Session Information
Date: Sunday, October 21, 2018
Title: Systemic Lupus Erythematosus – Clinical Poster I: Clinical Manifestations and Comorbidity
Session Type: ACR Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: Tuberculosis (TB) has complex interplay with systemic lupus erythematosus (SLE). In addition, SLE, corticosteroid, and immunosuppressants are associated with TB infection. However, the prognostic factors of TB in patients with SLE have not been fully investigated. The aim of this study was to evaluate the effects of corticosteroid and immunosuppresants on the prognosis of TB in SLE patients.
Methods: This retrospective cohort study was conducted by reviewing the medical records between January 1, 2006 and December 31, 2016. SLE patients with TB infection were screened via ICD codes. Only those fulfilled the ACR 1997 classification criteria of SLE and presented with microbiological or typical histological evidence of TB were enrolled. Patients with history of organ transplantation, HIV, incomplete history of immunosuppressive agents, and those without taking anti-TB regimen were excluded. The primary outcome was mortality during TB treatment.
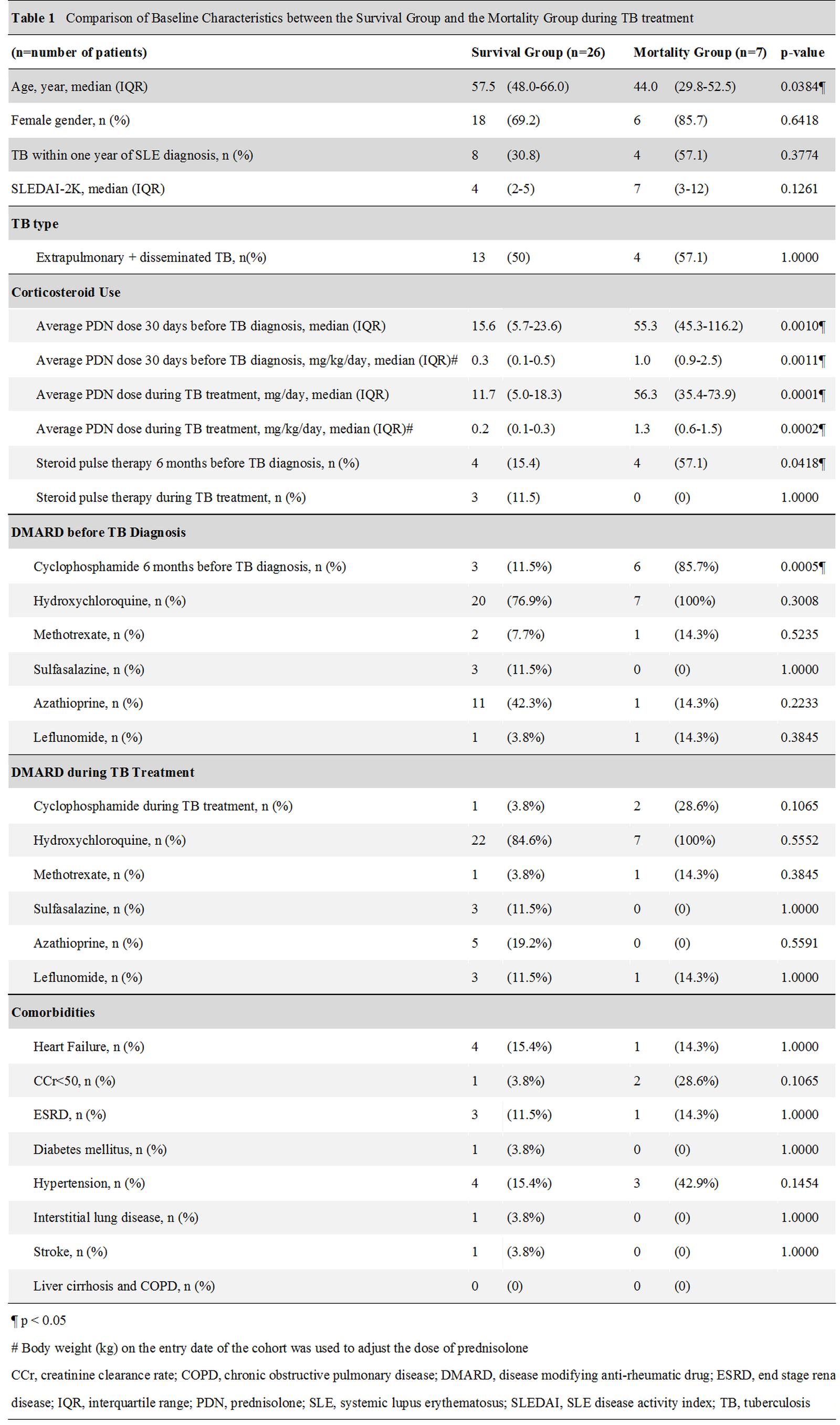
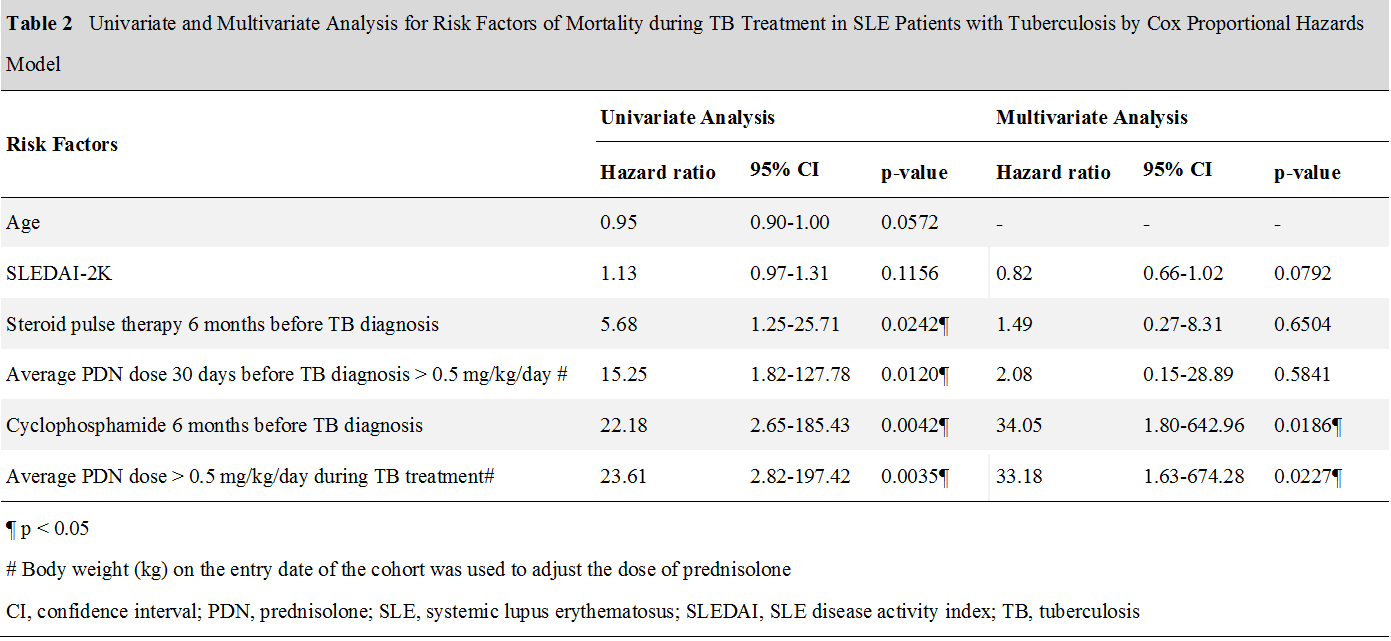
Results: 5388 patients with ICD codes of SLE were screened, and 88 patients with ICD codes of TB were identified. After review of the medical records, 32 patients and 33 episodes fulfilled the inclusion criteria and were enrolled. The mortality during TB treatment was 21.2% (7/33). In comparison with the patients in the survival group (n=26), the patients in the mortality group (n=7) had younger age at diagnosis (44.0 vs 57.5, p=0.0384), higher average prednisolone dose 30 days before TB diagnosis (55.3 mg/day vs 15.6 mg/day, p=0.0010), higher average prednisolone dose during TB treatment (56.3 mg/day vs 11.7 mg/day, p=0.0001), more steroid pulse therapy 6 months before the TB diagnosis (4/7, 57.1% vs 4/26, 15.4%. p=0.0418), and more cyclophosphamide pulse therapy 6 months before the TB diagnosis (6/7, 85.7% vs 3/26, 11.5%. p=0.0005). There was no significant difference between the two groups in SLEDAI-2K (7 vs 4, p=0.1261). The multivariate analysis by Cox proportional hazard model revealed that average dose of prednisolone more than 0.5 mg/kg/day during TB treatment (HR 33.18, 95% CI 1.63-674.28, p=0.0227) and cyclophosphamide 6 months before the diagnosis of TB (HR 34.05, 95% CI 1.80-642.96, p=0.0186) were associated with higher mortality during TB treatment.
Conclusion: This retrospective cohort study finds that the mortality during TB treatment correlates with prednisolone dose during TB treatment and cyclophosphamide use 6 months before TB diagnosis.
To cite this abstract in AMA style:
Cheng CF, Lu CH, Hsieh SC, Li KJ. Higher Prednisolone Dose during Treatment of Tuberculosis Correlates with Mortality during Tuberculosis Treatment in Systemic Lupus Erythematosus Patients: A Retrospective Cohort Study [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/higher-prednisolone-dose-during-treatment-of-tuberculosis-correlates-with-mortality-during-tuberculosis-treatment-in-systemic-lupus-erythematosus-patients-a-retrospective-cohort-study/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/higher-prednisolone-dose-during-treatment-of-tuberculosis-correlates-with-mortality-during-tuberculosis-treatment-in-systemic-lupus-erythematosus-patients-a-retrospective-cohort-study/