Session Information
Date: Saturday, November 7, 2020
Title: Epidemiology & Public Health Poster II: OA, Osteoporosis, & Other Rheumatic Disease
Session Type: Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose: An association between ulcerative colitis (UC) and peripheral arthritis has been known since the 1930’s and more recently has been described as a part of the spectrum of peripheral Spondyloarthritis (p-SpA). Prevalence rates of p-SpA in UC have been reported with varying estimates from clinical and cohort studies. To our knowledge there are no US population-based studies to estimate the prevalence of UC-associated peripheral arthritis or arthralgia. We describe herein population-based rates of peripheral arthritis and arthralgia among those with and without UC using previously unreported data from NHANES II (1976-80), a nationally-representative survey of the US population.
Methods: NHANES II participants ages 20-69 were interviewed and examined by physicians at mobile examination centers and defined as having UC if they reported having been diagnosed with UC by a physician. Previous analysis of NHANES II and NHANES 2009-10 data showed these self-reports to be consistent with true UC given corresponding high rates of colonoscopy, surgery, UC-related comorbidities, and UC-related symptoms.
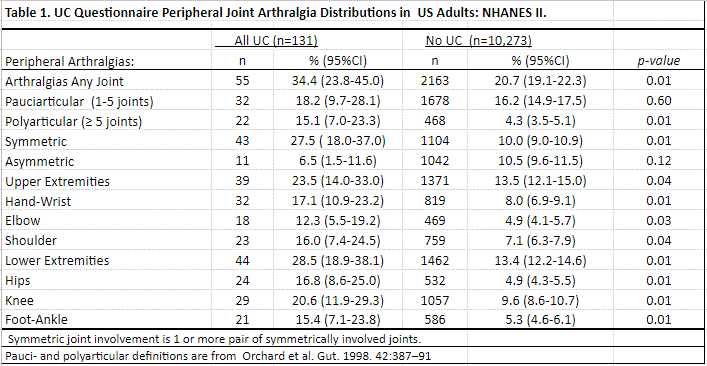
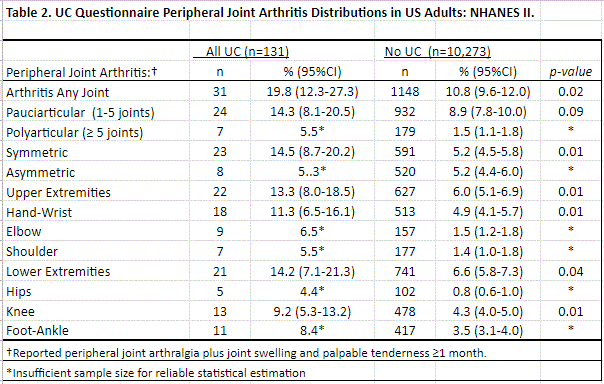
Interview data was collected for a present or past history of peripheral arthralgias for ≥6 weeks (Table 1) and of arthritis signs and symptoms (arthralgias plus joint swelling and tenderness for ≥1 month) (Table 2). A physician joint exam was also performed (Table 3). Statistical analysis used SASTM 9.4 using survey design variables and sample weights to produce nationally representative estimates.
Results: 10,404 participants were interviewed and examined, 131 with a history of UC. 34% of those with UC reported present or past peripheral arthralgias (an estimated 400,000 persons nationwide) compared to 21% of those without (p=0.01). Rates of overall present or past polyarticular arthralgias, and of arthralgias at the hand and wrist, elbow, shoulder, hip, knee, and foot and ankle were all elevated among those with UC (all p< 0.05) (Table 1). 20% of participants with UC reported present or past peripheral arthritis compared to 11% without (p=0.02; Table 2). Rates of arthritis at the hand and wrist and knee were significantly elevated in UC (p< 0.05 for both). Rates of arthritis at the elbow, shoulder, hip, and foot and ankle were all elevated, but sample size precluded statistical evaluation (Table 2).
Overall, those with UC had significantly increased exam findings (28% vs. 12% without; p=0.03), notably increased pain on passive joint motion (12% with UC vs. 7% without; p=0.03). The rates of joint swelling on exam were similarly low in both groups (Table 3). On exam, Heberden’s Node prevalences were similar between both groups.
Conclusion: Rates of self-reported peripheral arthralgia and arthritis were elevated in NHANES II participants who reported a history of UC compared to the general population. However, while rates of joint pain with motion on exam were elevated in UC, rates of examination-based swelling were not. This may suggest that much of much of UC patients’ joint pain is due to peri-articular structure involvement, including possible tenosynovitis and enthesitis, and that point-prevalence of true arthritis is low consistent with p-SpA patients.
To cite this abstract in AMA style:
Stens O, Kim H, Hou J, Weisman M. The US Prevalence of Ulcerative Colitis Associated Peripheral Arthralgias and Arthritis: Data from the National Health & Nutrition Examination Survey (NHANES) [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/the-us-prevalence-of-ulcerative-colitis-associated-peripheral-arthralgias-and-arthritis-data-from-the-national-health-nutrition-examination-survey-nhanes/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/the-us-prevalence-of-ulcerative-colitis-associated-peripheral-arthralgias-and-arthritis-data-from-the-national-health-nutrition-examination-survey-nhanes/