Session Information
Date: Sunday, November 7, 2021
Title: Patient Outcomes, Preferences, & Attitudes Poster II: Measurements (0739–0763)
Session Type: Poster Session B
Session Time: 8:30AM-10:30AM
Background/Purpose: Uptake of treat to target strategies for the management of rheumatoid arthritis (RA) is low. While there are known system-related barriers to accessing treatment, poor primary (starting) and secondary (continuing) adherence are prevalent causes of suboptimal care. The objective of this study was to better understand the heterogeneity in patients’ conceptualization of treatment of RA in order to inform interventions aimed at improving appropriate utilization of DMARDs.
Methods: Participants were recruited from an online research registry. Those meeting eligibility criteria [physician diagnosed RA currently being treated with DMARD(s)] rated 56 items (coded on 5-point scales with appropriate anchors) reflecting concepts raised during preparatory in-depth individualized patient interviews. To combine similar items for ease of analysis and interpretation we conducted a principal components analysis using Varimax rotation. We then entered mean scores, weighted by how heavily each item loaded onto each factor, into a k-means cluster analysis. We examined whether demographic characteristics differed across clusters using ANOVA and chi-square for continuous and categorical variables, respectively.
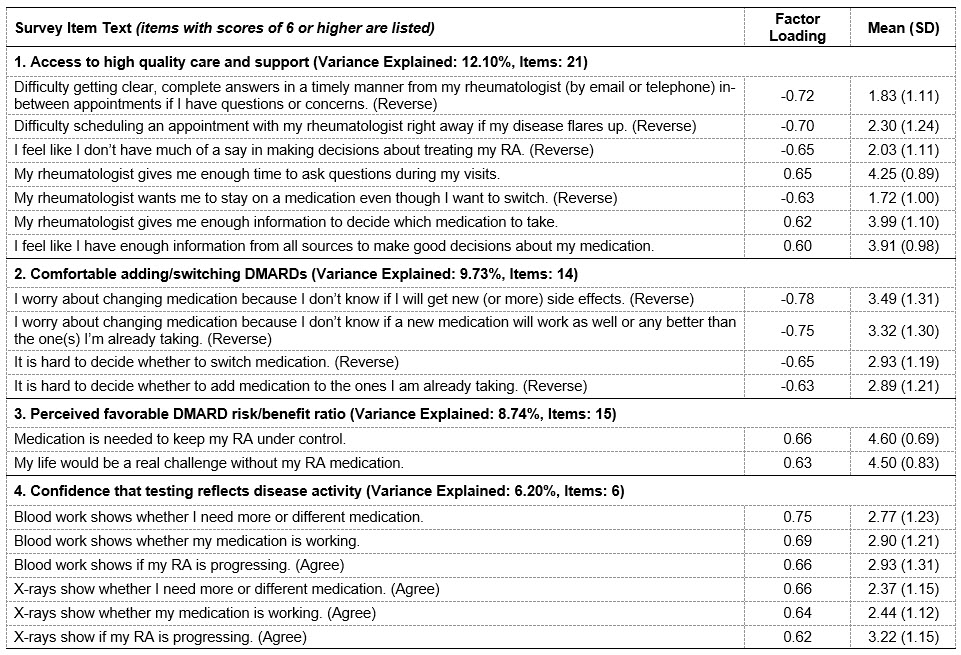
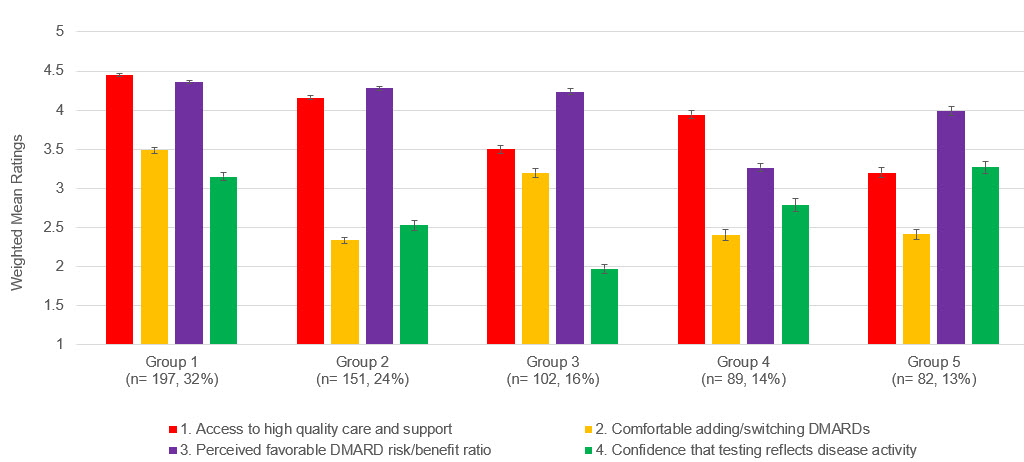
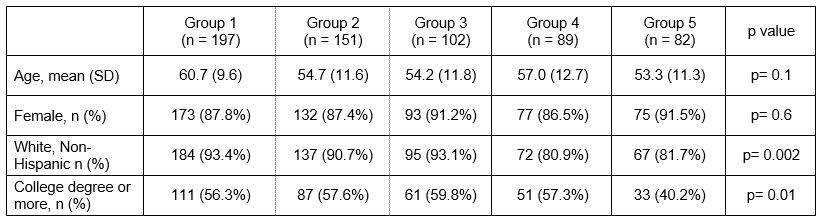
Results: Participants (N= 621) ranged in age from 22 to 93, with a mean of 57 years old (SD= 11.5). Most (89%) were female and reported themselves to be non-Hispanic white (89%); 27% reported having a post-graduate degree. A scree plot revealed that a 4-factor solution explaining 36.8% of the variance would provide desirable interpretability, with a discontinuous drop in eigenvalues for additional factors slowly tapering and adding little discriminability between later solutions. The four factors (% variance explained, number of items) were: 1) Access to high quality care and support (12.10%, n= 21); 2) Comfortable adding/switching DMARDs (9.73%, n= 14); 3) Perceived favorable DMARD risk/benefit ratio (8.74%, n= 15); and 4) Confidence that testing reflects disease activity (6.20%, n= 6). Table 1 lists the mean ratings for items with factor loading scores of 6 or greater. A 5-cluster solution showed the most stable convergence of cluster centers after 10 iterations. Figure 1 shows the weighted mean scores for each factor across clusters. While four out of the five groups perceived a favorable DMARD risk/benefit ratio, all groups voiced some discomfort with adding or changing DMARDs, with Groups 2, 4 and 5 having particularly low scores. Level of comfort adding/switching DMARDs was not mitigated by access to high quality care and support. There were a greater number of non-white participants in Groups 4 and 5, and less well-educated participants in Group 5 (Table 2). No differences in age or sex across groups were observed.
Conclusion: Patients’ conceptualization of RA treatment varies. However, adding/switching DMARDs appears to be ubiquitous regardless of the perceived benefits associated with DMARDs and access to high quality care and support. Interventions outside of the traditional physician-patient relationship are needed to facilitate treatment escalation in patients with RA. Further research is required to understand residual variance not explained by our model.
To cite this abstract in AMA style:
Hsiao B, Downs J, Lanyon M, Harrold L, Curtis J, Blalock S, Wiedmeyer C, VENKATACHALAM S, Nowell W, Fraenkel L. Understanding Heterogeneity in Patients’ Conceptualization of Treatment for Rheumatoid Arthritis: A Cluster Analysis [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/understanding-heterogeneity-in-patients-conceptualization-of-treatment-for-rheumatoid-arthritis-a-cluster-analysis/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/understanding-heterogeneity-in-patients-conceptualization-of-treatment-for-rheumatoid-arthritis-a-cluster-analysis/