Session Information
Session Type: Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose: Cardiac involvement, including electrocardiogram (ECG) abnormalities, is associated with worse prognosis in systemic sclerosis (SSc). We studied the incidence, risk factors and outcomes of conduction and rhythm disorders in a population-based cohort of patients with SSc and non-SSc comparators from the same geographic area.
Methods: A previously identified incident cohort of SSc patients (1980-2016) in a well-defined geographic area was compared to a randomly selected 2:1 cohort of age- and sex-matched non-SSc subjects from the same population base. Demographics, disease characteristics, cardiovascular risk factors and laboratory tests were abstracted by manual record review. ECGs and Holter ECGs were reviewed to determine the occurrence of any conduction or rhythm abnormalities. The need for cardiac interventions was also abstracted.
Results: 78 incident SSc cases and 156 non-SSc comparators were identified [age 56 years± 15.7, 91% female]. Prevalence of any conduction disorders before SSc diagnosis compared to non-SSc comparators was 15% vs. 7% (p=0.06), and any rhythm disorder was 18% vs. 13% (p=0.33). During a median follow up of 10.5 years in patients with SSc and 13.0 years in non-SSc comparators, conduction disorders developed in 25 SSc patients with a cumulative incidence (ci) of 20.5% (95% CI: 12.4-34.1%) compared to 28 non-SSc patients with ci of 10.4% (95% CI: 6.2-17.4%) (HR: 2.57; 95% CI: 1.48-4.45), while rhythm disorders developed in 27 SSc patients with ci of 27.3% (95% CI: 17.9-41.6%) vs 43 non-SSc patients with ci of 18.0% (95% CI: 12.3-26.4%) (HR: 1.62; 95% CI: 1.00-2.64). (Figure 1)
Conduction disorders in patients with SSc during follow up included: 1st-degree atrioventricular block (AVB) (n=12), 2nd-degree AVB (n=1), 3rd-degree AVB (n=1), right bundle branch block (n=10), left bundle branch block (n=4), bifascicular block (n=6), and prolonged-QT (n=13). Rhythm disorders included: atrial fibrillation (n=10), atrial flutter (n=4), supraventricular tachycardia (n=4), ventricular tachycardia (n=1), and premature ventricular contractions (n=16).
ECG, Holter ECG, and cardiac interventions are presented in Table 1. Pulmonary hypertension (PHT) was the only significant risk factor identified for development of both conduction and rhythm disorders, while current smoking was a significant risk factor for development of rhythm disorders only (Table 2). Conduction and rhythm disorders were associated with increased mortality among patients with SSc (HR=7.60, 95% CI: 3.49-16.55 and HR=4.87, 95% CI: 2.28-10.42, respectively, after adjusting for age, sex and calendar year of diagnosis).
Conclusion: Patients with SSc have a significantly higher prevalence of conduction disorders at disease onset than non-SSc comparators. During the course of their disease, their risk of developing conduction disorders is 2.6-fold, and risk of rhythm disorders is 1.6-fold increased, compared to non-SSc subjects. Our study findings warrant increased vigilance and screening for ECG abnormalities in patients with SSc who have PHT. Underlying mechanisms for this association require further elucidation.
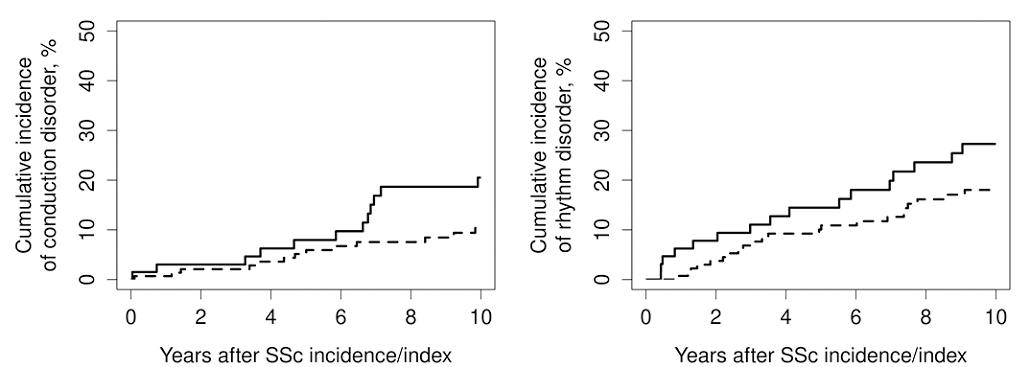 Figure 1: Cumulative incidence of any conduction or any rhythm disorder in systemic sclerosis (SSc) (solid line) vs non-SSc comparators (dashed line).
Figure 1: Cumulative incidence of any conduction or any rhythm disorder in systemic sclerosis (SSc) (solid line) vs non-SSc comparators (dashed line).
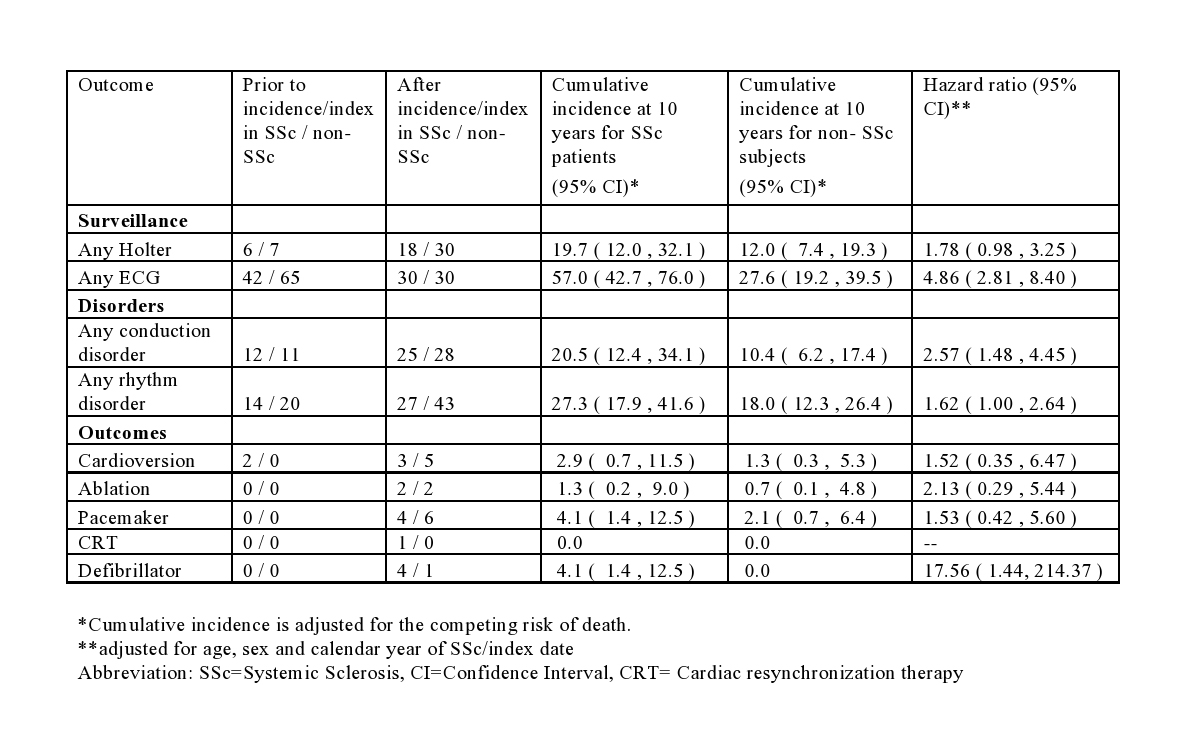 Table 1. Cumulative incidence of conduction and rhythm disorders in 78 patients with systemic sclerosis (SSc) compared with 156 non-SSc comparators
Table 1. Cumulative incidence of conduction and rhythm disorders in 78 patients with systemic sclerosis (SSc) compared with 156 non-SSc comparators
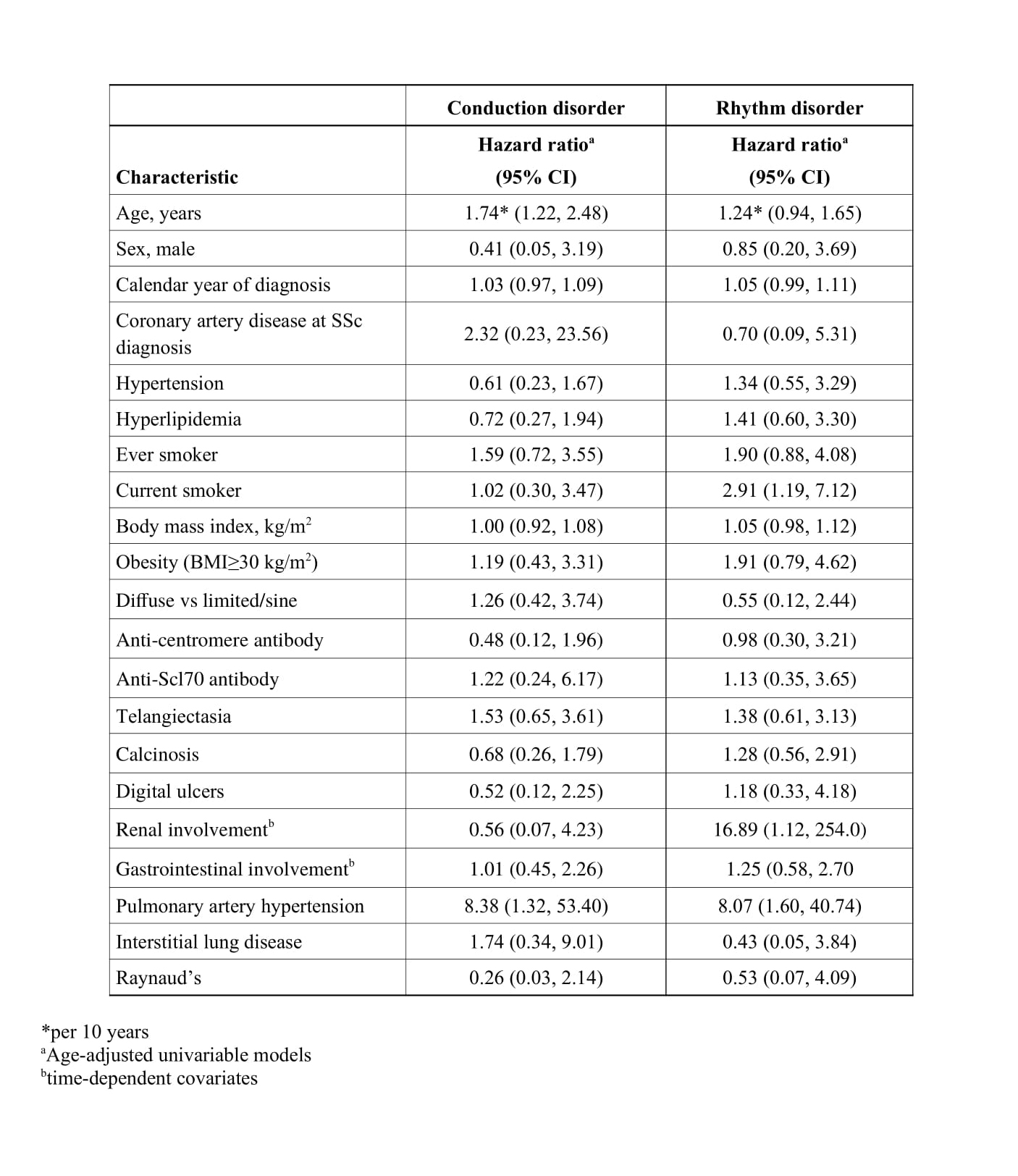 Table 2. Risk factors at systemic sclerosis (SSc) diagnosis for conduction and rhythm disorders in 64 SSc patients without these disorders at disease onset
Table 2. Risk factors at systemic sclerosis (SSc) diagnosis for conduction and rhythm disorders in 64 SSc patients without these disorders at disease onset
To cite this abstract in AMA style:
Radwan Y, Kurmann R, Sandhu A, El-Am E, Crowson C, Matteson E, Osborn T, Warrington K, Mankad R, Makol A. Systemic Sclerosis Portends a Higher Risk of Conduction and Rhythm Disorders at Diagnosis and During Disease Course: Results from a US Population Based Study [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/systemic-sclerosis-portends-a-higher-risk-of-conduction-and-rhythm-disorders-at-diagnosis-and-during-disease-course-results-from-a-us-population-based-study/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/systemic-sclerosis-portends-a-higher-risk-of-conduction-and-rhythm-disorders-at-diagnosis-and-during-disease-course-results-from-a-us-population-based-study/
