Session Information
Session Type: Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose: Total knee replacement (TKR) is considered an effective knee OA treatment and is a commonly performed orthopedic procedure that relieves pain and improves function and quality of life.1 However, up to 20% of patients may not achieve good clinical outcomes.2 Also, comorbidities and patient factors may limit the ability to safely perform the TKR. The objective of this was to identify the percentage and distribution of TKR surgical candidates across specialties (rheumatologists [RH], orthopedic surgeons [OS], sports medicine [SM] physicians, and pain specialists [PS]) to gain insight into patient characteristics influencing TKR candidacy.
Methods: Board-certified physicians with >2 years in practice and >10 knee OA patients per week participated in an interview about their two most recent knee OA patients. Interviews were conducted from March to April 2019 and assessed demographics, referral patterns, comorbidities, time to treatment, imaging use, candidacy for TKR, and reasons for noncandidacy. Multiple reasons for TKR noncandidacy per patients were allowed. Since no patient-identifying information was included, this project was exempt from IRB review and HIPAA consent. As this study was designed to assess multiple characteristics and associated effect modifications, a confidence level of 90% was used.3
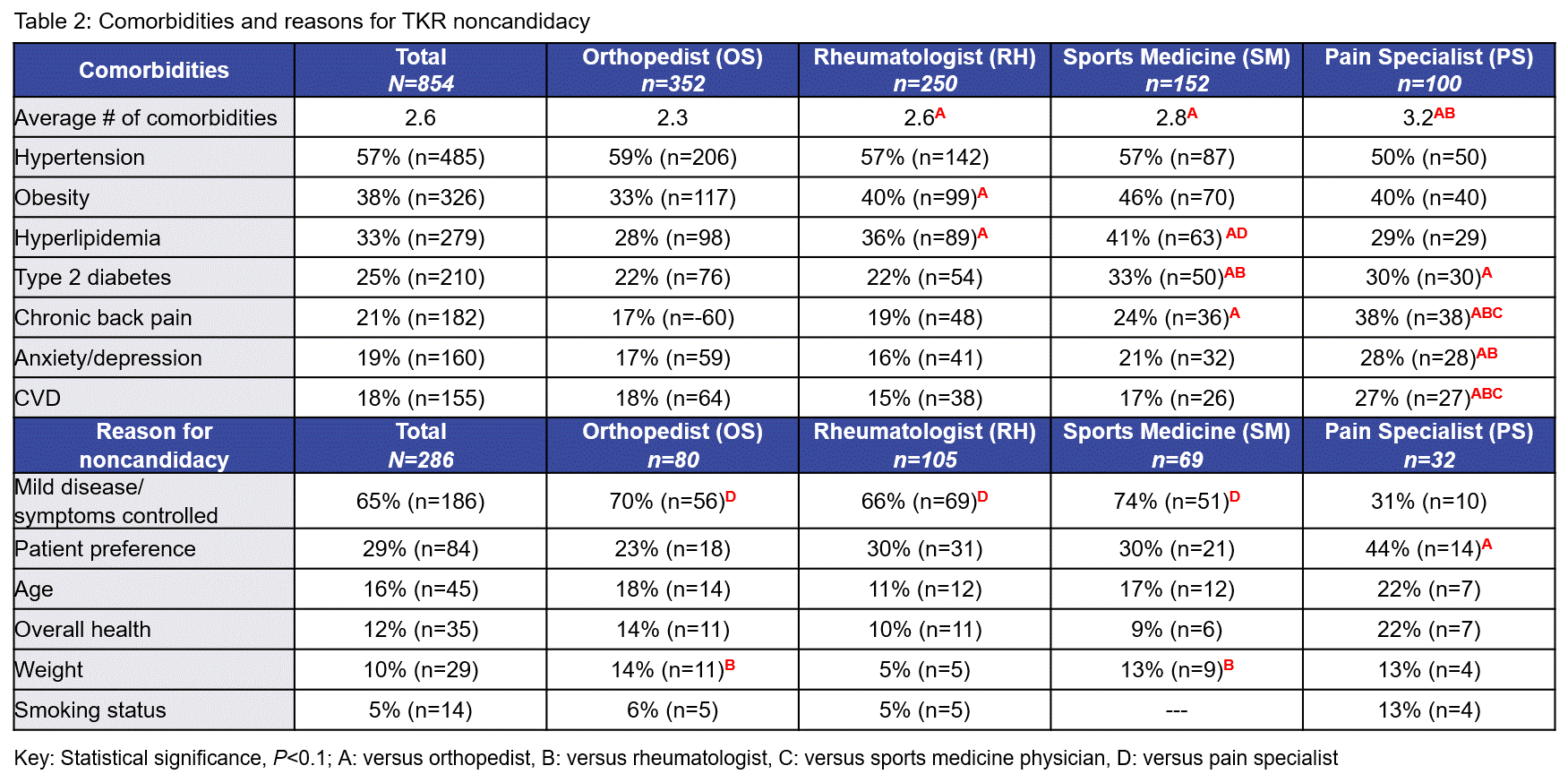
Results: Overall, the mean age of knee OA patients was 65 years (range: 63 years for SM patients to 66 years for PS patients) (Table 1). Primary care physicians were the most common referrers to RH (83%) and the reported mean time from symptom onset to diagnosis was 3.4 years (longest in RH patients; 4.5 years). Overall, the mean number of comorbidities was 2.6, with the most common being hypertension and obesity (Table 2). The mean pain score was 5.5 (0–10 NRS) and 58% of RH patients had moderate pain. RH saw predominantly KL grade 3 (55.6%) patients whereas OS saw more KL grade 4 (45.3%) patients. TKR candidacy was assessed for 779 patients; approximately half of these were identified as future surgical candidates, with 38% projected to undergo TKR within the next 12 months. Overall, of 286 (37%) identified as TKR noncandidates, 65% had mild disease or well-controlled symptoms. Among RH noncandidates (42%, n=105), additional reasons for TKR exclusion included patient preference (30%), age (11%), overall health (10%), weight (5%), and smoking habits (5%) (Table 2). Limitations to this study included potential selection bias, confounding by risk factors, inability to show causation, small n’s, missing data, and pre-COVID-19 proposed timeline for TKR.
Conclusion: In this observational chart review, of the 42% of TKR noncandidates who were RH patients, several patient factors were identified as reasons for exclusion (patient preference, age, overall health, and lifestyle choices [such as smoking]). Patient preference contributed the largest impact (30%) and other influences were well characterized, suggesting further investigation of patient-focused factors that impact decision-making regarding TKR is warranted.
References:
- NEJM 2015; 373:1597-1606
- EFORT Open Rev. 2018;3(8):461‐470
- J Thorac Dis. 2016 Sep; 8(9): E928–E931
To cite this abstract in AMA style:
Bedenbaugh A, Lee V, Oderda G, Kennedy S, Tambiah J, Brixner D, McAlindon T. Patient Characteristics and Factors Affecting Decision-Making Regarding Total Knee Replacement by Different Types of Physicians Treating Patients with Knee OA [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/patient-characteristics-and-factors-affecting-decision-making-regarding-total-knee-replacement-by-different-types-of-physicians-treating-patients-with-knee-oa/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/patient-characteristics-and-factors-affecting-decision-making-regarding-total-knee-replacement-by-different-types-of-physicians-treating-patients-with-knee-oa/