Session Information
Date: Tuesday, November 12, 2019
Title: Epidemiology & Public Health Poster III: OA, Gout, & Other Diseases
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Gout is a common inflammatory arthritis, characterized by hyperuricemia leading to crystallization of uric acid in joints. Proinflammatory cytokines have been known as an increasing factor for osteoporotic fractures, and chronic inflammatory diseases such as rheumatoid arthritis (RA) are considered to be a risk factor for osteoporosis and fractures. However, association between hyperuricemia and osteoporotic fractures, and relationship between gout and osteoporotic fractures has shown conflicting results. We hypothesized that older patients with gout would have a similar risk of osteoporotic fracture compared with older patients with RA.
Methods: Using claims data from Medicare Parts A/B/D (2008-2015), we conducted a cohort study. We selected gout with ≥2 diagnosis codes and ≥1 dispensing for gout treatment. Similarly, RA were identified with ≥2 diagnosis codes and ≥1 dispensing for disease-modifying antirheumatic drugs. Gout patients were 1:1 matched to RA patients on age, sex, and index date. The primary outcome was non-vertebral fractures, a composite endpoint of humerus, wrist, pelvis or hip fracture, based on previously validated claims-based algorithms (PPV > 93%). The secondary outcome was hip fracture. We calculated the incidence rate (IR) of non-vertebral fracture and hip fracture in each group. Cox proportional hazards regression estimated the hazard ratio (HR) with 95% confidence intervals (CI) for the primary and secondary outcomes in gout versus RA, adjusting for 45 baseline risk factors for osteoporosis.
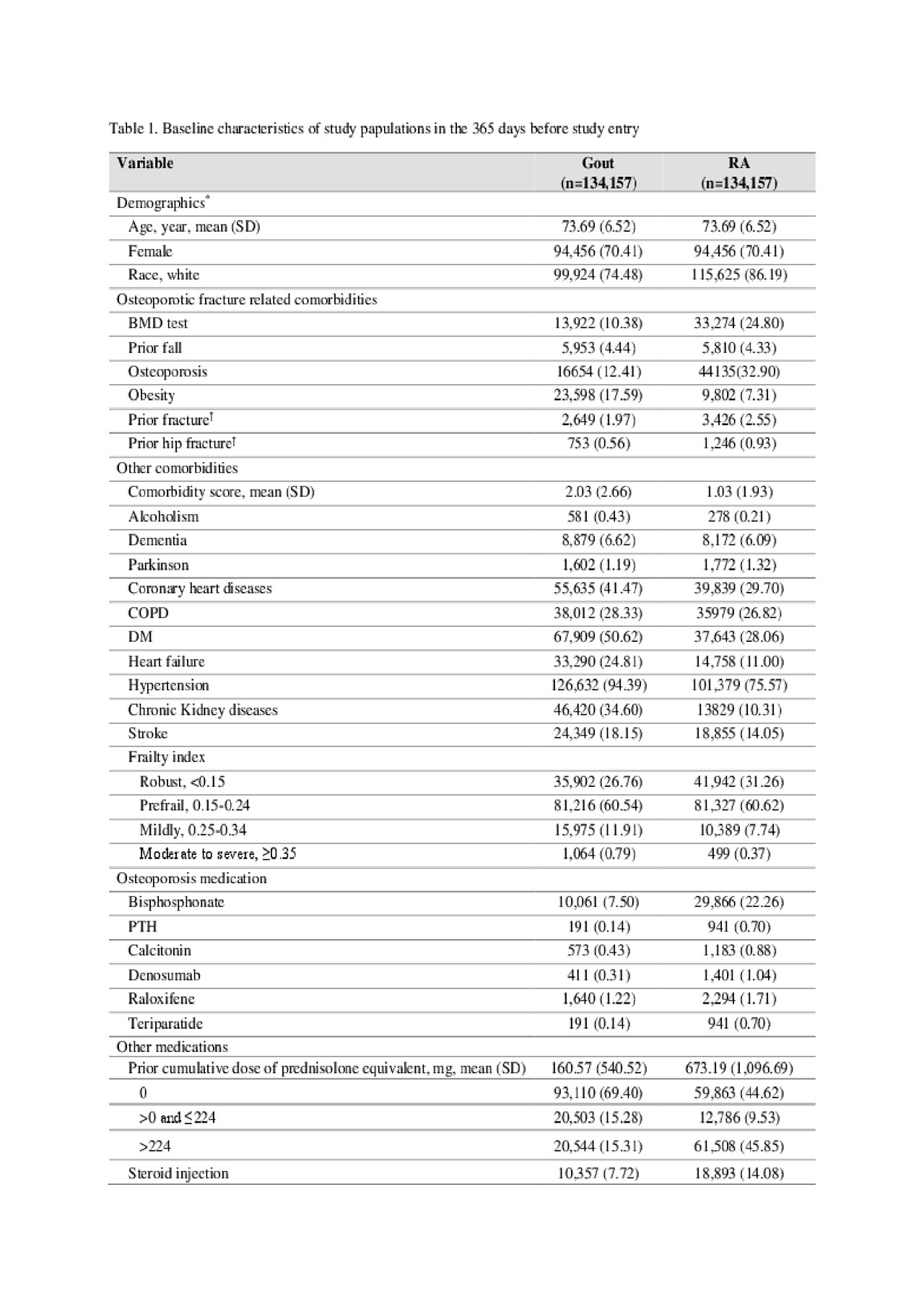
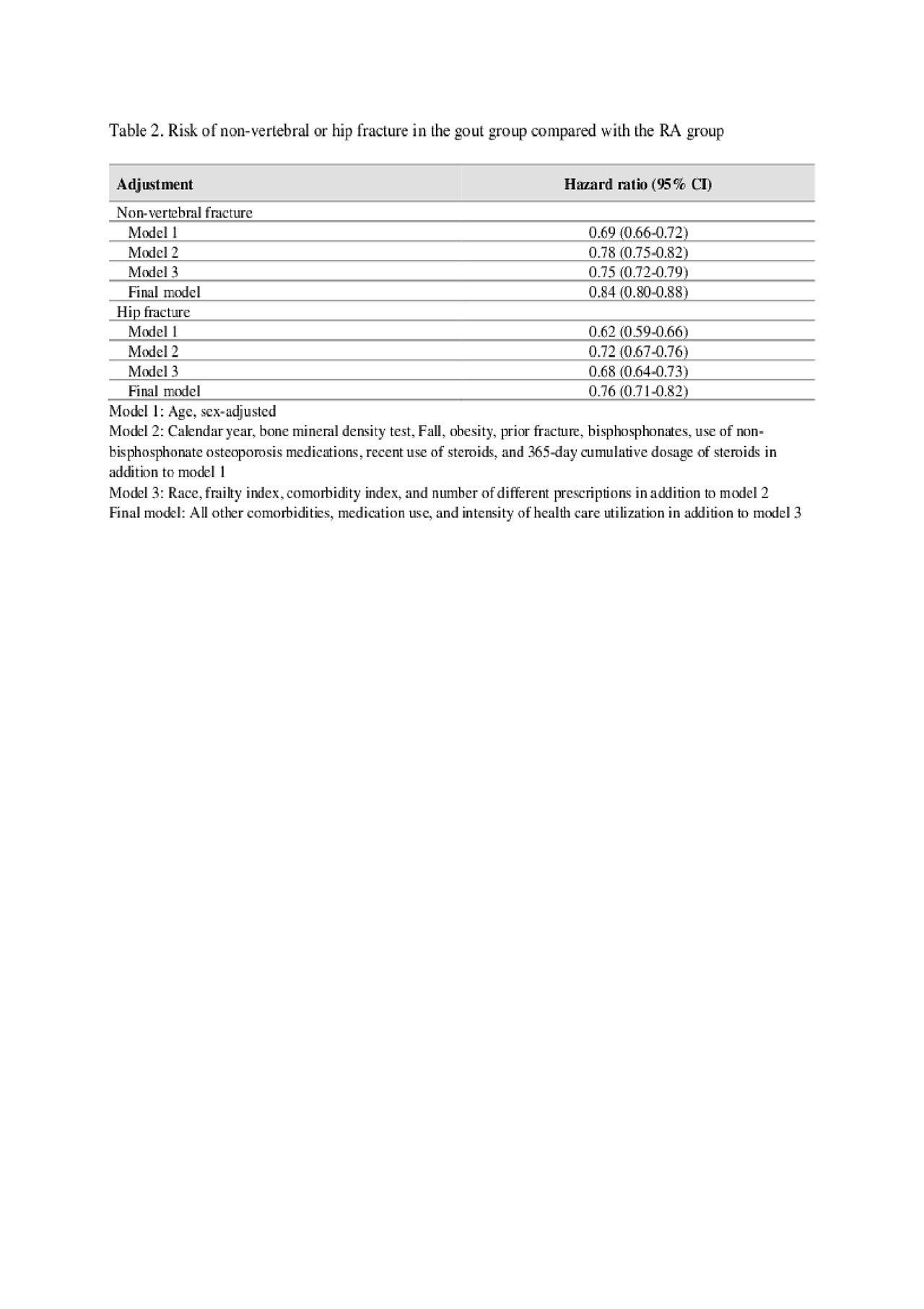
Results: We included a total of 134,157 matched pairs of gout and RA patients with mean age of 73.7 years. 70.4% were female. Risk factors of osteoporotic fracture such as receipt of a bone mineral density test, diagnosis of osteoporosis, prior fracture, use of osteoporosis medication, and steroid use were more prevalent in RA than gout. However, other comorbidities including obesity, coronary heart disease, heart failure, hypertension, hyperlipidemia, diabetes, and chronic kidney disease were more frequently noted in gout than RA (Table 1). Over the mean 2.8-year follow up, the IR per 1,000 person-year (PY) of non-vertebral fractures was 10.42 in gout and 15.01 in RA, and the IR per 1,000 PY of hip fracture was 4.86 in gout and 7.73 in RA. The IR of non-vertebral fractures was more than twofold higher in patients aged ≥75 years than patients aged 65-74 years, and about threefold higher in the patients with prior fracture than the patients without prior fracture in both groups. Multivariable HR associated with gout versus RA was 0.84 (95% CI 0.80-0.88) for non-vertebral fractures and 0.76 (95% CI 0.71-0.82) for hip fractures (Table 2). Subgroup analyses by age, sex, history of prior fractures, 365-day cumulative dose of steroids and absence of TNF inhibitor use showed similar results (Figure).
Conclusion: In this large cohort of older patients enrolled in Medicare, the absolute rate of non-vertebral fractures or hip fractures was high in both gout and RA. However, gout was associated with a decreased risk of non-vertebral and hip fractures regardless of age, sex, steroid use and prior fracture, compared to RA.
FractureRisk_gout_2019ACR_abstract_ver0.6_table1
FractureRisk_gout_2019ACR_abstract_ver0.6_table2

FractureRisk_gout_2019ACR_abstract_ver0.6_figure
To cite this abstract in AMA style:
Cho S, Liu J, Kim S. Risk of Non-vertebral Fracture in Gout Compared to Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/risk-of-non-vertebral-fracture-in-gout-compared-to-rheumatoid-arthritis/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/risk-of-non-vertebral-fracture-in-gout-compared-to-rheumatoid-arthritis/
