Session Information
Date: Sunday, November 8, 2020
Title: RA – Diagnosis, Manifestations, & Outcomes Poster III: Cardiopulmonary Aspects
Session Type: Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: A novel risk prediction score combines serum biomarkers from the multi-biomarker disease activity (MBDA) test with clinical information to predict 3-year risk for a cardiovascular disease (CVD) event in RA patients. The CVD risk prediction score was developed and internally validated in a cohort of patients from the Medicare database. We have now examined the performance of the score in subgroups of patients of interest to practicing rheumatologists.
Methods: A cohort of RA patients age ≥40 with ≥1 RA diagnosis from a rheumatologist, without history of malignancy, past myocardial infarction (MI) or stroke was created by linking Medicare administrative data (2006-2016) to MBDA test results obtained during routine care. The cohort was randomly split 2:1 for training/internal validation. The composite CV outcome was MI, stroke or CV death occurring within 3 years. Candidate predictors for inclusion in model training were selected from traditional CV risk factors, RA-related factors and the MBDA score and its 12 biomarkers (log-transformed). Training was conducted using backward elimination. The final risk score algorithm included: age, diabetes, hypertension, smoking, prior history of CV disease, adjusted MBDA score, TNF-R1, MMP-3 and leptin. In the internal validation dataset this MBDA-based CV risk score was evaluated by: 1) Kaplan-Meier (KM) curves of observed event rates over time for patients grouped by the test into the low, borderline, intermediate or high categories of predicted risk and 2) goodness-of-fit plots showing the relationship between observed event rates and predicted risk for patients grouped by CV event-based deciles (based on Kaplan-Meier estimates with 95% CI).
Results: 30,751 RA patients were linked to MBDA test results and eligible for analysis. Mean (SD) age was 68.7 (9.5) years (23.4% < 65 years); 82% were women; mean MBDA score was 41 (14). Comorbidities were frequent (diabetes 39%, hypertension 78%, smoking 24%, history of high-risk CV condition 37%). RA-related features included use of glucocorticoids by 58%, methotrexate 60%, TNFi 33% and other biologics 16%. Median (IQR) 3-year CV risk predicted by the test was 3.4% (2.1%, 5.6%). Based on extrapolation to 10-year risk, 19.6% of patients would be considered low/borderline, 52.2% intermediate, and 28.2% high risk per ACC/AHA 2018 guidelines. In the validation dataset, CVD event rates increased the most over time for patients assigned by the test to categories of greatest CVD risk (Figure 1). The relationship between predicted CVD risk and observed CVD events demonstrated a good fit in the validation dataset, both overall and among patients grouped by sex, age, diabetes, prior CVD history, statin use, initiation of change of a biologic/targeted therapy and category of MBDA score (Figures 2 and 3).
Conclusion: The MBDA-based CVD risk prediction score, which combines biomarker and clinical variables, discriminated 3-year risk for a CVD event in RA patients. Predicted risk had good fit relative to observed CVD event rates, both overall and in several patient subgroups, including males/females, diabetics, statin users and patients with different levels of disease activity based on the MBDA score.
 Figure 1. Kaplan-Meier plot for CVD event occurrence by the risk category predicted with the MBDA-based CVD risk score model, validation data (N=10,275)
Figure 1. Kaplan-Meier plot for CVD event occurrence by the risk category predicted with the MBDA-based CVD risk score model, validation data (N=10,275)
 Figure 2. Goodness-of-fit Plots for Demographic Subgroups
Figure 2. Goodness-of-fit Plots for Demographic Subgroups
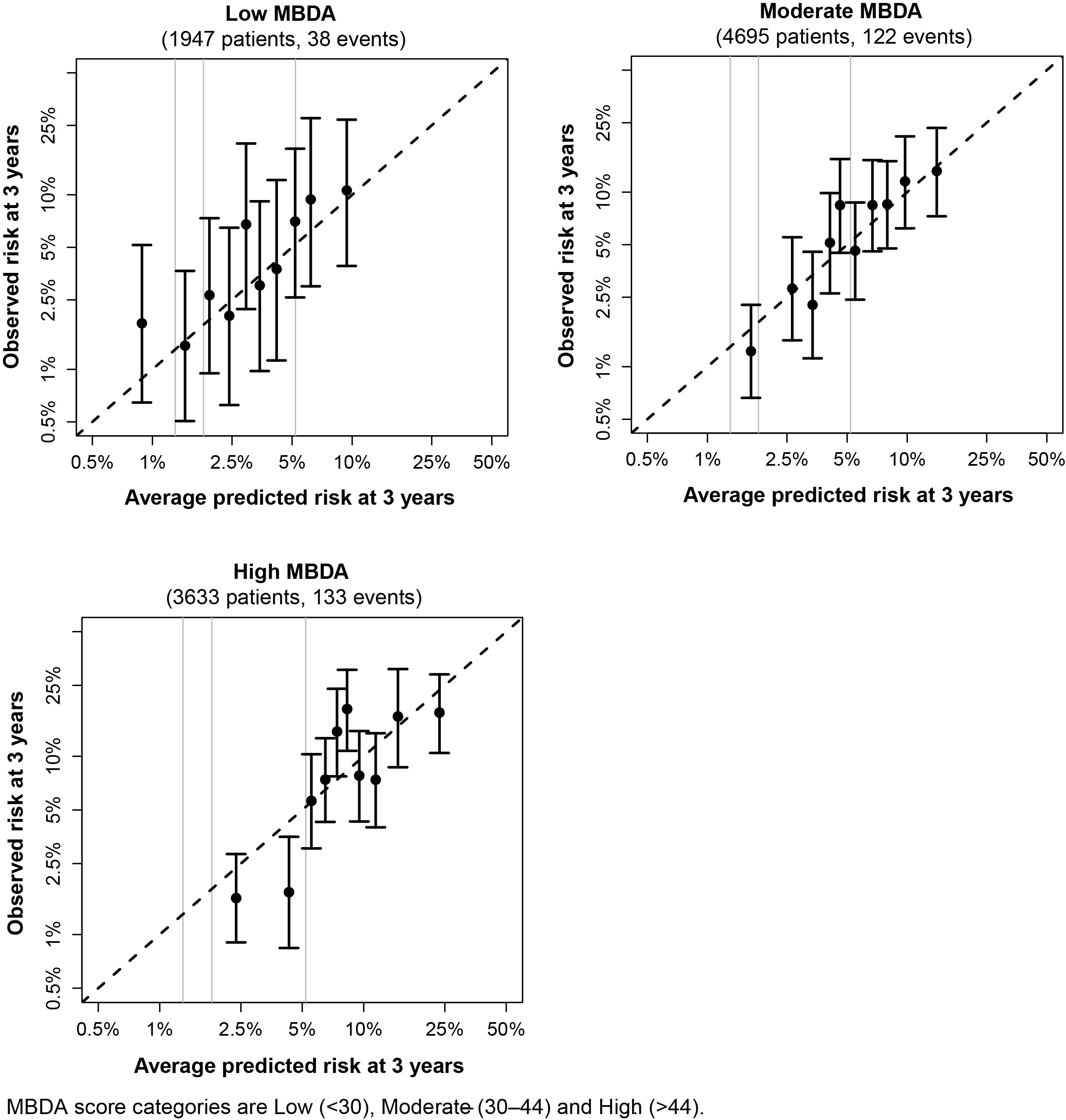 Figure 3. Goodness-of-fit Plots for Disease Activity Subgroups, based on Category of MBDA Score
Figure 3. Goodness-of-fit Plots for Disease Activity Subgroups, based on Category of MBDA Score
To cite this abstract in AMA style:
Curtis J, Xie F, Crowson C, Sasso E, Hitraya E, Chin C, Bamford R, Ben-Shachar R, Gutin A, Flake D, Mabey B, Lanchbury J. Performance of the MBDA-based CVD Risk Score in RA Patient Groups of Clinical Interest [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/performance-of-the-mbda-based-cvd-risk-score-in-ra-patient-groups-of-clinical-interest/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/performance-of-the-mbda-based-cvd-risk-score-in-ra-patient-groups-of-clinical-interest/
