Session Information
Date: Sunday, November 8, 2020
Title: RA – Diagnosis, Manifestations, & Outcomes Poster III: Cardiopulmonary Aspects
Session Type: Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: Rheumatoid Arthritis (RA) patients are at nearly 50% increased risk of heart failure (HF) compared to non-RA patients, despite adjusting for the presence of coronary artery disease, suggesting that RA associated inflammation is an independent contributor to HF. Higher prevalence of diastolic dysfunction as well as significantly higher rate of change in key diastolic parameters (mitral A wave velocity, mitral E/A, and Left Atrial Volume Index (LAVI)) were demonstrated in RA patients without clinical HF vs. controls. While significant associations between baseline patient reported RA characteristics and adverse changes in diastolic parameters have been demonstrated, an association between RA disease activity against baseline and/or change in diastolic function has not yet been elucidated.
Methods: RA patients (N=163) without clinical cardiovascular disease were enrolled and followed over a 3-to 6-year time period. At baseline, patients underwent echocardiography and assessment of cardiovascular and RA associated disease risk factors. A subset (n=60) underwent repeat echocardiography on a subsequent visit 3-6 years later. Diastolic function was assessed according to 2015 guidelines. Annualized rate of change for each chosen diastolic outcome variable (E/e’, E/A, tricuspid regurgitation (TR) velocity, LAVI, Deceleration Time (DT) of E wave) was calculated. Multivariable regression models were used to adjust for biologically plausible confounders identified from univariate regressions.
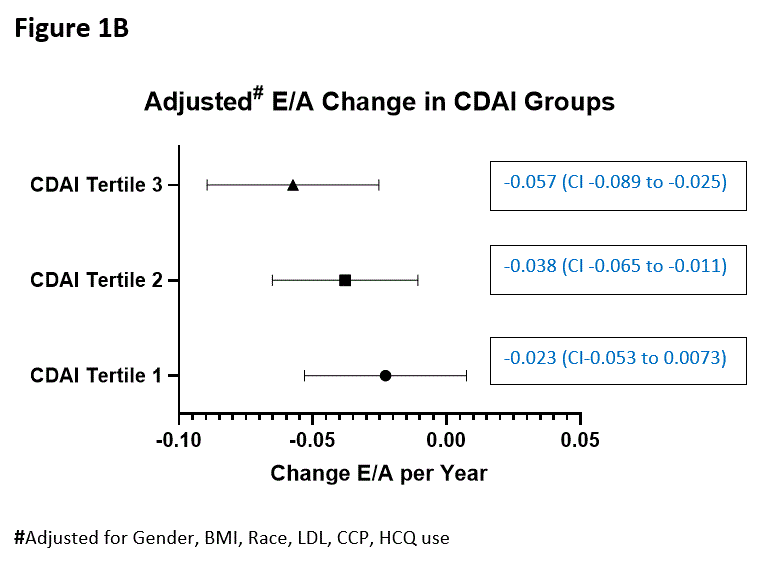
Results: At least one abnormal diastolic parameter was observed in 59% of the cohort at baseline, and in 69% at follow-up. Significant decline in E velocity (p=0.01), lateral and septal e’ velocity (p=0.001 and p=0.05, respectively) and E/A (p=0.03) were observed (Table 1). After adjustment for confounders, baseline E/e’ was 0.363 units higher per square root Clinical Disease Activity Index (CDAI) (p=0.002) and 0.539 units higher per unit of DAS28CRP (p=0.005). Additionally, E/e’ increased by 0.174 units/year per square root CDAI (p=0.026) in adjusted models. As CDAI increased in tertile, greater increase in E/e’ per year was observed (See Figure 1A). Moreover, E/A decreased by 0.014 units/year per square root CDAI (p=0.029) in a final adjusted model. As CDAI increased in tertile, greater decline in E/A per year was observed (See Figure 1B).
Conclusion: We report significant adverse changes over time in 2 key diastolic parameters (increasing E/e’ and decreasing E/A) in association with higher baseline disease activity, while adjusting for a number of potential confounders. Whether DMARD treatment and subsequent reduction of disease activity impacts baseline and follow up left ventricular structure and function in RA should be elaborated further in prospective/controlled studies.
To cite this abstract in AMA style:
Park E, Ito K, Depender C, Giles J, Bathon J. In a Prospective RA Cohort, Higher Baseline Disease Activity Is an Independent Predictor of Decline in Left Ventricular Diastolic Function [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/in-a-prospective-ra-cohort-higher-baseline-disease-activity-is-an-independent-predictor-of-decline-in-left-ventricular-diastolic-function/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/in-a-prospective-ra-cohort-higher-baseline-disease-activity-is-an-independent-predictor-of-decline-in-left-ventricular-diastolic-function/