Session Information
Date: Monday, November 9, 2020
Session Type: Poster Session D
Session Time: 9:00AM-11:00AM
Background/Purpose: As the rheumatology workforce experiences an alarming shortage, it is critical that rheumatology fellows receive advanced training experiences to reinforce their commitment to rheumatology patient care and to strengthen their knowledge, competency, and skills in evidence-based management for common conditions like rheumatoid arthritis (RA). As part of a continuing medical education (CME) program in RA, we conducted a survey study in which rheumatology fellows rated their training in RA care.
Methods: On October 5, 2019, rheumatology residents and fellows from 20 US-based academic institutions were selected by their program directors to attend a 1-day educational workshop in RA. Three RA experts designed and led the interactive presentations, case-based discussions, and Q&A sessions. Pre-program surveys included items for trainees to assess and rate their challenges, confidence, and experience in various aspects of RA care. Post-program surveys included items assessing the impact of the education in these domains.
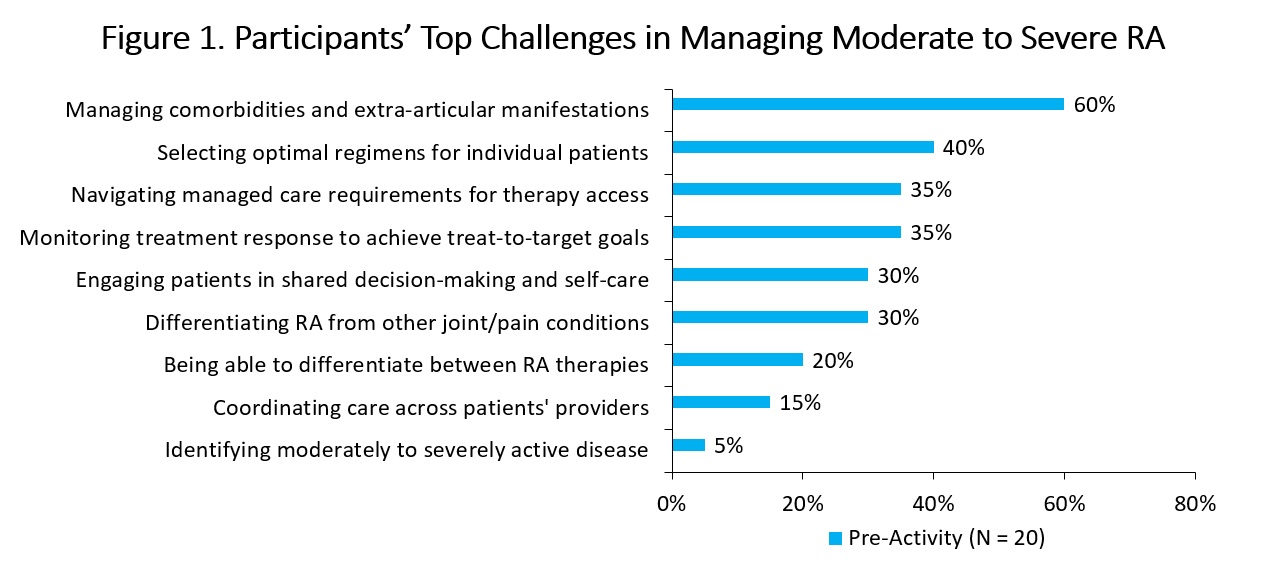
Results: Surveys were completed by 20 rheumatology residents and fellows (10% PGY2, 15% PGY3, and 75% fellows); 70% were female and had a median age of 31 years old. Participants indicated their main challenges in RA care are managing comorbidities and extra-articular manifestations (60%); selecting optimal regimens for individual patients (40%); navigating managed care requirements (35%); and monitoring treatment response to achieve treat-to-target goals (35%; Figure 1). Methods used by the participants to assess RA disease activity included joint examination (95%), clinical judgement (90%), laboratory tests (80%), validated disease severity scores (75%), and patient-reported outcomes (40%).
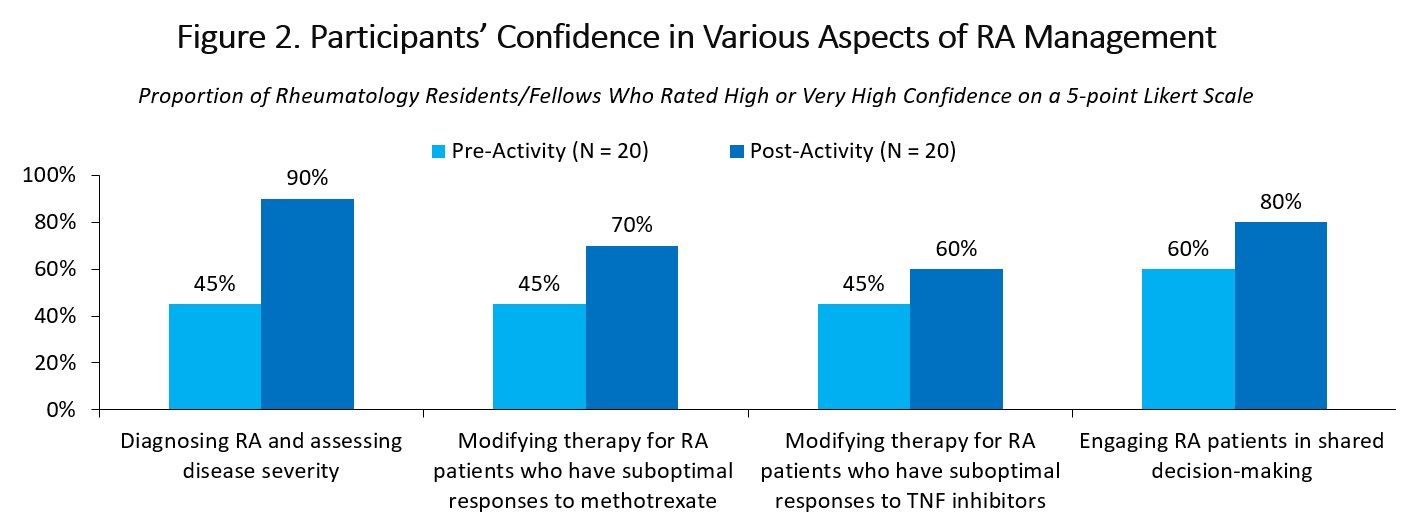
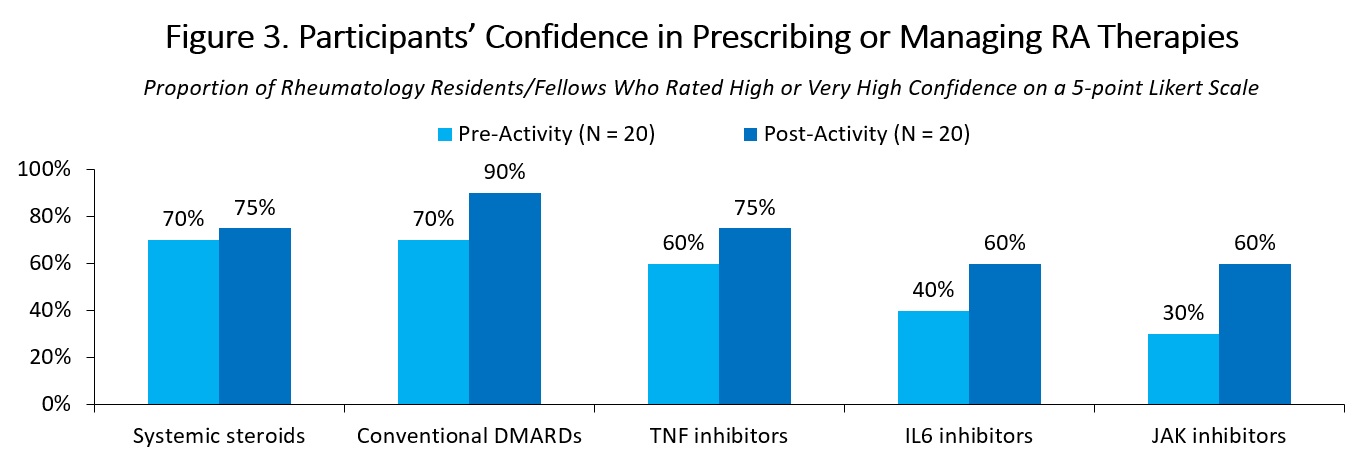
Before the education, low proportions of participants reported high confidence in performing various aspects of RA care, including diagnosing RA and assessing disease severity (45% with high or very high confidence), modifying therapy for patients with inadequate response to methotrexate (45%) or TNF inhibitors (45%), and engaging patients in shared decision-making (60%; Figure 2). After the education, participants reported increased confidence in these domains. In a separate question, 70% of participants reported high or very high confidence in prescribing or managing patients who are on systemic steroids and conventional synthetic DMARDs (Figure 3); lower proportions of participants reported high or very high confidence in prescribing or managing patients on TNF, IL-6, and JAK inhibitors (60%, 40%, and 30% respectively). These proportions also increased in post-program survey.
Lastly, the survey assessed participants’ perspectives on strategies for addressing the shortage of rheumatologists in the US. Most participants (55%) indicated that creating collaborative models with primary care would have the largest impact on addressing patient needs in the immediate future.
Conclusion: Educational gaps exist among rheumatology residents and fellows in their confidence, perspectives, and experience in RA patient care. These findings can help develop additional education opportunities for fellows that help close these gaps.
To cite this abstract in AMA style:
Agarwal S, Manno R, Fajardo K, Simone L, Carter J, Sapir T. RA-Related Knowledge and Skills of Rheumatology Fellows Among 20 US Academic Institutions [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/ra-related-knowledge-and-skills-of-rheumatology-fellows-among-20-us-academic-institutions/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/ra-related-knowledge-and-skills-of-rheumatology-fellows-among-20-us-academic-institutions/