2017-May 2020 were evaluated retrospectively. Autoantibodies were positive if ANA was 1:160 or higher or one of cSjA and eSjA were higher than normal values. A MSGB was abnormal if the focus score was 1 or more. The sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV) of ANA, cSjA, and eSjA were analyzed using the MSGB as a gold standard.
Results: Thirty-two children 5-17 years of age (mean 12.28 , median 14) who underwent testing for ANA, cSjA, eSjA, and MSGB were included. Twenty-three children fulfilled the 2016 ACR/EULAR SS classification criteria. Abnormal MSGB results were found in 5 of 9 children who have not fulfilled the criteria. One child with normal MSGB has fulfilled the criteria. Twelve and five of the children had positive SSA and SSB antibodies respectively. All but 1 of the positive SSB patients were also SSA positive. Twenty-two children had at least one positive eSjA with anti-CA6 IgG, the most prevalent novel antibodies (52%). Abnormal MSGB with a focus score of 1 and more than 1 were found in 2 and 25 children, respectively. Three of the four children with all negative autoantibodies still had abnormal MSGB. The sensitivity, specificity, PPV, and NPV of each autoantibody is shown in Table 1. The eSjA has the highest PPV and NPV. The combination of eSjA and ANA or cSjA or both slightly increased sensitivity, but not specificity, PPV or NPV of eSjA.
Conclusion: eSjA are a potential biomarker and reliable predictor of abnormal MSGB in jSS. Patients with negative autoantibodies did not entirely exclude a diagnosis of jSS since these biomarkers have a low NPV. MSGB should still be considered in any case with a high index of suspicion with negative autoantibodies.
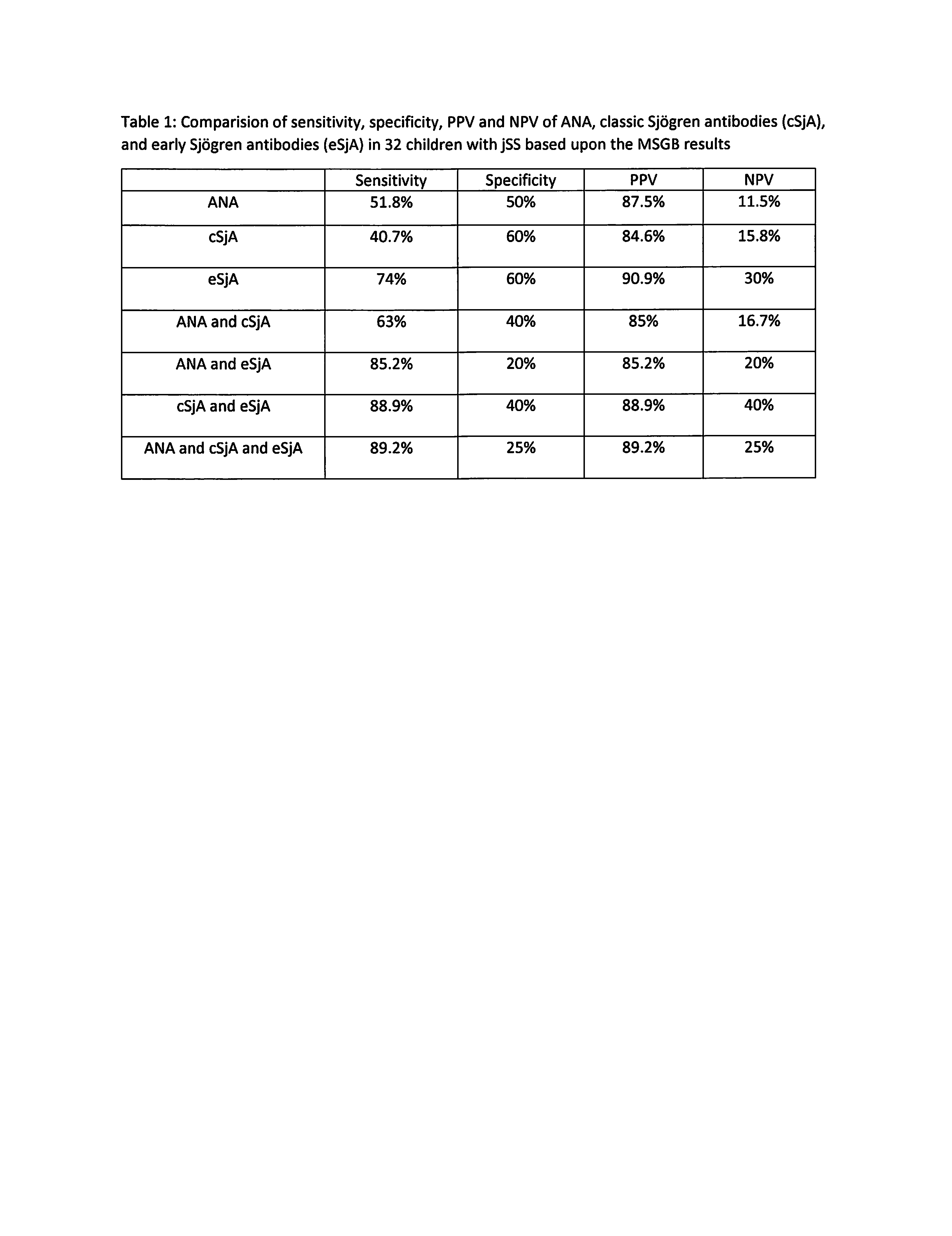 Table 1: Comparision of sensitivity, specificity, PPV and NPV of ANA, classic Sjögren antibodies (cSjA), and early Sjögren antibodies (eSjA) in 32 children with jSS based upon the MSGB results
Table 1: Comparision of sensitivity, specificity, PPV and NPV of ANA, classic Sjögren antibodies (cSjA), and early Sjögren antibodies (eSjA) in 32 children with jSS based upon the MSGB results
To cite this abstract in AMA style:
Thatayatikom A, Thatayatikom S, Bhattacharyya I, Elder M, Modica R, Cha S. Early Sjögren Antibodies: Potential Biomarker for Abnormal Minor Labial Salivary Gland Biopsy in Juvenile Sjögren’s Syndrome [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/early-sjogren-antibodies-potential-biomarker-for-abnormal-minor-labial-salivary-gland-biopsy-in-juvenile-sjogrens-syndrome/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/early-sjogren-antibodies-potential-biomarker-for-abnormal-minor-labial-salivary-gland-biopsy-in-juvenile-sjogrens-syndrome/
