Session Information
Date: Sunday, November 7, 2021
Title: RA – Diagnosis, Manifestations, & Outcomes Poster II: Miscellaneous Aspects of RA (0786–0812)
Session Type: Poster Session B
Session Time: 8:30AM-10:30AM
Background/Purpose: The concept of difficult-to-treat rheumatoid arthritis (D2T RA) has emerged as the greatest unmet need in recent years. We have investigated the clinical characteristics and the contributing factors toward the outcome in patients with D2T RA in the real world setting using a multicenter RA ultrasound prospective observational cohort study.
Methods: We enrolled 366 RA patients from a multicenter prospective ultrasound observational cohort study [KUDOS study] who received biologic or targeted synthetic disease-modifying antirheumatic drugs (b/tsDMARDs) therapy. We evaluated the therapeutic efficacy by the patients’ clinical disease activity scores and musculoskeletal ultrasound (MSUS) scores (sum of semi-quantitative evaluation from 22 joints from both wrist and finger joints) every 3 months during 12 months. We defined a D2T RA as a patient with (1) failure of ≥2 b/tsDMARDs and (2) at least moderate disease activity (DAS28-ESR >3.2 or CDAI >10) or inability to taper glucocorticoid treatment (≥7.5 mg/ day prednisone) at baseline. First, we compared characteristics between D2T RA and non-D2T RA. Second, we attempted to identify any variables that were independently contributing factors of the good outcome defined as CDAI remission and treatment continuation at 12 months from the patients’ baseline characteristics and types of b/tsDMARD mode of action by performing a multivariate logistic regression analysis.
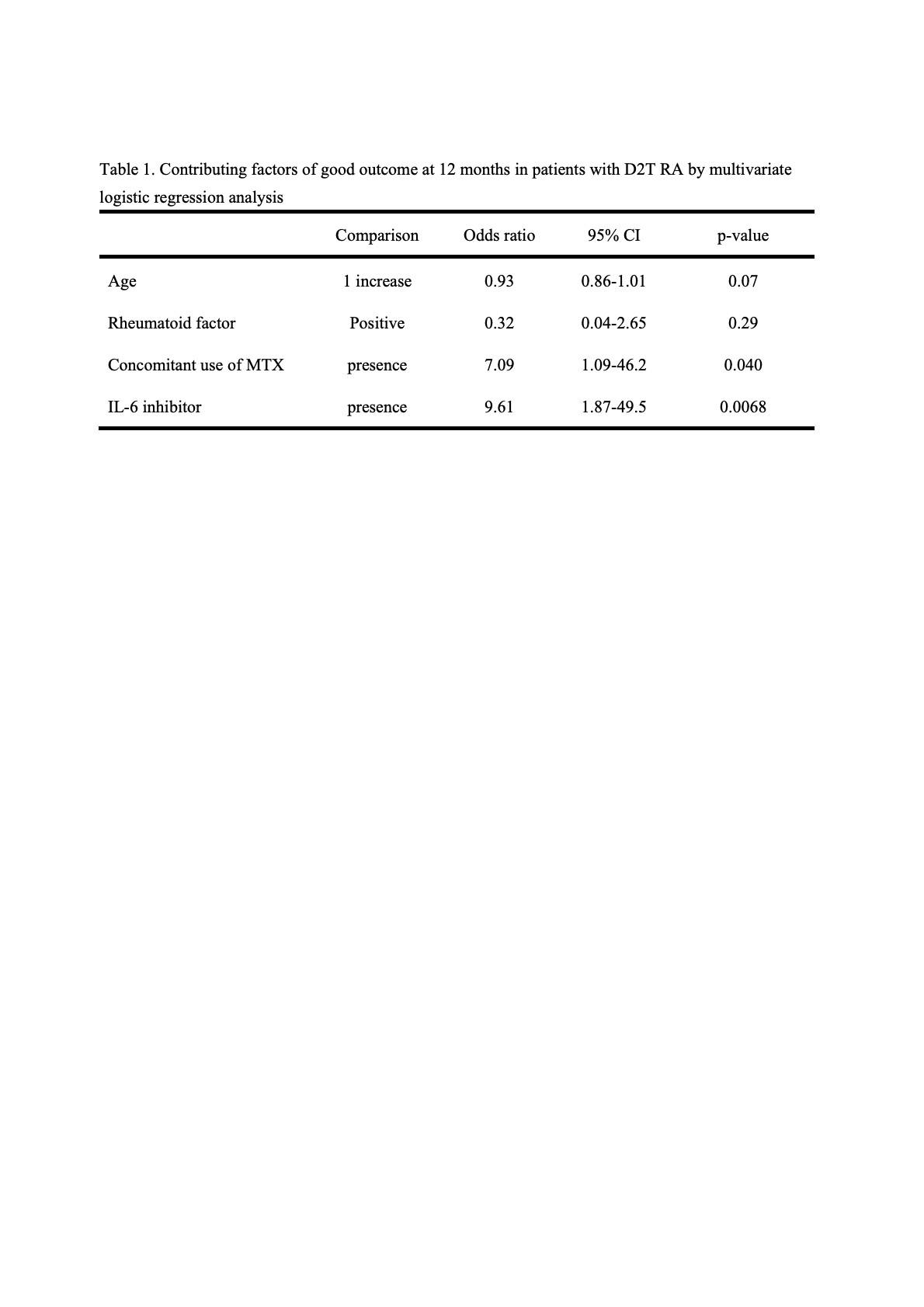
Results: Among 366 patients with RA, 74 (20.2%) were D2T RA. Disease duration, the positivity of rheumatoid factor, a complication of interstitial pneumonia, concomitant use of glucocorticoids, clinical disease activity scores and MSUS scores were significantly higher in D2T RA compared with non-D2T RA. There was no significant difference in the continuation rate at 12 months between D2T RA and non-D2T RA (60.8 vs 67.8%, p=0.44). Clinical and ultrasound remission (CDAI ≤2.8 and PD=0) rates at 12 months were significantly lower in D2T RA compared with non-D2T RA (9.5 vs 24.3%, p=0.0053). When good outcome at 12 months was defined as the achievement of CDAI remission with the continuation of b/tsDMARDs, 14 (18.9%) have achieved a good outcome. Multivariate logistic regression analysis showed that IL-6 inhibitor therapy (odds ratio 9.61, 95% confidence interval [CI] 1.87–49.5, p=0.0068) and concomitant use of methotrexate (MTX) (odds ratio 7.09, 95%CI 1.09–46.2, p=0.040) were independent contributors of good outcome (Table 1).
Conclusion: In our ultrasound cohort study, one-fifth of patients were classified as D2T RA at study entry. In patients with D2T RA, concomitant use of MTX and treatment with IL-6 inhibitors were associated with clinical remission and treatment continuation at 12 months.
To cite this abstract in AMA style:
Kawashiri S, Michitsuji T, Endo Y, Nishino A, Shimizu T, Sumiyoshi R, Koga T, Iwamoto N, Ichinose K, Kawakami A. Contributing Factors of Good Outcome in Difficult-to-treat Rheumatoid Arthritis: A Multicenter RA Ultrasound Prospective Observational Cohort Study in Japan [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/contributing-factors-of-good-outcome-in-difficult-to-treat-rheumatoid-arthritis-a-multicenter-ra-ultrasound-prospective-observational-cohort-study-in-japan/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/contributing-factors-of-good-outcome-in-difficult-to-treat-rheumatoid-arthritis-a-multicenter-ra-ultrasound-prospective-observational-cohort-study-in-japan/