Session Information
Date: Sunday, November 7, 2021
Title: Metabolic & Crystal Arthropathies – Basic & Clinical Science Poster I (0660–0682)
Session Type: Poster Session B
Session Time: 8:30AM-10:30AM
Background/Purpose: Globally, the prevalence of gout is rising in females more than males,1 but data on modifiable risk factors for female gout are scarce. Emerging evidence suggests inflammation may drive the progression from hyperuricemia to clinical gout,2 but the role of extrinsic, modifiable sources of chronic inflammation on gout risk, such as diet, is unknown. Greater dietary inflammatory potential has been independently associated with increased risk of incident cardiovascular disease (CVD)3 and type 2 diabetes (T2D),4 conditions with higher prevalences among females with gout. We prospectively examined the relation between dietary inflammatory potential and gout risk in two large cohorts of US women over 30 years.
Methods: We studied 77,425 women from Nurses Health Study (NHS) (1986-2016) and 93,454 from NHS II (1989-2017) who were free of gout at baseline. Dietary intake and covariates were ascertained by validated questionnaires every 2-4 years, along with new cases of physician-diagnosed gout (every 2 years). Inflammatory potential of diet was evaluated using a food-based, empirical dietary index of inflammatory potential score (EDIP), pre-defined based on circulating levels of IL-6, C-reactive protein, adiponectin, and TNFαR2.5
We assigned an EDIP score for each woman, adjusted for total energy intake, and used Cox proportional hazards models to prospectively examine the relation between quintiles of cumulative average EDIP scores (reflection of habitual diet) and incident gout, adjusting for potential confounders. We further adjusted for body mass index (BMI), a potential causal intermediate, and conducted subgroup analyses.
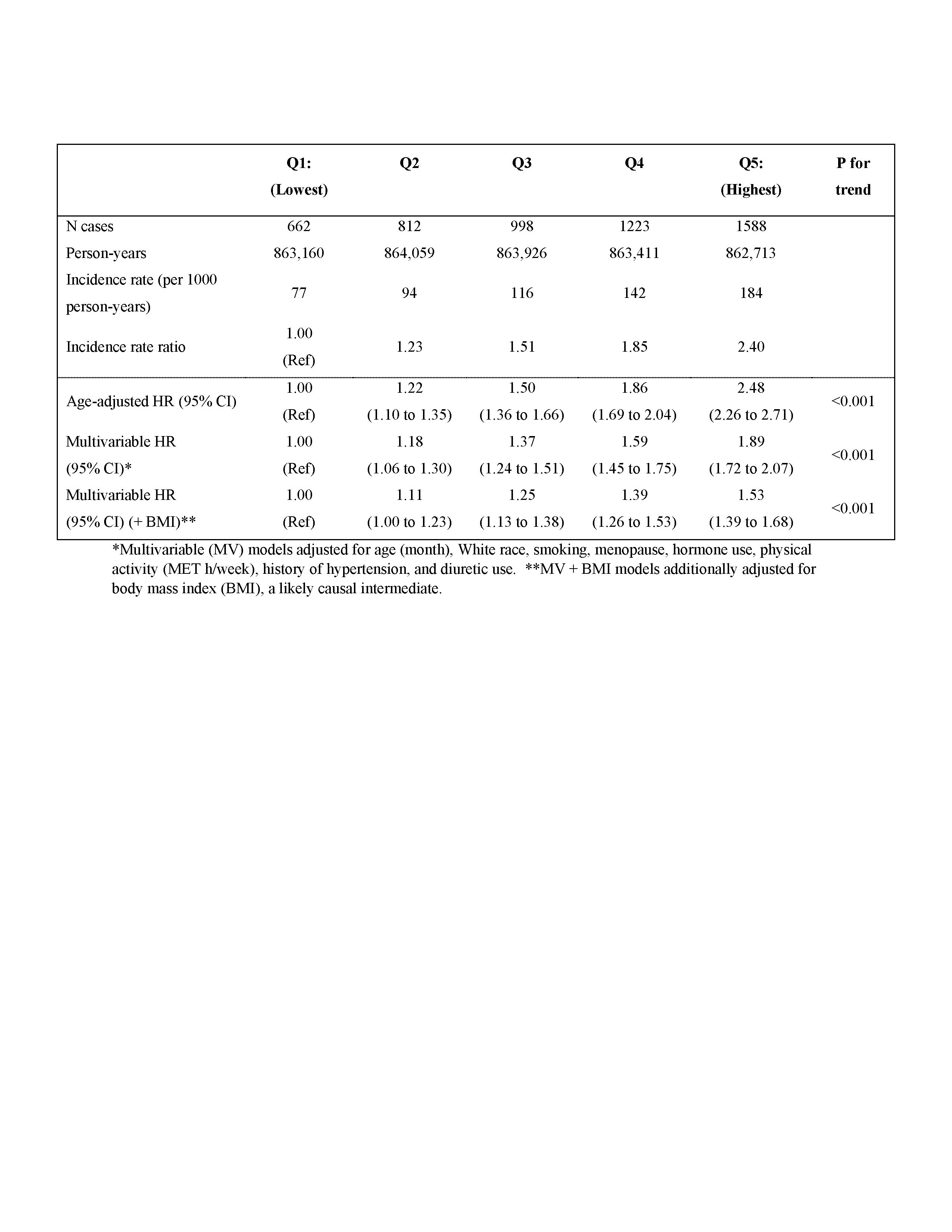
Results: We documented 5,283 cases of incident gout over 4,317,270 person-years, including 3,670 in the NHS (mean age of 50 years at baseline; 49% post-menopausal) and 1,613 in NHS II (mean age 36 years; 3.6% post-menopausal). In pooled multivariable-adjusted (MV) analyses, women in the highest EDIP quintile had nearly two-times greater risk of gout (MV HR 1.9, 95% CI: 1.7 to 2.1) compared to women in the lowest quintile (Table 1). This remained positive with further adjustment for BMI, a likely causal intermediate (MV HR 1.5, 95% CI 1.4 to 1.7).
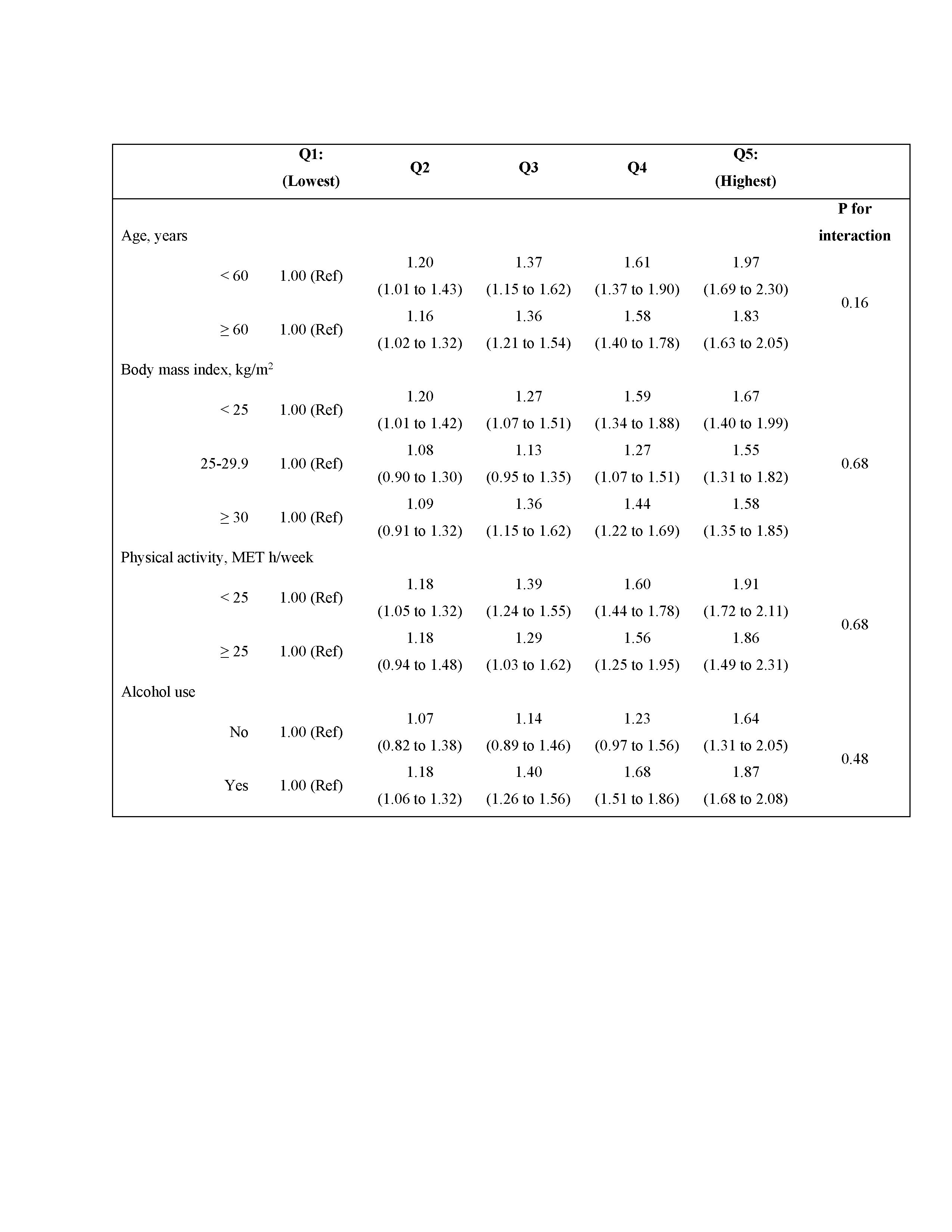
Effects were similar for the older and younger cohorts, with MV HRs of 1.9 (95% CI 1.7 to 2.1, p for trend < 0.001) and 1.9 (1.6 to 2.2, p < 0.001) before BMI adjustment, in the NHS I and II, respectively, and 1.6 (1.4 to 1.7, p < 0.001) and 1.5 (1.3 to 1.8, p < 0.001), respectively, after BMI adjustment. Estimates did not differ significantly across other subgroups.
Conclusion: In these large prospective cohorts of both older and younger women, habitual pro-inflammatory dietary pattern was independently associated with increased risk of incident gout, beyond the pathway through adiposity. Our findings support a role for chronic inflammation in development of female gout, similar to CVD1 and T2D.2 Adhering to a diet with lower inflammatory potential may modulate systemic and metabolic inflammation, potentially reducing gout risk and these life-threatening comorbidities among women.
1Shen Arthrit Rheum (2021); PMID 33760368
2Xia Rheumatology (2020); PMID 31624843
3Li JACC (2020); PMID 32406924<
4Lee Diabetes Care (2020); PMID 32873589
5Tabung; PMID 27358416
To cite this abstract in AMA style:
McCormick N, Yokose C, Lu N, Joshi A, Choi H. Pro-Inflammatory Diet and Increased Risk of Incident Female Gout: 30-Year Prospective Cohort Study of >170,000 Pre- and Post-Menopausal US Women [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/pro-inflammatory-diet-and-increased-risk-of-incident-female-gout-30-year-prospective-cohort-study-of-170000-pre-and-post-menopausal-us-women/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/pro-inflammatory-diet-and-increased-risk-of-incident-female-gout-30-year-prospective-cohort-study-of-170000-pre-and-post-menopausal-us-women/