Session Information
Session Type: Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose: The pathogenesis of pediatric uveitis remains unclear. Studies of biomarkers using aqueous humor (AqH) identified S100 proteins, cytokines, and chemokines as potential biomarkers of uveitis activity. AqH collection is invasive and less feasible. Tears may serve as a surrogate as the same biomarkers present in AqH were detected in tears of uveitis patients. We showed that S100A12, IL-8, and sICAM-1 levels differ based on uveitis activity in JIA-associated uveitis (JIA-U). We aim to determine if tear-based biomarkers differ in a patient’s eyes based on uveitis activity by laterality and diagnoses.
Methods: Tears were collected by Schirmer strips from children ≥5 years old with diagnosis of bilateral uveitis. Uveitis activity was graded by SUN criteria. Anterior chamber (AC) cell grade < 0.5 was inactive. AC grades ≥0.5+ were active. S100A8, A9 and A12 were measured by ELISA, and IL-18, IL-8, IP-10, MCP-1, RANTES and sICAM-1 by Luminex assays. Biomarkers levels were assessed between paired eyes of a person by 1) unilateral activity (active eye and inactive contralateral eye), 2) bilateral activity (both active eyes), and 3) diagnosis (JIA-U vs non-JIA-U).
Results: Fifteen children contributed 34 tear samples (JIA-U n=8; idiopathic chronic anterior uveitis n=5; and idiopathic uveitis n=2). At time of tear collection, 53% had bilateral active uveitis (53% AC cell grade 0.5+). Treatment included topical (82%) and systemic therapy (76%) (Table 1). Stratifying by laterality, all biomarker levels were similar between the active uveitic eye and the inactive contralateral uveitic eye in those with unilateral active uveitis. In bilateral active uveitis, levels were also similar in both eyes except for S100A12 that was lower in the higher-grade uveitic eye (7979 pg/ML-/+SD 7835) compared to the lower-grade (25,727+/- 39,154; P=0.032). Stratifying by diagnosis, children with JIA-U relative to non-JIA-U group, primarily had unilateral active uveitis (78 vs 25%) with AC cell grade 0.5+ (100 vs 53%), greater use of systemic therapy (89 vs 63%) with similar use of topical steroids (83 vs 81%). Regardless of uveitis activity, biomarkers levels between both eyes of children with JIA-U were similar. In non-JIA-U, only S100A12 was higher in the lower-grade or inactive eye. All other biomarkers levels were similar. Comparing eyes of children with JIA-U and non-JIA-U, the JIA-U group had significantly higher S100A12, IL-8, RANTES, and sICAM than non-JIA-U (Table 2).
Conclusion: Our results suggest that S100A12 levels may differ in the eyes of children with a history of bilateral uveitis who have bilateral active disease especially non-JIA-U. Although we expected a difference in biomarker levels of paired eyes of children with unilateral active uveitis, earlier damage to the blood-ocular barrier may allow crossing of biomarkers to the inactive uveitic eye. Use of topical steroids may also dampen the inflammatory response. Elevated S100A12, sICAM, and IL-8 in children with JIA-U compared to non-JIA-U supports the potential role of neutrophils in JIA-U. A limitation of our study is sample size. Further work is needed to clarify the impact of topical steroids on biomarkers levels and the role of S100A12, sICAM1, and IL-8 in uveitis activity.
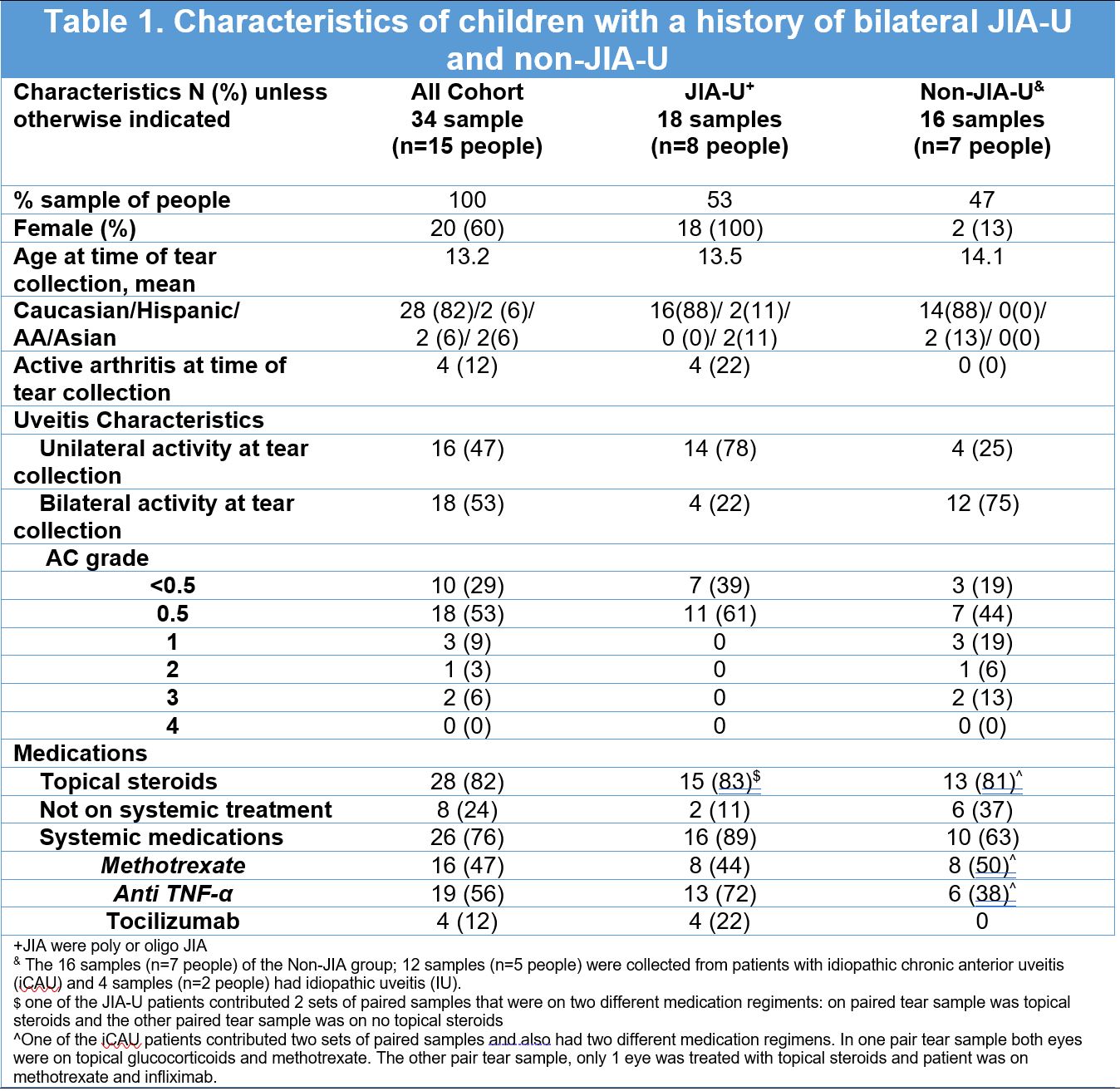 Table 1: Clinical characteristics
Table 1: Clinical characteristics
 Table 2: Tear biomarker levels between JIA-U and non-JIA-U
Table 2: Tear biomarker levels between JIA-U and non-JIA-U
To cite this abstract in AMA style:
Rodriguez-Smith J, Miraldi Utz V, Cassedy A, Thornton S, Schulert G, Sproles A, Mwase N, Hennard T, Altaye M, Grom A, Angeles-Han S. Comparing S100 Proteins and Cytokine Levels in Tears Based on Uveitis Activity Laterality in Children with JIA-associated Uveitis and Non-JIA-U [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/comparing-s100-proteins-and-cytokine-levels-in-tears-based-on-uveitis-activity-laterality-in-children-with-jia-associated-uveitis-and-non-jia-u/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/comparing-s100-proteins-and-cytokine-levels-in-tears-based-on-uveitis-activity-laterality-in-children-with-jia-associated-uveitis-and-non-jia-u/
