Session Information
Date: Monday, November 11, 2019
Title: Systemic Sclerosis & Related Disorders – Basic Science Poster
Session Type: Poster Session (Monday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Chronic inflammation may modulate the balance of classical, intermediate and non-classical monocyte subsets (defined by CD14/CD16 expression)1. Monocytes are heterogeneous and subsets can be further delineated by examining expression of other cellular markers such as CD163, a haemoglobin-scavenging receptor which is associated with resolving inflammation and fibrosis. Systemic sclerosis (SSc) is a chronic autoimmune disease and a prototype for studying how the immune system regulates fibrosis2. The aim of this study is to characterise monocyte/macrophage subsets, and their function in SSc.
Methods: Blood samples from healthy donors and SSc patients were collected for serum, leukocyte and monocyte isolation. Leukocytes were stained with CD14, CD16 and CD163 antibodies for FACS analysis. Monocytes were isolated by negative selection and Ficoll separation of blood and cultured for 7 days into macrophages. Soluble CD163 levels were measured by ELISA. Macrophage supernatants were applied to scratch-wounded healthy skin fibroblast monolayers and fibroblast-populated collagen gels, to assess their effect on fibroblast migration and contraction, respectively. Mann-Whitney U tests, 2-tailed unpaired t-tests, Spearman’s Rank and linear regression were used for statistical analysis.
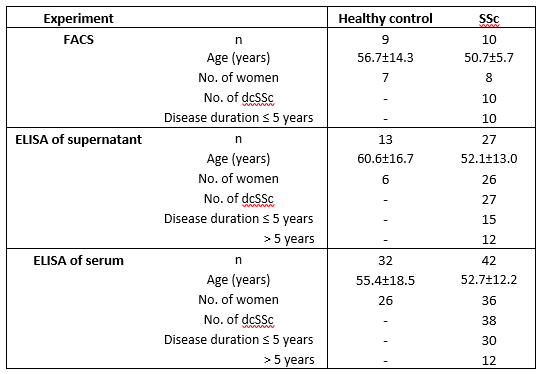
Results: In our cohort of SSc patients (Table 1), we found two-fold more circulating CD163+CD14loCD16hi non-classical monocytes (6.02±0.8 x103 cells/mL), than in healthy controls (2.69±1.0 x103 cells/mL), p=0.026. Accordingly, we observed significantly higher levels of soluble CD163 in SSc sera (682ng/mL) than in healthy control sera (587ng/mL), Mann Whitney U=413, p=0.010. Higher levels of soluble CD163/total protein were detected in supernatants of SSc macrophage cultures (9.96 x10-3) compared to those of healthy controls (7.76 x10-3), Mann Whitney U=77, p=0.005. There were no associations between sera or supernatant CD163 levels and clinical parameters such as disease duration, modified Rodnan skin score and lung fibrosis.
Fibroblasts treated with SSc macrophage media migrated faster (n=2, rate of closure 2.9% wound area/hour, R2=0.90) into the scratch wound area of monolayers than those treated with healthy control media (n=2, rate of closure 1.7% wound area/hour, R2=0.82), p=0.017. SSc macrophage supernatant promoted fibroblast contraction as indicated by the lower weight of fibroblast-populated collagen gels cultured in SSc macrophage supernatant (n=5, 110.7±8.6 mg) compared to those in healthy control supernatant (n=2, 153.6±6.8 mg), p=0.035.
Conclusion: Our data suggests that the increased frequency of systemic CD163+ non-classical monocytes corresponds with upregulation of soluble CD163 in SSc. Parallel to this, the paracrine macrophage-fibroblast crosstalk is supportive of the micro-environment in promoting fibrosis. Thus, modulating both the systemic and local effects of non-classical monocytes mediated by CD163 may have therapeutic relevance in targeting fibrosis in SSc.
References:
- Ziegler-Heitbrock L et al, Blood. 2010;116(16):e74-80.
- Toledo DM, Pioli PA. Curr Rheumatol Rep. 2019;21(7):31.
To cite this abstract in AMA style:
Tam A, Reinke-Breen L, Trujillo G, Xu S, Denton C, Abraham D, Jarai G, Ong V. Identification of Distinct Pro-Fibrotic Monocyte and Macrophage Subsets in Systemic Sclerosis [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/identification-of-distinct-pro-fibrotic-monocyte-and-macrophage-subsets-in-systemic-sclerosis/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/identification-of-distinct-pro-fibrotic-monocyte-and-macrophage-subsets-in-systemic-sclerosis/