Session Information
Session Type: Abstract Submissions (ACR)
Background/Purpose:
Approximately 25% of psoriasis (Ps) patients develop psoriatic arthritis (PsA), a potentially destructive joint disease, within 10 years of Ps onset. Although early diagnosis and therapy of PsA can prevent bone and joint damage, diagnostic and response biomarkers of psoriatic diseases are currently absent. To address this unmet need, we focused on Dendritic Cell-Specific Transmembrane protein (DC-STAMP), a valid marker of osteoclast precursors (OCP). We examined the frequency of the DC-STAMP+IL-17+ subset (monocytes and T cells) in the peripheral blood of healthy controls (HC), Ps and PsA patients and monitored this cell subset in PsA patients before and after the anti-Tumor Necrosis therapy (TNFi).
Methods:
Ps was confirmed by a dermatologist and PsA by a rheumatologist based on the CASPAR criteria. Blood samples were collected from 61 subjects (Ps, n=19; PsA, n=17; HC, n=25). Blood samples from PsA patients were collected at baseline and 16 weeks following treatment with an anti-TNF reagent (adalimumab, infliximab or etanercept). Cell populations were analyzed by flow cytometry with an 11-color antibody cocktail and OC were enumerated by TRAP staining after 8-day cell culture in vitro.
Results:
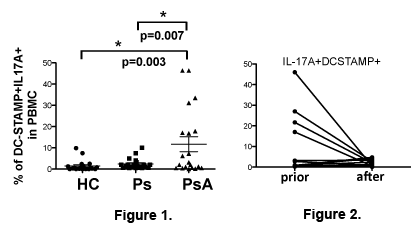 The DC-STAMP+IL-17+ subset was significantly increased in PsA but not in Ps or HC (Figure 1). The area under the Receiver Operating Characteristic (ROC) curve for DC-STAMP+IL17A+ cells (PsA vs. HC) was 0.769. The DC-STAMP+IL17A+ cell frequency decreased significantly following TNFi therapy in PsA patients considered as anti-TNFi responders (12 out of 17). Figure 2 summarizes the frequency of DC-STAMP+IL17A+ before and after anti-TNFi medication (8.2 ± 13.7 (prior) vs. 1.6 ± 1.5 (after), p=0.09). Intriguingly, the reduction in DC-STAMP+IL17A+ cell subset was associated with a decreased circulating OCP frequency (930 ± 857 (prior) vs. 142 ± 144 (after) / per 106 monocytes, p=0.004).
The DC-STAMP+IL-17+ subset was significantly increased in PsA but not in Ps or HC (Figure 1). The area under the Receiver Operating Characteristic (ROC) curve for DC-STAMP+IL17A+ cells (PsA vs. HC) was 0.769. The DC-STAMP+IL17A+ cell frequency decreased significantly following TNFi therapy in PsA patients considered as anti-TNFi responders (12 out of 17). Figure 2 summarizes the frequency of DC-STAMP+IL17A+ before and after anti-TNFi medication (8.2 ± 13.7 (prior) vs. 1.6 ± 1.5 (after), p=0.09). Intriguingly, the reduction in DC-STAMP+IL17A+ cell subset was associated with a decreased circulating OCP frequency (930 ± 857 (prior) vs. 142 ± 144 (after) / per 106 monocytes, p=0.004).
Conclusion:
Our results demonstrate that the DC-STAMP+IL17A+ cell subset: (1) can distinguish PsA from HC and Ps subjects; (2) declines rapidly following TNFi therapy; (3) positively correlates with circulating OCPs. Collectively, these data reveal a novel susceptibility and response biomarker and underscore the importance of IL-17 expressing cells in PsA pathogenesis.
Disclosure:
Y. G. Chiu,
None;
E. M. Schwarz,
Laget Inc.,
1,
Laget Inc.,
2,
DePuy Inc.,
2,
DePuy Inc.,
5,
Boehringer Ingelheim,
7;
H. He,
None;
F. A. Tausk,
None;
S. Moorehead,
None;
M. Smith,
None;
C. T. Ritchlin,
Amgen, Janssen, UCB, Abbott, Boerhinger Ingleheim, Lilly, ,
5.
« Back to 2013 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/the-dc-stampil17a-cell-subset-is-elevated-in-psoriatic-arthritis-psa-patients-and-declines-following-anti-tnfi-therapy/
