Session Information
Date: Saturday, November 7, 2020
Title: Epidemiology & Public Health Poster II: OA, Osteoporosis, & Other Rheumatic Disease
Session Type: Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose: The most common site of osteoporotic fragility fractures is the thoracic spine. However, bone mineral density (BMD) measurements at the hip are used to predict fracture risk using tools like FRX™, while spinal measurements only assess response to treatment. Dual energy X-ray absorptiometry (DEXA) measures BMD at lumbar vertebrae L1-3 and L1-4, user-dependant. It is not known if predictors of hip osteoporosis and fracture mimic those for vertebral osteoporosis.
Aim:
- Evaluate factors associated with osteoporosis in the lumbar spine in female patients presenting for BMD estimation.
Methods: Female patients presenting for BMD estimation at a district general hospital in North West England, 2004-2016, were studied. In addition to BMD in L1-4, demographics, fracture history, and risk factors were recorded. Logistic regression models at each lumbar vertebral level were used to identify predictors of osteoporosis (T-score≤-2.5).
Results: 26119 unique patients underwent BMD estimation during our study period, mean age of 65.0 years (SD 12.4). Other characteristics are shown in Table 1. Fragility fractures were significantly associated with increased osteoporosis risk at all lumbar levels. Current aromatase inhibitor-use and hormone replacement therapy (HRT) were associated with significantly decreased likelihood of osteoporosis at all lumbar levels. All other demographics, co-morbidities, and medications investigated were associated with osteoporosis at varying lumbar levels.
Conclusion: Our results show a clear difference in co-morbidities and medication-use associated with osteoporosis at different lumbar levels. Traditional risk factors for osteoporosis are not associated with decreased BMD in the lumbar spine. Patients with vertebral osteoporosis were more likely to sustain fragility fractures as expected. HRT is bone-protective and was therefore associated with decreased likelihood of osteoporosis. Current aromatase inhibitor use was associated with decreased likelihood of osteoporosis at all lumbar levels, while current corticosteroid use was associated with decreased likelihood of osteoporosis in the lower lumbar region. Both medications are known to reduce BMD- these results are confounded by concurrent use of calcium, vitamin D, and bisphosphonate treatment.
SLE was associated with reduced likelihood of osteoporosis at the superior and inferior lumbar spine, also likely confounded by treatment. Current hyperthyroidism was associated with significantly increased risk of osteoporosis averaged throughout the lumbar spine, consistent with previous studies. Current alcohol intake was associated with decreased risk of osteoporosis at L3, consistent with previous work demonstrating a protective effect of low-moderate alcohol intake on bone health.
In conclusion, we demonstrate risk factors for low BMD are not equal throughout the lumbar spine, and differ from traditional osteoporotic risk factors, including those commonly used in predictive scores for fracture. Our results suggest a need to consider risk factors specific to lumbar spine osteoporosis when planning prevention and management of vertebral fragility fractures.
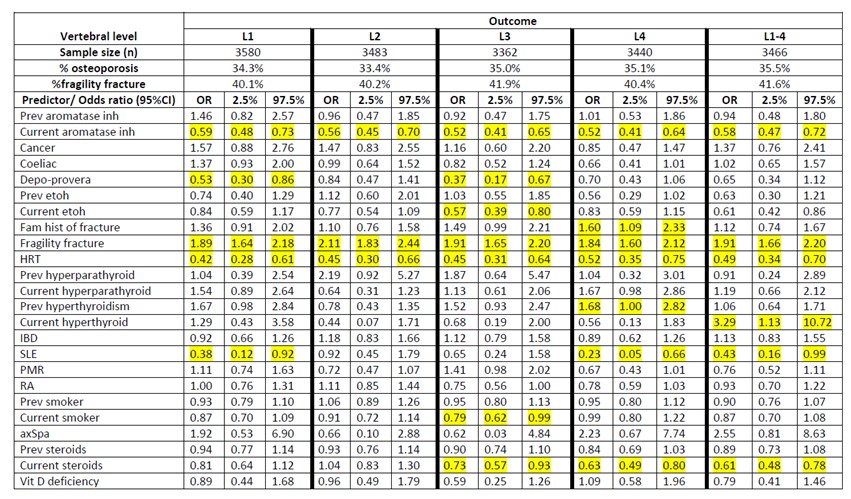 Table 1: Odds ratios for risk of osteoporosis, associated with co-morbidities and medication-use, in the lumbar vertebral spine
Table 1: Odds ratios for risk of osteoporosis, associated with co-morbidities and medication-use, in the lumbar vertebral spine
To cite this abstract in AMA style:
Bukhari M, Dey M. Risk Factors for Lumbar Vertebral Osteoporosis Do Not Reflect Factors Traditionally Associated with Osteoporosis at the Hip [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/risk-factors-for-lumbar-vertebral-osteoporosis-do-not-reflect-factors-traditionally-associated-with-osteoporosis-at-the-hip/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/risk-factors-for-lumbar-vertebral-osteoporosis-do-not-reflect-factors-traditionally-associated-with-osteoporosis-at-the-hip/
