Session Information
Date: Tuesday, November 9, 2021
Title: Patient Outcomes, Preferences, & Attitudes Poster IV: COVID-19 (1589–1613)
Session Type: Poster Session D
Session Time: 8:30AM-10:30AM
Background/Purpose: The COVID-19 pandemic has had substantial impact on the care of patients with autoimmune rheumatic diseases (ARDs), resulting in frequent medication interruptions early in the pandemic. This study used longitudinal data to examine trends in medication interruptions and patients’ feelings of anxiety throughout the pandemic and to evaluate whether medication interruptions were associated with an increased risk for disease flares.
Methods: Members of the ArthritisPower and Vasculitis Patient Powered Research Network online patient registries and other patient organizations were invited to complete a baseline survey (week 0) and then every 2 weeks until week 8, monthly until week 28, with a final survey at week 38. We analyzed patients with ARDs who completed baseline surveys between March 29 and June 30, 2020 and completed at least one follow-up survey, with follow-up captured through February 2021. Changes over time in PROMIS Anxiety T-scores and medication interruptions due to COVID-19 concerns (among patients receiving DMARDs) were assessed using generalized estimating equation (GEE) models to account for within-person correlations. GEE models were also used to assess associations between medication interruptions and self-reported disease flares at the next survey among patients on DMARDs who were not currently in a flare, adjusting for demographics, medication type, disease type, and calendar time.
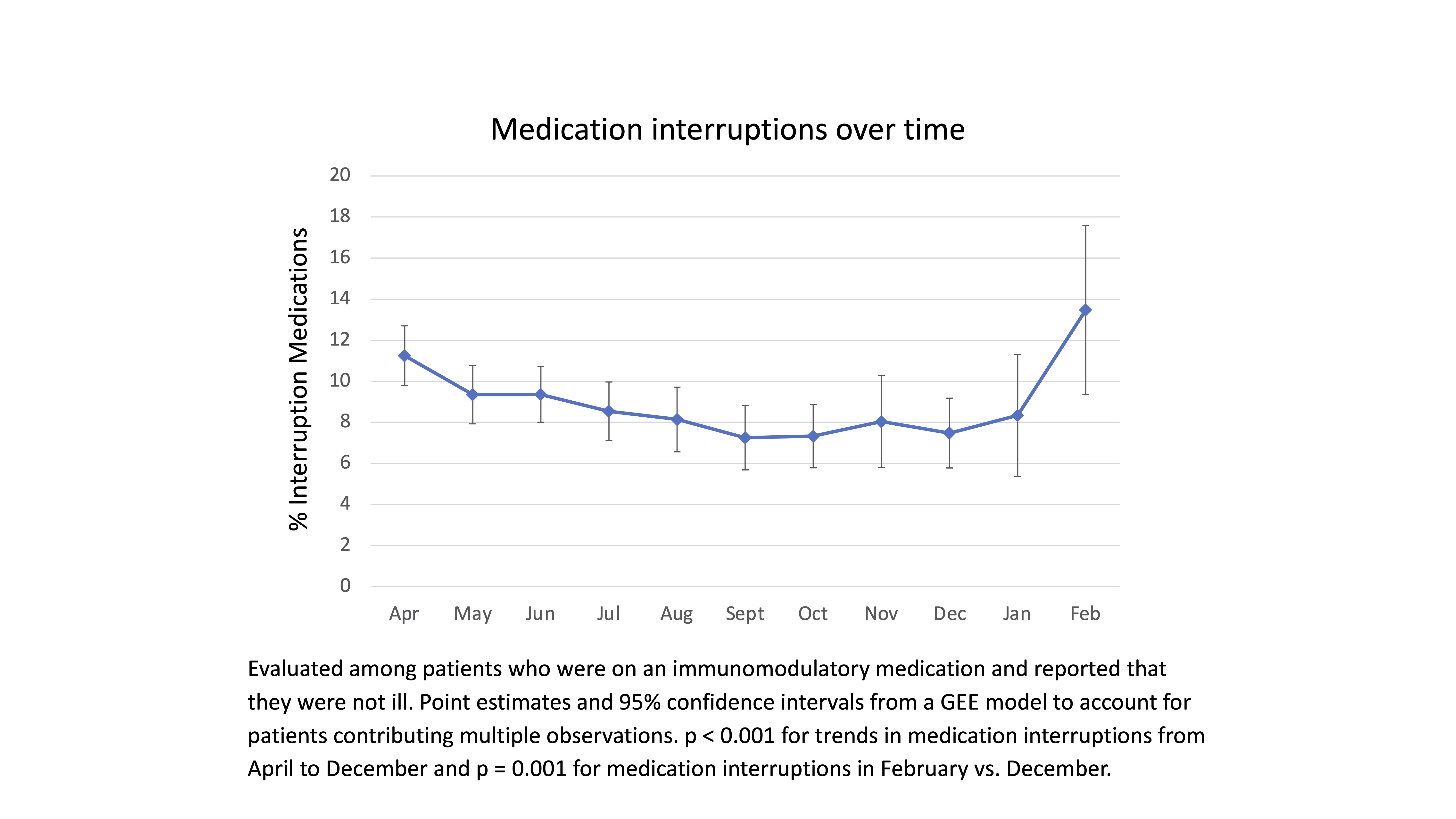
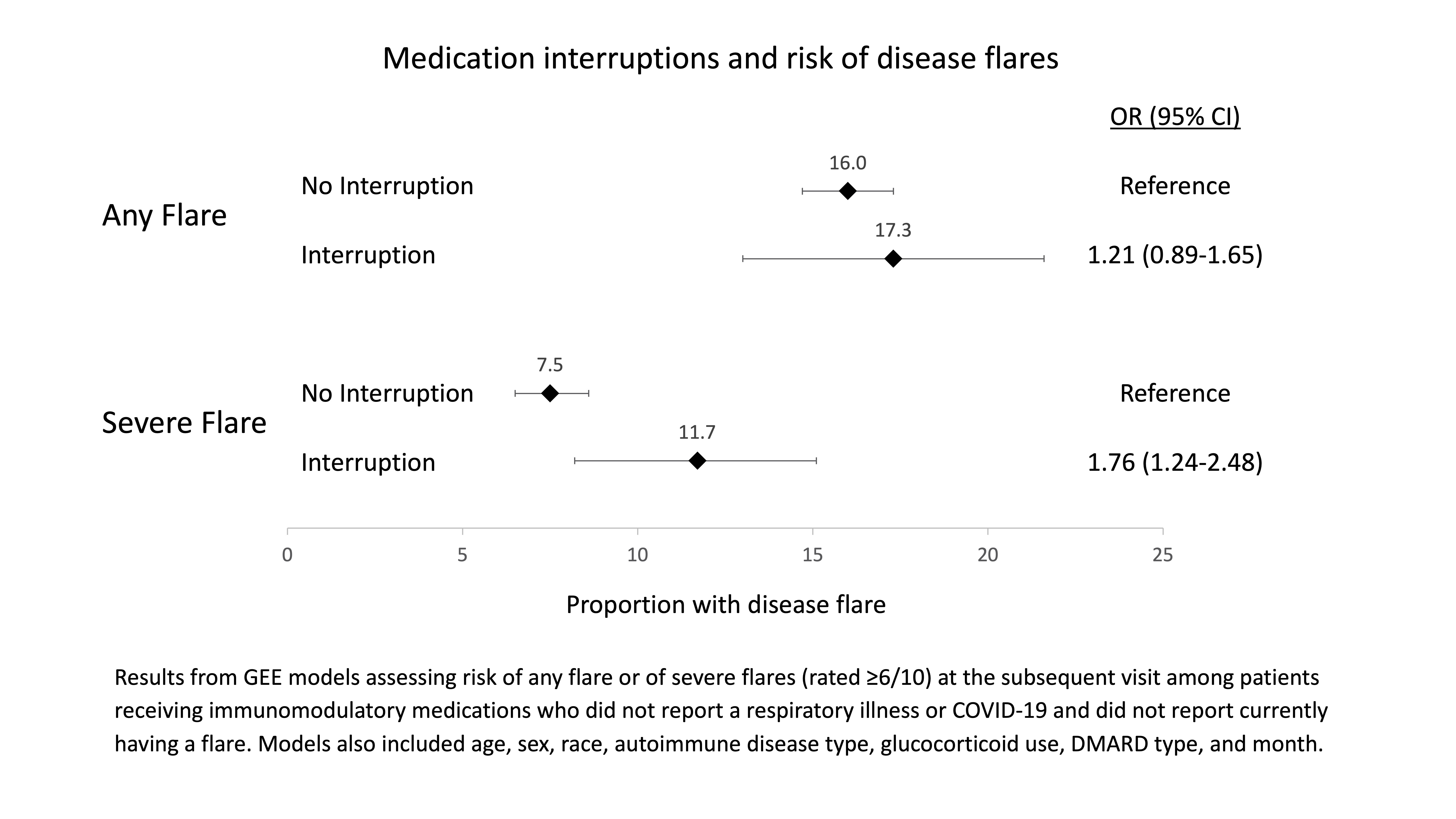
Results: A total of 2,396 patients completed a median of 6 surveys (interquartile range 3-9). Mean age was 57 years, 87% were female, and the most common ARDs were rheumatoid arthritis, vasculitis, and psoriatic arthritis (Table 1). Average PROMIS-Anxiety T scores decreased significantly from 59.0 in April 2020 to 55.6 in February 2021 (p < 0.001 for trend) and medication interruptions also decreased significantly from April (11.2%) to December 2020 (7.5%) (p < 0.001 for trend) but increased to 13.5% in February 2021 (p = 0.001 vs. December) (Figure 1). Medication interruptions were more common in those with higher anxiety (p < 0.001), occurring in 10.5% with PROMIS-Anxiety T-score ≥60 vs. 7.8% with score < 60. 1,419 patients had at least one survey response during which they were on DMARDs and did not report a current flare (5,270 total responses). Among this population, 839 (15.9%) reported any flare and 459 (8.7%) a severe flare (≥6/10) at the next survey. Medication interruptions were associated with a significant increase in the risk of severe flare [11.7% vs. 7.5%; OR 1.76 (95% CI 1.24-2.48)] (Figure 2).
Conclusion: Patients with ARDs had high levels of anxiety and frequent medication interruptions at the start of the COVID-19 pandemic. Although anxiety and frequency of medication interruptions improved over time, interruptions increased in February of 2021, possibly related to vaccination efforts or the national surge in COVID-19. Medication interruptions were associated with an increased risk of severe disease flares, highlighting the importance of maintaining continuity of care and avoiding unnecessary medication interruptions during the pandemic and future public health crises.
To cite this abstract in AMA style:
Dharia T, George M, VENKATACHALAM S, Banerjee S, Baker J, Curtis D, Danila M, Gavigan K, Merkel P, Shaw D, Curtis J, Nowell W. Trends in Medication Interruptions and Associations with Disease Flares During a Public Health Crisis: Longitudinal Data from Patients with Autoimmune Rheumatic Diseases During the COVID-19 Pandemic [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/trends-in-medication-interruptions-and-associations-with-disease-flares-during-a-public-health-crisis-longitudinal-data-from-patients-with-autoimmune-rheumatic-diseases-during-the-covid-19-pandemic/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/trends-in-medication-interruptions-and-associations-with-disease-flares-during-a-public-health-crisis-longitudinal-data-from-patients-with-autoimmune-rheumatic-diseases-during-the-covid-19-pandemic/