Session Information
Date: Monday, November 9, 2020
Title: RA – Diagnosis, Manifestations, & Outcomes Poster IV: Lifespan of a Disease
Session Type: Poster Session D
Session Time: 9:00AM-11:00AM
Background/Purpose: Optimal perioperative glucocorticoids (GC) dosing for rheumatoid arthritis (RA) patients on chronic GCs undergoing total joint replacement is unknown. Ideal GC dosing prevents perioperative hypotension while also avoiding the complications associated with higher GC exposure. The purpose of this study was to determine whether preoperative GC exposure or perioperative GC dosing was associated with risk of complications in a large cohort of RA patients undergoing TJA.
Methods: A retrospective chart review was performed to identify patients with RA undergoing TJA at a single, high-volume institution. Glucocorticoid usage was recorded for all patients as well as cumulative perioperative GC dose during hospitalization. GC exposure was assessed by the number of doses, single or multiple, and cumulative amount of GC administered over the hospitalization period (in milligrams). Outcomes of interest included incidence of perioperative hypotension and inpatient complications (hyperglycemia, defined as blood glucose level > 180mg/dL, local or systemic infection, and cardiovascular events). Multivariable logistic regression was performed to evaluate the impact of GC dosing on these adverse events.
Results: Four hundred and thirty two RA patients undergoing TJA were included with 233 (54%) undergoing TKA. Mean age was 64±12 years and 78% were women. One hundred and thirty (30%) RA TJA patients were on chronic GC treatment (mean daily dose 7±4mg) and median cumulative perioperative GC dose was 37mg [IQR 27, 57]. Cumulative inpatient dose of GC was not associated with risk for perioperative hypotension during the hospitalization [unadjusted OR 1.00 (0.99-1.01) p=0.66]. Patients who received multiple doses had more post-operative adverse events compared to those who received single GC doses. Multivariable logistic regression adjusting for age, BMI and Charlson Comorbidity Index, showed patients with higher cumulative GC dose had higher risk for short-term complications with every 10 mg increase in GC dosing increasing inpatient complication risk by 8.4%, (p=0.02).
Conclusion: This study of 432 RA patients undergoing TJA found a 32% incidence of chronic preoperative GC usage. GC dosing during the intra- and early post-operative period was not associated with risk of hypotension. However, patients with higher GC exposure were more likely to have hyperglycemia and catheter-associated urinary tract infection (CAUTI). These findings suggest lower GC dosing does not increase risk of hypotensive perioperative events and avoids the increased risk of inpatient complications associated with high GC dosing regiments. Further research is needed to determine the optimal perioperative regimen for patients with RA undergoing arthroplasty.
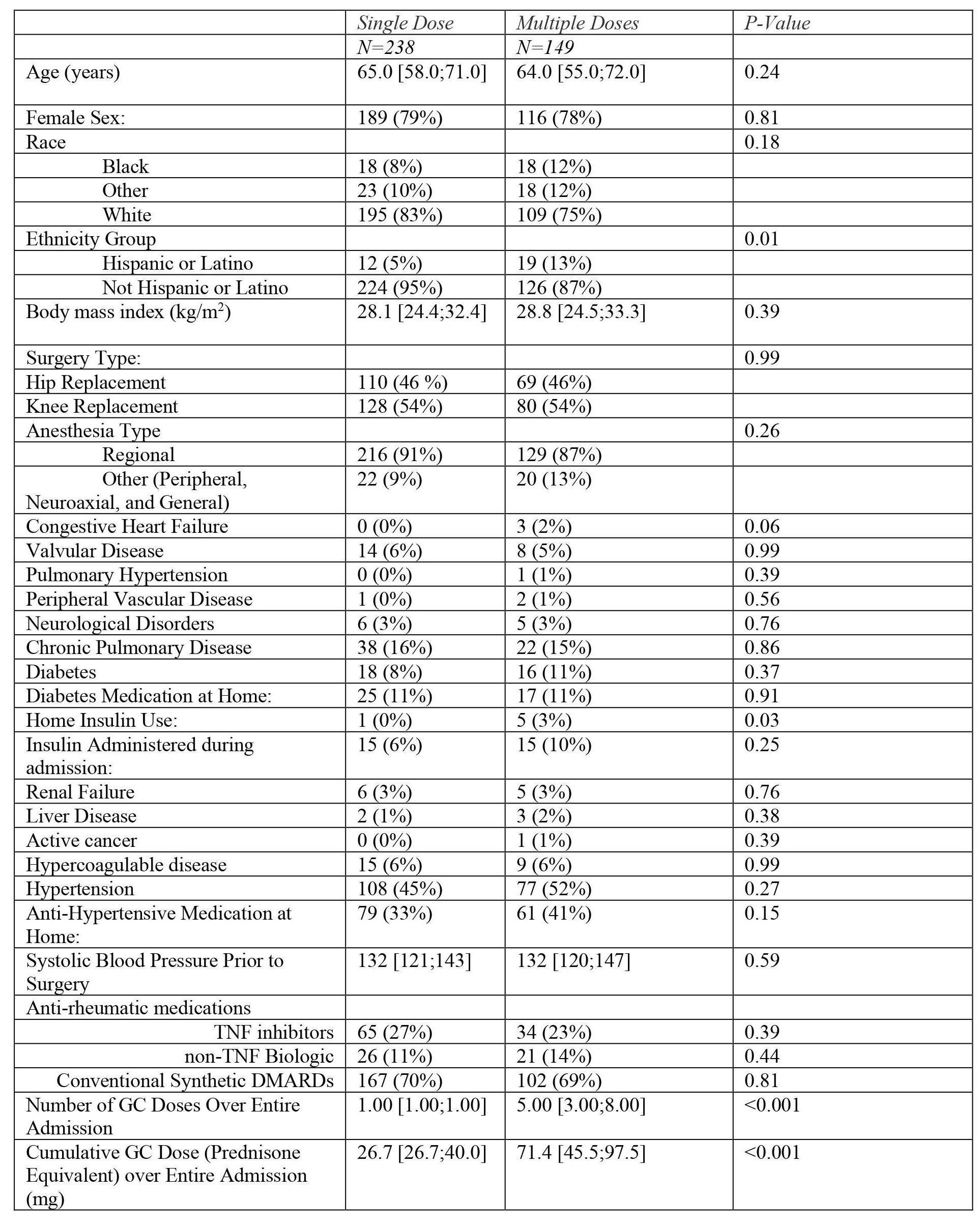 Baseline characteristics of patients according to perioperative GC exposure.
Baseline characteristics of patients according to perioperative GC exposure.
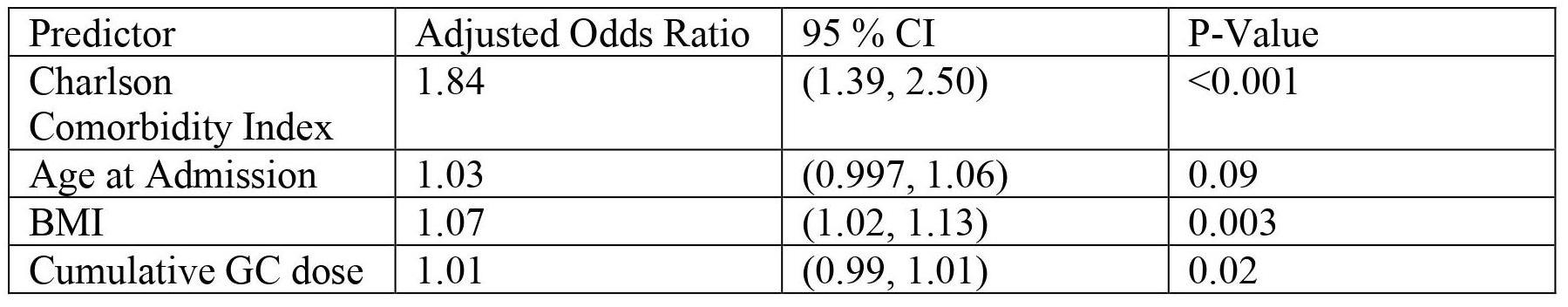 Multivariable regression: association of cumulative GC dose and patient characteristics with complications following arthroplasty
Multivariable regression: association of cumulative GC dose and patient characteristics with complications following arthroplasty
To cite this abstract in AMA style:
Chukir T, Goodman S, Tornberg H, Do H, Thomas C, Sigmund A, Sculco P, Mehta B, Russell L, Figgie M, Stein E. Perioperative Steroids in Rheumatoid Arthritis Patients Having Total Joint Replacements: Help or Harm? [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/perioperative-steroids-in-rheumatoid-arthritis-patients-having-total-joint-replacements-help-or-harm/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/perioperative-steroids-in-rheumatoid-arthritis-patients-having-total-joint-replacements-help-or-harm/
