Session Information
Date: Tuesday, November 15, 2016
Title: Systemic Lupus Erythematosus – Clinical Aspects and Treatment - Poster III: Biomarkers and Nephritis
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: Approximately half of SLE patients develop lupus nephritis (LN), a major cause of morbidity and early mortality. It is known that prolonged renal inflammation is associated with irreversible kidney damage and leads to end stage renal disease (ESRD), making early aggressive treatment mandatory. Failure to achieve therapeutic response or recurrence of renal flare should prompt repeat biopsy, as changes in renal activity and chronicity are known to occur. However, the role of repeat biopsy in determining long-term renal prognosis remains controversial.
Methods: To test the hypothesis that histopathologic worsening between first and second biopsies might be predictive of ESRD and death, the medical records of 141 LN patients with >1 biopsy were obtained from a single large urban medical center. Cases were initially attained using procedure and diagnosis billing codes from 1/1999-1/2015, with subsequent retrospective chart review. Worsening of biopsies was defined as unfavorable histopathologic classification transitions or worsening of chronicity; if neither were present, the patient was defined as non-worsening. Covariates in the Cox proportional hazard models included age at first biopsy, gender, race, initial biopsy class, and initial induction therapy.
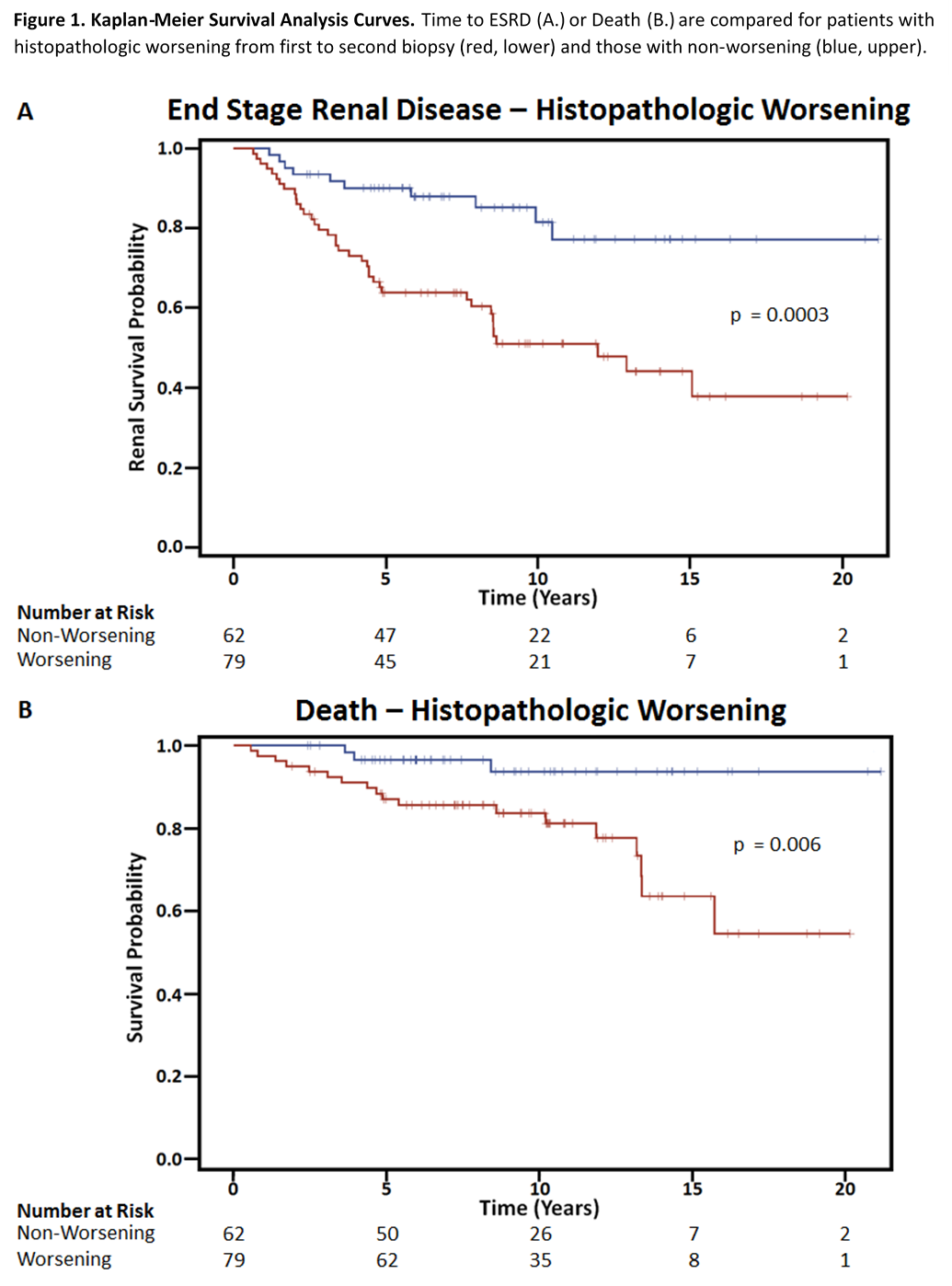
Results: Of 630 patients initially screened, 141 had >1 biopsy, with characteristics as noted in Table 1. Advancing chronicity was detected in 48(34.0%) and a renal class switch to higher grade of pathology was found in 54(38.3%). At least one of these biopsy progressions was reported in 79(56.0%) patients. Five years following initial biopsy, 28(35.4%) of those with worsening histopathology on second biopsy developed ESRD, compared to 6(9.7%) of non-worsening patients (Figure 1). After only five years, 10(12.7%) of the worsening histopathology patients had died compared to 2(3.2%) of non-worsening patients. Over a 20 year period, those with worsening of nephritis at second biopsy had a significantly greater risk of ESRD (Hazard Ratio 4.2, p=0.0001) and death (Hazard Ratio 4.3, p=0.022) after adjusting for age, gender, race, biopsy class, and treatment.
Conclusion: A repeat renal biopsy demonstrating worsening pathology is strongly prognostic for poor outcomes and could justify changes in treatment that might not have been assumed necessary on clinical grounds. The high frequency of worsening in nephritis class and chronicity supports the cost effectiveness of repeat biopsy. 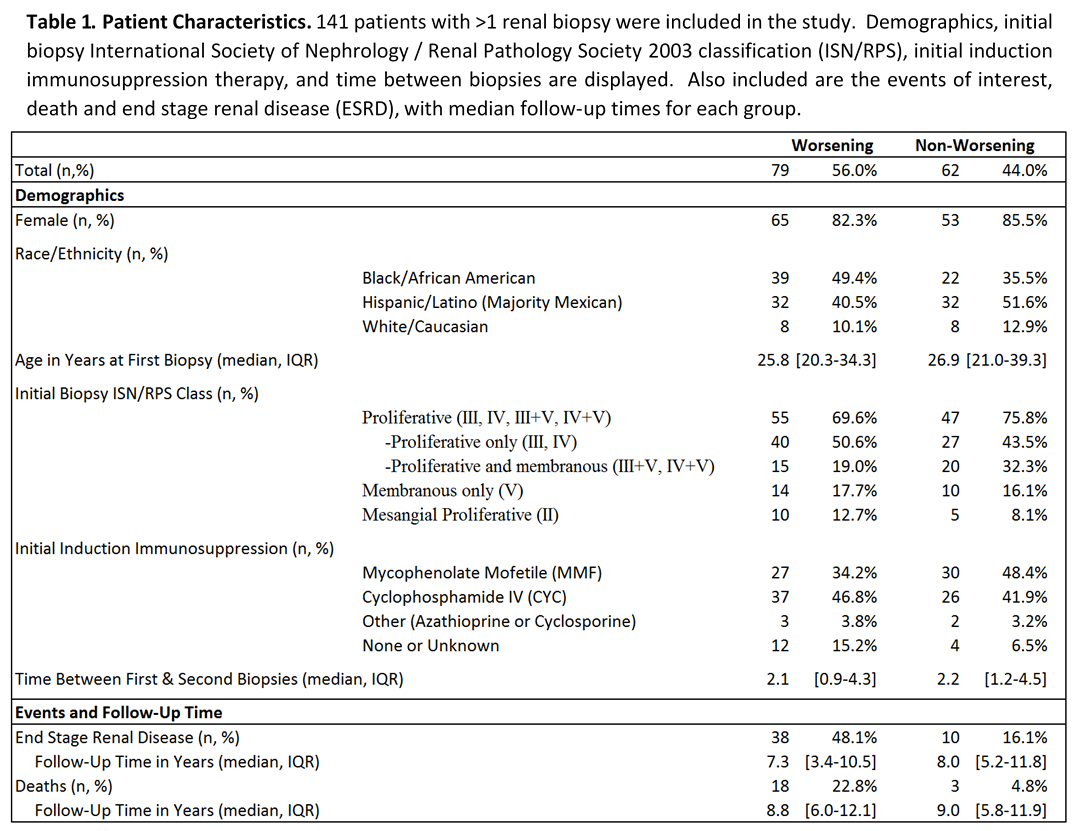
To cite this abstract in AMA style:
Arriens C, Chen S, Karp D, Saxena R, Sambandam K, Chakravarty E, James JA, Merrill JT. Prognostic Significance of Repeat Biopsy in Lupus Nephritis: Histopathologic Worsening Is an Independent Risk Factor for End Stage Renal Disease and Death [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/prognostic-significance-of-repeat-biopsy-in-lupus-nephritis-histopathologic-worsening-is-an-independent-risk-factor-for-end-stage-renal-disease-and-death/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/prognostic-significance-of-repeat-biopsy-in-lupus-nephritis-histopathologic-worsening-is-an-independent-risk-factor-for-end-stage-renal-disease-and-death/