Session Information
Date: Thursday, March 30, 2023
Title: Poster Breakout 1 - Lupus: Genetics, Epigenetics, & Social Determinants
Session Type: Breakout Session
Session Time: 5:10PM-5:40PM
Background/Purpose: Differences in prevalence rates of childhood-onset SLE (cSLE) among different racial/ethnic groups have been well described. Yet, the role of social determinants of health (SDoH) in severity of presentation is not well understood. We hypothesized that in an urban center with a large, diverse catchment area, SDoH may influence the severity of cSLE at initial diagnosis.
Methods: We completed an IRB-approved retrospective review of children diagnosed with cSLE between 1/1/18 – 5/31/22 at Texas Childrens Hospital in Houston, TX. Patients were excluded if diagnosis was made at an outside institution or diagnosed at 18 years. We abstracted demographics, clinical characteristics and SDoH data such as insurance status, social work consultation and access to PCP. Statistical analyses were performed using Stata v15.1 (StataCorp, College Station, TX, USA) and comparisons were made using ANOVA and Kruskal-Wallis tests.
Results: The mean age of the 136 patients who met inclusion criteria was 13.4 years + 3 SD. The majority of patients were female (n=112, 82.4%) and ~80% were Hispanic White (n=72, 52.9%) or Black (n=35, 25.7%). Fourteen (10.3%) patients were uninsured and 50% (n=68) had Medicaid or Childrens Health Insurance Program (CHIP). Half of the patients (n=68) were diagnosed during an inpatient admission with 49 (36%) on the floor and 19 (14%) in the ICU. The average SLEDAI was 12.5 + 7.1 SD with 48.5% (n=66) of patients presenting with SLEDAI 12 (severe disease). One third of patients preferred a language other than English (n=44, 32.4%). Only 66% (n=91) of patients had a documented PCP. Social work was consulted in most patients as per section protocol (n=109, 80.1%); specific reasons listed in Table 1.
The distribution of race/ethnicity showed varied disease activity (SLEDAI and number of ACR criteria), CNS involvement and CYC therapy at levels that reached statistical significance (Table 2). Black and Biracial populations had higher SLEDAI scores at presentation (P =0.01). Non-Hispanic White patients were less likely to have a social work consult compared to the other race/ethnicities (P =0.01). CNS involvement was highest among Black children (P=0.004). CYC was most often used in Black and Biracial populations (P=0.003).
Several demographic and SDoH parameters influenced disease severity at levels that reached statistical significance, including insurance status, race/ethnicity, referral source, PCP availability, primary language, and transportation needs. When assessed by insurance status, uninsured patients were most likely to be diagnosed on an inpatient floor and those with Medicaid had the highest proportion of ICU admissions (P=0.034; Table 3). Uninsured patients and those on Medicaid had the highest percentage of social work consults (P =0.001).
Conclusion: In children drawn from a large urban catchment area, we observed an influence of race/ethnicity on disease severity, and also potential SDoH proxy measures (non-English primary language, insurance status and transportation barriers). Work is underway to target modifiable SDoH in our catchment area.
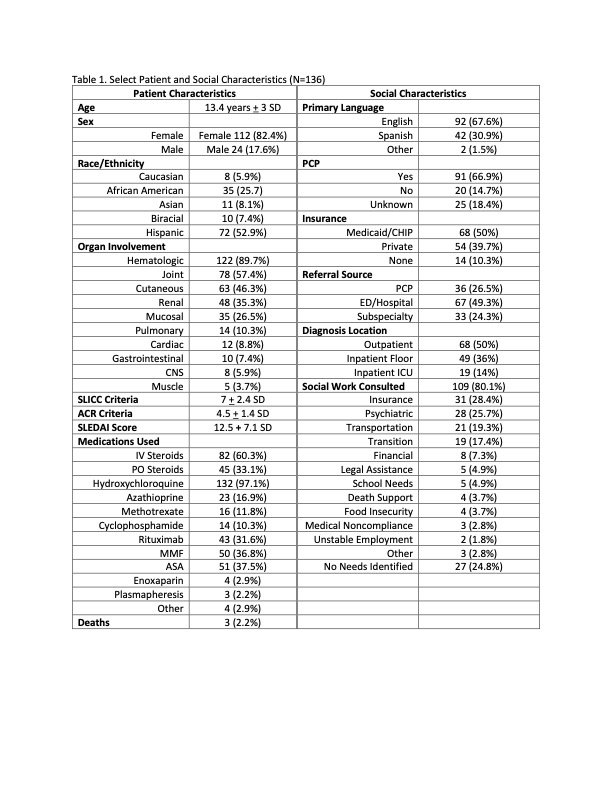 Table 1. Select Patient and Social Characteristics (Nf136)
Table 1. Select Patient and Social Characteristics (Nf136)
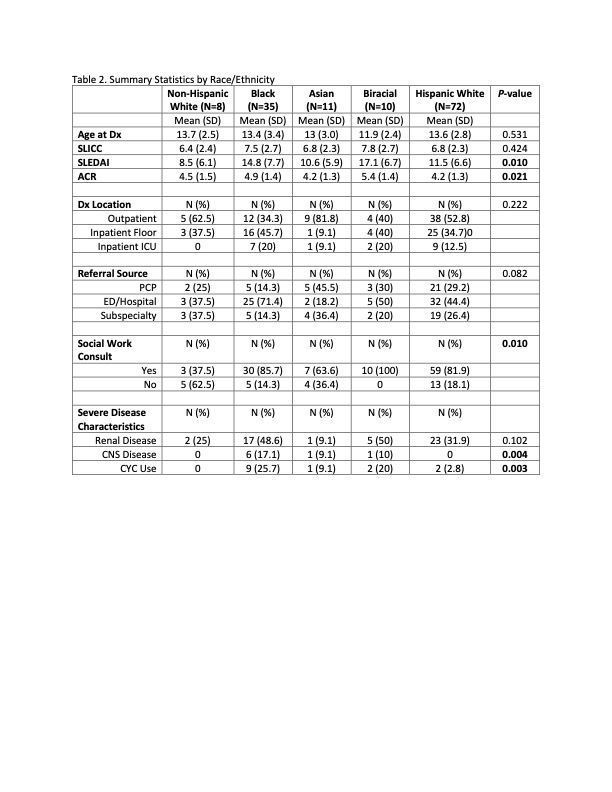 Table 2. Summary Statistics by Race/Ethnicity
Table 2. Summary Statistics by Race/Ethnicity
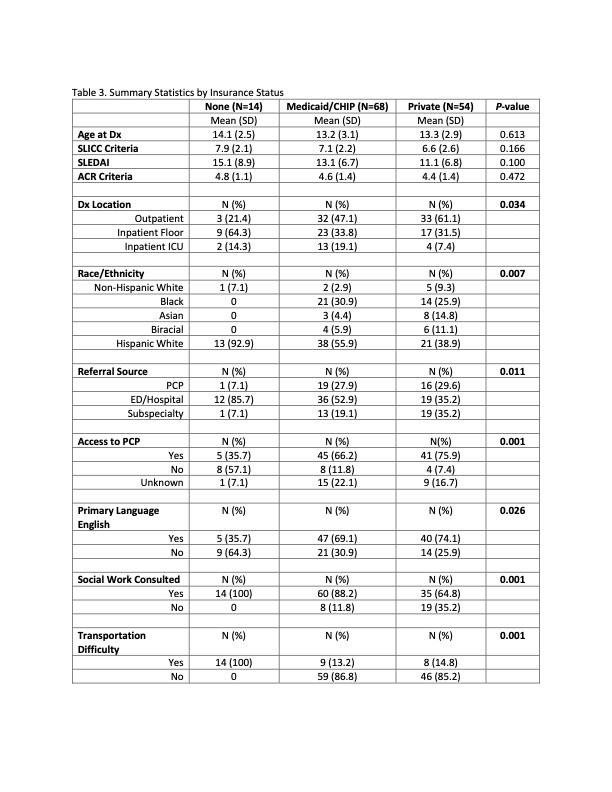 Table 3. Summary Statistics by Insurance Status
Table 3. Summary Statistics by Insurance Status
To cite this abstract in AMA style:
Beil E, Muscal E, Guffey D, Deguzman M, Peckham-Gregory E. The Impact of Social Inequities on Presentation of Childhood-Onset Systemic Lupus Erythematosus (cSLE) at a Large Tertiary Center [abstract]. Arthritis Rheumatol. 2023; 75 (suppl 4). https://acrabstracts.org/abstract/the-impact-of-social-inequities-on-presentation-of-childhood-onset-systemic-lupus-erythematosus-csle-at-a-large-tertiary-center/. Accessed .« Back to 2023 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/the-impact-of-social-inequities-on-presentation-of-childhood-onset-systemic-lupus-erythematosus-csle-at-a-large-tertiary-center/
