Session Information
Session Type: Poster Session (Sunday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Systemic Sclerosis (SSc) is a progressive fibrotic and vascular disease with peripheral manifestations including arthritis, tendinopathy, sclerodactyly, contractures, calcinosis, acroosteolysis, and vascular disease which can lead to significant pain, deformity, and functional impairment. Tender joints (TJs) and swollen joints (SJs) are frequently encountered in SSc, but identifying their exact cause remains challenging. Prior studies have suggested inflammatory arthritis is present in anywhere from 25% to 49% of SSc patients. We sought to use ultrasound (US) to evaluate the prevalence of inflammatory arthritis and other joint and soft tissue pathology and to assess for associations with presence of TJs and SJs.
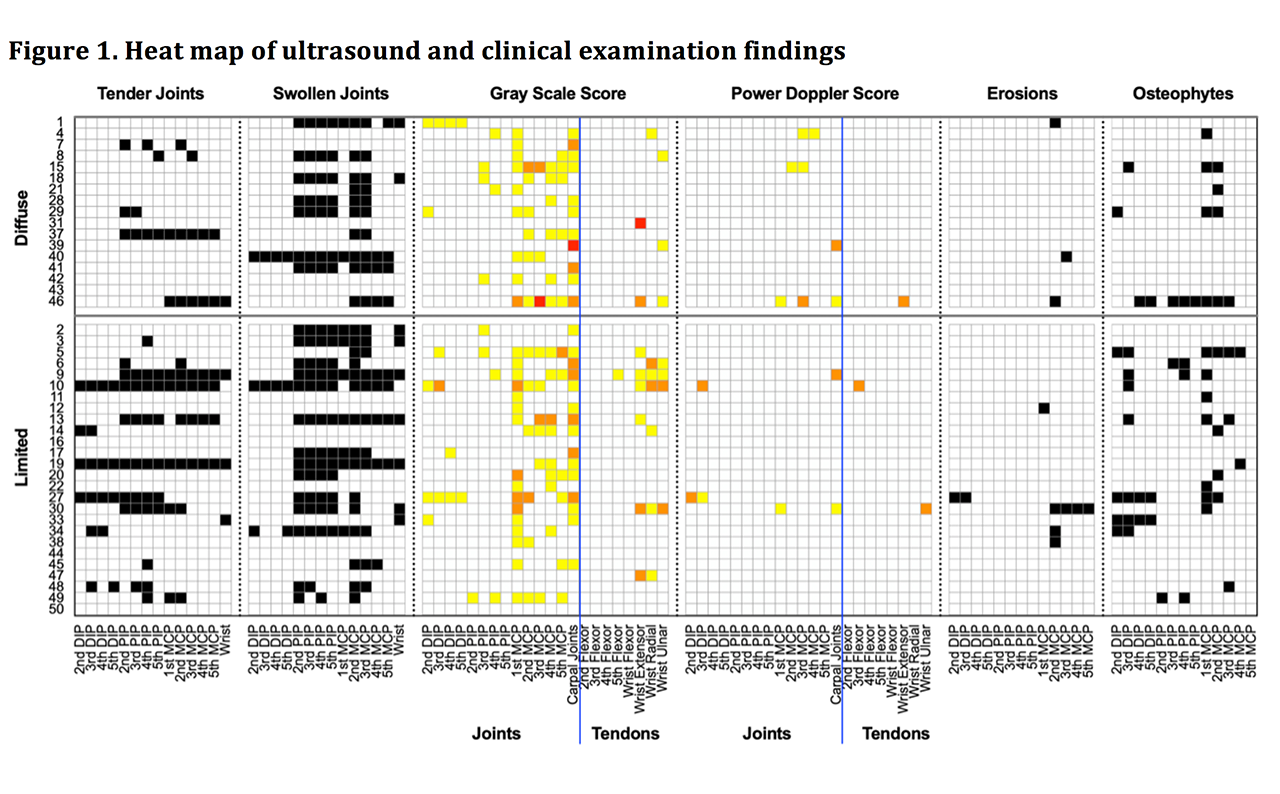
Methods: Patients meeting ACR/EULAR classification criteria for SSc were prospectively evaluated by US of the hands and wrists. Bilateral B-mode and power doppler exams of the joints and tendons were rated on a semiquantitative scoring system (0-3) for both gray scale (GS, a marker of synovial hypertrophy) and power doppler (PD, a marker of hyperemia and active inflammation). Studies were scored blindly by 3 experienced sonographers using OMERACT consensus guidelines. US also evaluated for erosions (ER), osteophytes (OS), ulnar artery occlusion (UAO), and median nerve cross sectional area. TJs, SJs, modified Rodnan skin score (MRSS), contractures, and ulcerations were assessed clinically. Concordance between US features and TJs and SJs was assessed using chance-corrected Cohen’s Kappa statistic. Severity scores for GS, PD, OS, ER, TJs and SJs for each patient were obtained by summation. Correlations between the severity of TJs and SJs and US features were assessed by Spearman’s rank correlation.
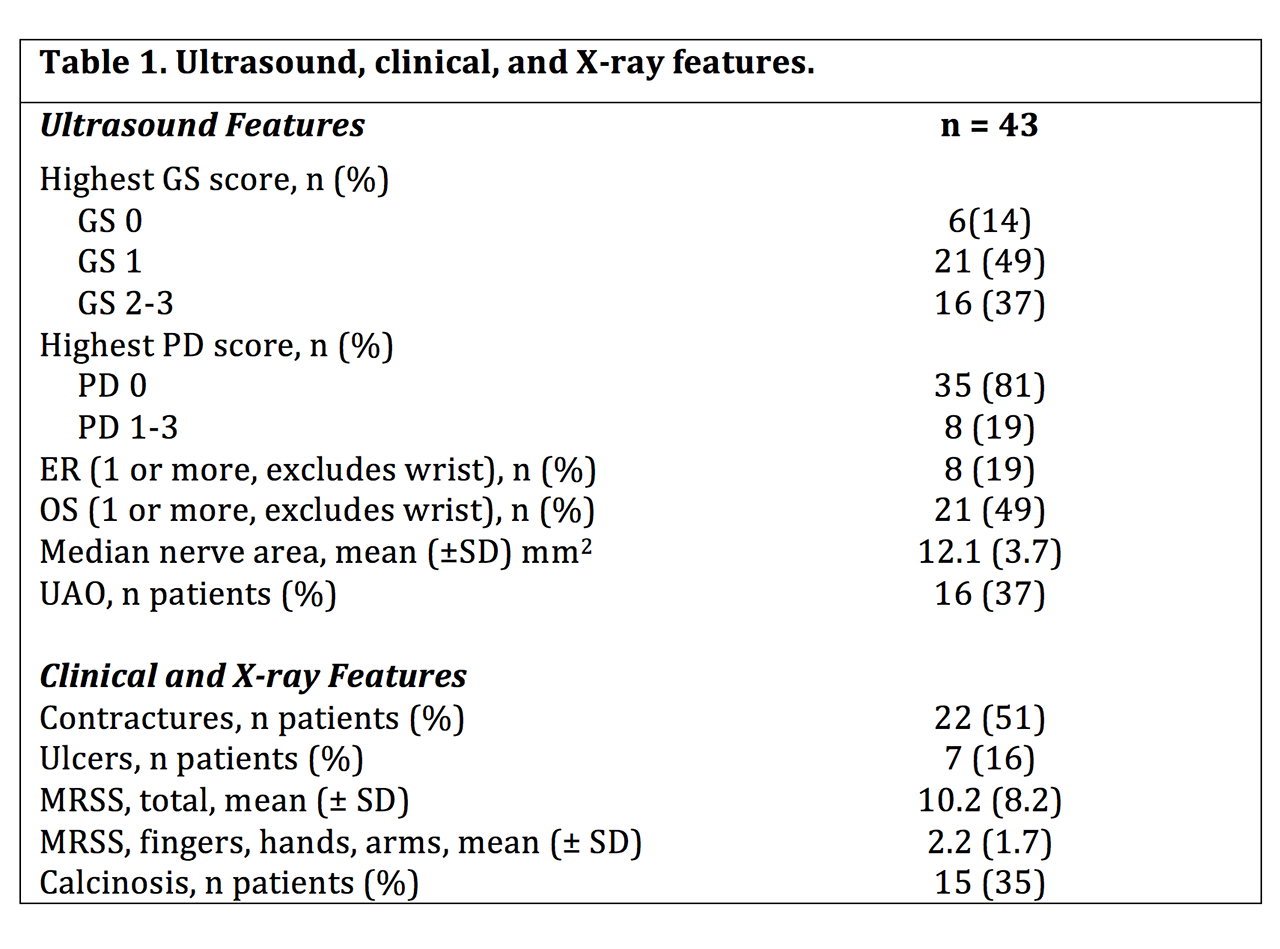
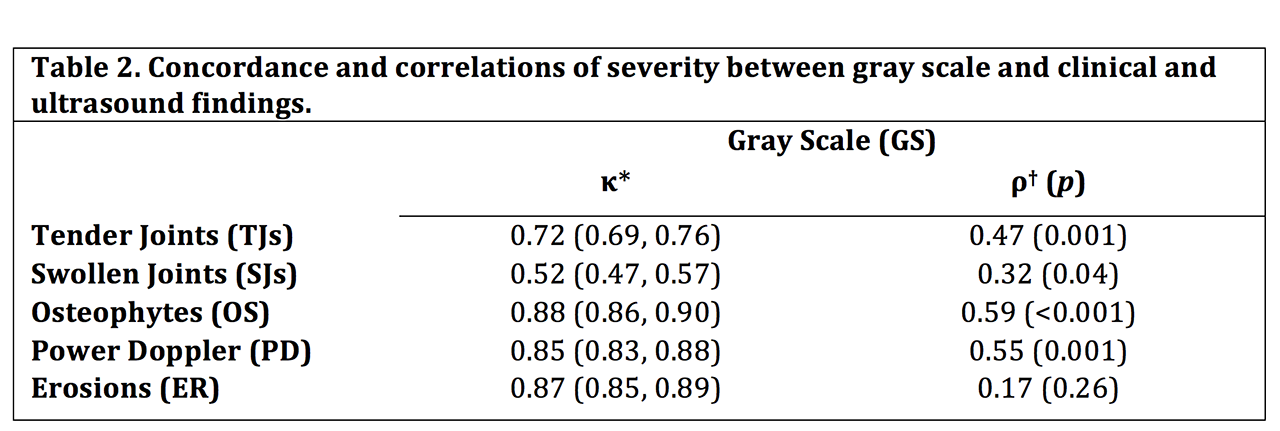
Results: 43 SSc patients (17 diffuse, mean age 58 ± 13.5) were evaluated by US. GS = 2-3 in at least one joint or tendon was seen in 16 (37%) of patients and PD > 0 in at least one joint or tendon was observed in 8 (19%) of patients (Table 1). TJs and SJs did not correlate with median nerve cross sectional area, UAO, calcinosis, digital ulcers, MRSS, or contractures. GS had higher concordance with and severity correlated more strongly with TJs than SJs. Both OS and PD severity strongly correlated with GS severity (Table 2). Of the 37 SSc patients with positive GS findings, PD and OS were seen in 22% and 54% of patients, respectively. Of the 19 patients with TJs, PD and OS were seen in 26% and 74% of patients, respectively.
Conclusion: US revealed a relatively low prevalence of active inflammatory arthritis of 19% as noted by infrequent PD findings. A majority of patients with GS and TJs were found to have OS while PD was less frequent, suggesting US findings of synovial hypertrophy and clinical TJs may be better explained by osteophytosis rather than active inflammatory arthritis.
To cite this abstract in AMA style:
Fairchild R, Chung M, Sharpless L, Li S, Hong J, Sheth K, Chung L. Ultrasound Evaluation of the Hands in Patients with Systemic Sclerosis: Osteophytosis Is a Major Contributor to Tender Joints [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/ultrasound-evaluation-of-the-hands-in-patients-with-systemic-sclerosis-osteophytosis-is-a-major-contributor-to-tender-joints/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/ultrasound-evaluation-of-the-hands-in-patients-with-systemic-sclerosis-osteophytosis-is-a-major-contributor-to-tender-joints/