Session Information
Date: Monday, November 9, 2020
Session Type: Poster Session D
Session Time: 9:00AM-11:00AM
Background/Purpose: Previous studies from Latin America have shown an association with peripheral arthritis in patients with spondyloarthritis with HLA-B*15 (as opposed to HLA-B27). We aimed to examine sociodemographic and clinical associations along with HLA-B alleles with peripheral arthritis and enthesitis in a longitudinal cohort of AS patients.
Methods: AS patients were derived from the Prospective Study of Outcomes in Ankylosing Spondylitis (PSOAS)/Australo-Anglo-American Spondyloarthritis (TASC) Cohort. All patients met the modified New York Criteria for AS. In addition to a baseline visit (where a history of peripheral arthritis, heel pain and other comorbidities was ascertained), study visits were conducted every 4 to 6 months consisting of an evaluation of spinal mobility, joint swelling/tenderness count, examination of enthesitis (using the UCSF Enthesitis Index) and disease activity (BASDAI, C-reactive protein [CRP], erythrocyte sedimentation rate [ESR]) and functional measures (Bath Ankylosing Spondylitis Functional Index [BASFI], exercise history) and medication use (NSAIDs, anti-TNF blockers, sulfasalazine (SSZ) and methotrexate (MTX). Relative predispositional effects analysis (RPE) was used to adjust for the effect of HLA-B*27 at the HLA-B locus to mask the alleles and analyze the other alleles for associations. Statistics were done using univariable and multivariable analyses for peripheral arthritis and enthesitis in association with clinical, sociodemographic factors, medications and HLA-B alleles.
Results: There were 1076 white AS patients with HLA-B typing included in this analysis. In the case of heel pain by history, at baseline visit affected AS patients were less likely to be taking NSAIDs, but more likely to be exercising >120 minutes a week and to have elevated ESR or CRP at baseline visit, even on multivariable analysis. For those found to have Achilles tendonitis or plantar fasciitis on physical exam, affected individuals were more likely to be female, to have concomitant joint swelling, to be functionally impaired (BASDAI > 40 mm), to be using anti-TNF agents and either MTX or SSZ (Table 1). For those with arthritis on physical exam (defined as joint swelling), again, associations were found with female gender, functional impairment (BASFI) >40 mm), to be exercising < 120 minutes/week, and to be using anti-TNF agents as well as MTX or SSZ (Table 2). Enthesitis at any point in the UCSF Enthesitis Index at any visit was associated with nonwhite ethnicity, concomitant joint swelling, a lower likelihood of regular exercise, and anti TNF use, as well as (marginally) with functioning less well (Table 3). No HLA-B association was found with heel pain, Achilles tendonitis or plantar fasciitis or enthesitis elsewhere, though the association with HLA-B15 persisted with peripheral arthritis.
Conclusion: This association study in a large prospective AS cohort shows a higher prevalence of peripheral musculoskeletal manifestations of AS in women, and the impact on physical function and activity and the concomitant use biologic and nonbiologic DMARDS. Further work is underway examining modifiable factors that might actually predict the future presence of arthritis and enthesitis in these patients.
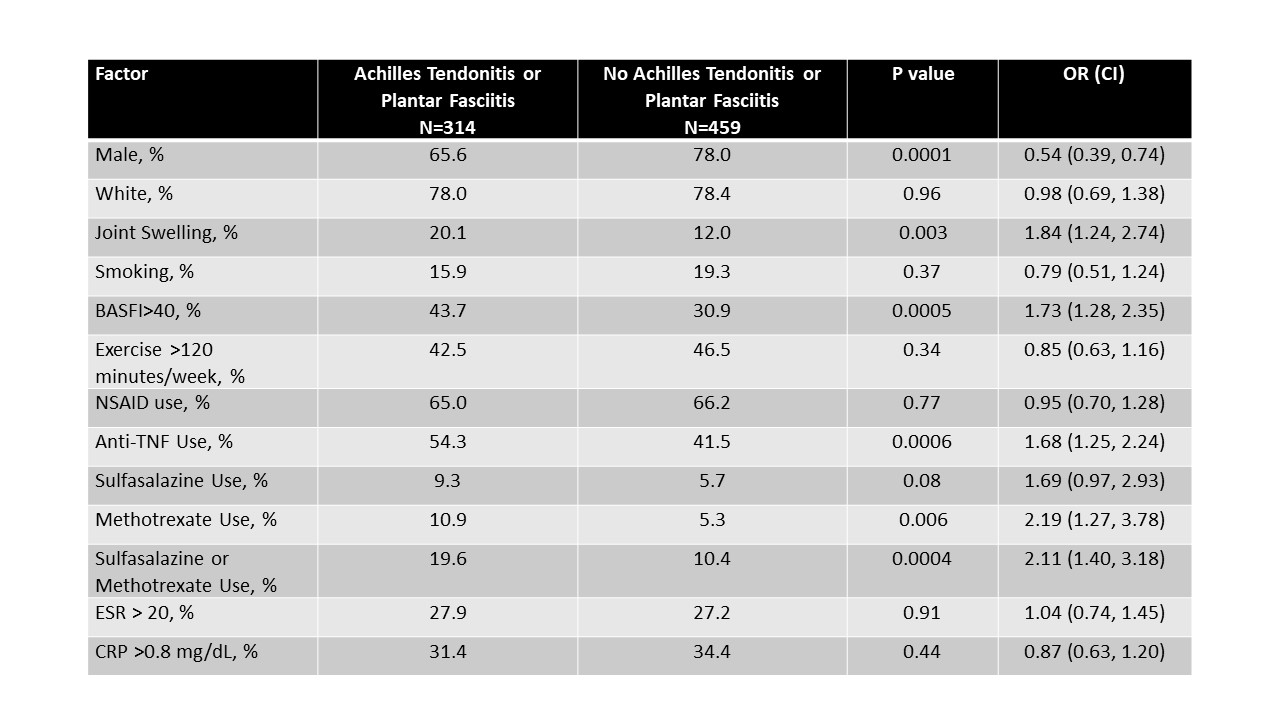 Table 1. Associations of Achilles Tendonitis or Plantar Fasciitis on Clinical Evaluation at any Study Visit
Table 1. Associations of Achilles Tendonitis or Plantar Fasciitis on Clinical Evaluation at any Study Visit
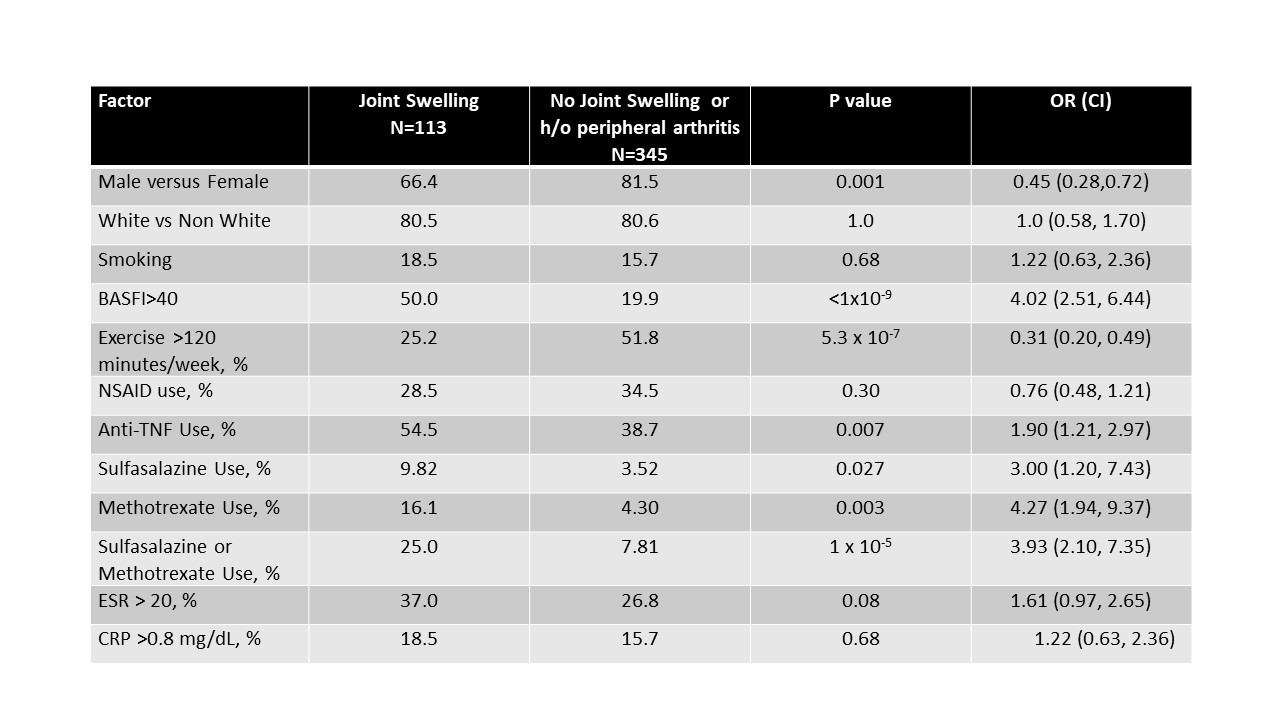 Table 2. Associations of Joint Swelling by Physical Exam At Any Study Visit
Table 2. Associations of Joint Swelling by Physical Exam At Any Study Visit
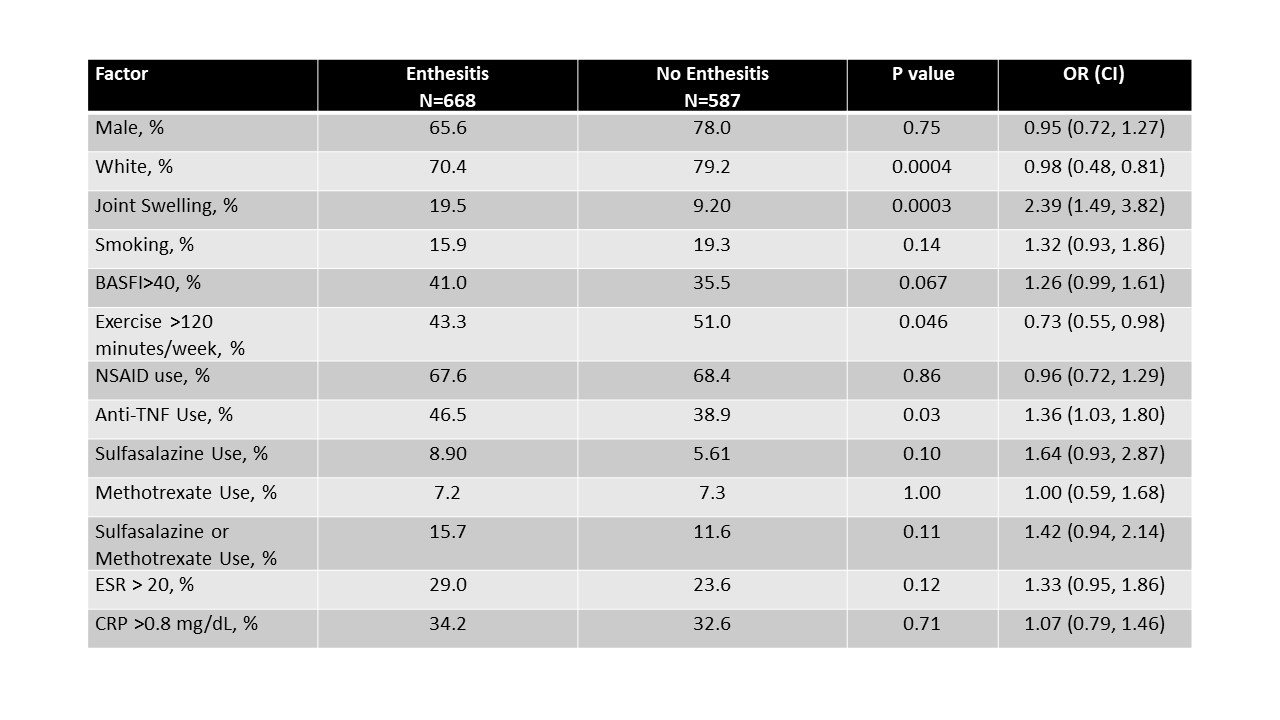 Table 3. Associations of Enthesitis by Physical Exam at any Study Visit
Table 3. Associations of Enthesitis by Physical Exam at any Study Visit
To cite this abstract in AMA style:
Naovarat B, Gensler L, Ward M, Hwang M, Brown M, Tahanan A, Rahbar M, Ishimori M, Weisman M, Reveille J. Relative Associations of Sociodemographic, Clinical and HLA-B Alleles with Enthesitis and Peripheral Arthritis in Patients with Ankylosing Spondylitis [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/relative-associations-of-sociodemographic-clinical-and-hla-b-alleles-with-enthesitis-and-peripheral-arthritis-in-patients-with-ankylosing-spondylitis/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/relative-associations-of-sociodemographic-clinical-and-hla-b-alleles-with-enthesitis-and-peripheral-arthritis-in-patients-with-ankylosing-spondylitis/
