Session Information
Date: Monday, November 9, 2020
Session Type: Abstract Session
Session Time: 11:00AM-11:50AM
Background/Purpose: Some rheumatoid arthritis (RA) patients rate their disease activity worse than their physician does, but recent prevalence and factors associated with such discordance have not been reviewed in a large real-world database. This study describes discordance at biological initiation (index visit) and over time. We hypothesized that higher levels of pain, morning stiffness, fatigue, Health Assessment Questionnaire (HAQ) score, Clinical Disease Activity Index (CDAI), and depression are associated with discordance at the index visit.
Methods: We included patients enrolled in the Corrona RA Registry who initiated their first biological or Janus kinase inhibitor on or after 2/1/2015 with both 6- and 12-month (± 3 mo) follow-up visits. Patient global assessment (PtGA) – physician’s global assessment (PhGA) (disease severity) ≥ 30 points on a 0-100 VAS scale was defined as positive discordance; > -30 to < 30 as concordance; and ≤ -30 as negative discordance. Patients with negative discordance were excluded based on prior studies. Positive discordance at all three (index, 6-, 12-mo) visits was classified as persistent discordance. Differences between discordant and concordant patients at index visit were quantified using effect sizes (standardized differences) based on Cohen’s descriptions for continuous variables (|d|): ~0.2 small effect size, ~0.5 medium, ~0.8 large; for categorical variables (w): ~0.1 small, ~0.3 medium, ~0.5 large. Mixed-effects logistic regression was used to test our a priori hypothesis.
Results: Among 54,307 patients in the registry, 758 patients met the inclusion criteria for analysis at the index visit, and of these, 752 were included in the analysis of persistent discordance. A total of 80 patients with negative discordance at any visit were excluded. Discordance prevalence was similar at the index (27%), 6- (30%), and 12-mo (30%) visits; 10% (n=65) had persistent discordance.
At the index visit (Table 1), large differences for discordant vs concordant patients included RAPID3 score (mean 16 vs 7.3, |d| = 1.5), pain (mean 63 vs 32, |d| = 1.2), fatigue (mean 61 vs 35, |d| = 0.9), morning stiffness severity (61 vs 40, w = 0.9), and HAQ (0.7 vs 0.3, w = 0.9), and a medium effect size for DAS28-ESR (mean 4.3 vs 3.6, |d| = 0.5). Results were similar for patients with persistent discordance (Table 2).
In a logistic regression model regressed on age, CDAI, opioid (including tramadol) use, pain, morning stiffness, fatigue, HAQ, depression, academic site; discordance (vs concordance) was positively associated with pain (OR=1.04, p=0.001) and HAQ (OR=1.72, p=0.053), and inversely associated with CDAI (OR=0.94, p=0.001). Morning stiffness, fatigue, and depression were not associated with discordance (Table 3).
Conclusion: About 30% of RA patients who initiated DMARDs had patient-physician discordance at any visit, and one-third of these (10% total) persisted at all three visits. Greater patient-reported pain and functional impairment were associated with discordance in adjusted models. Understanding factors associated with patient-physician discordance will help clinicians foster a more patient-centric discussion in treatment decisions.
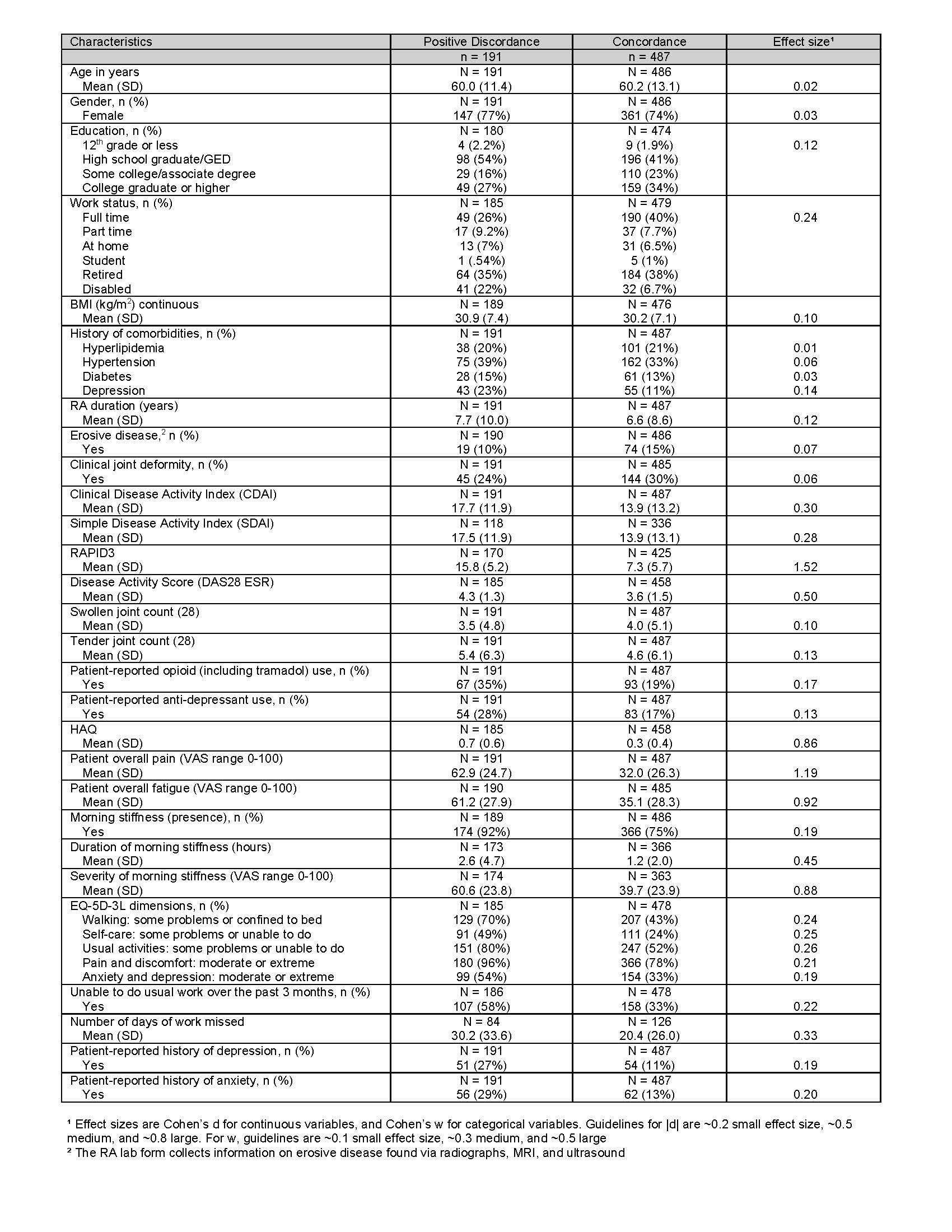 Table 1. Patient Demographics and Clinical Characteristics of Patients by Discordance Status at Index Visit
Table 1. Patient Demographics and Clinical Characteristics of Patients by Discordance Status at Index Visit
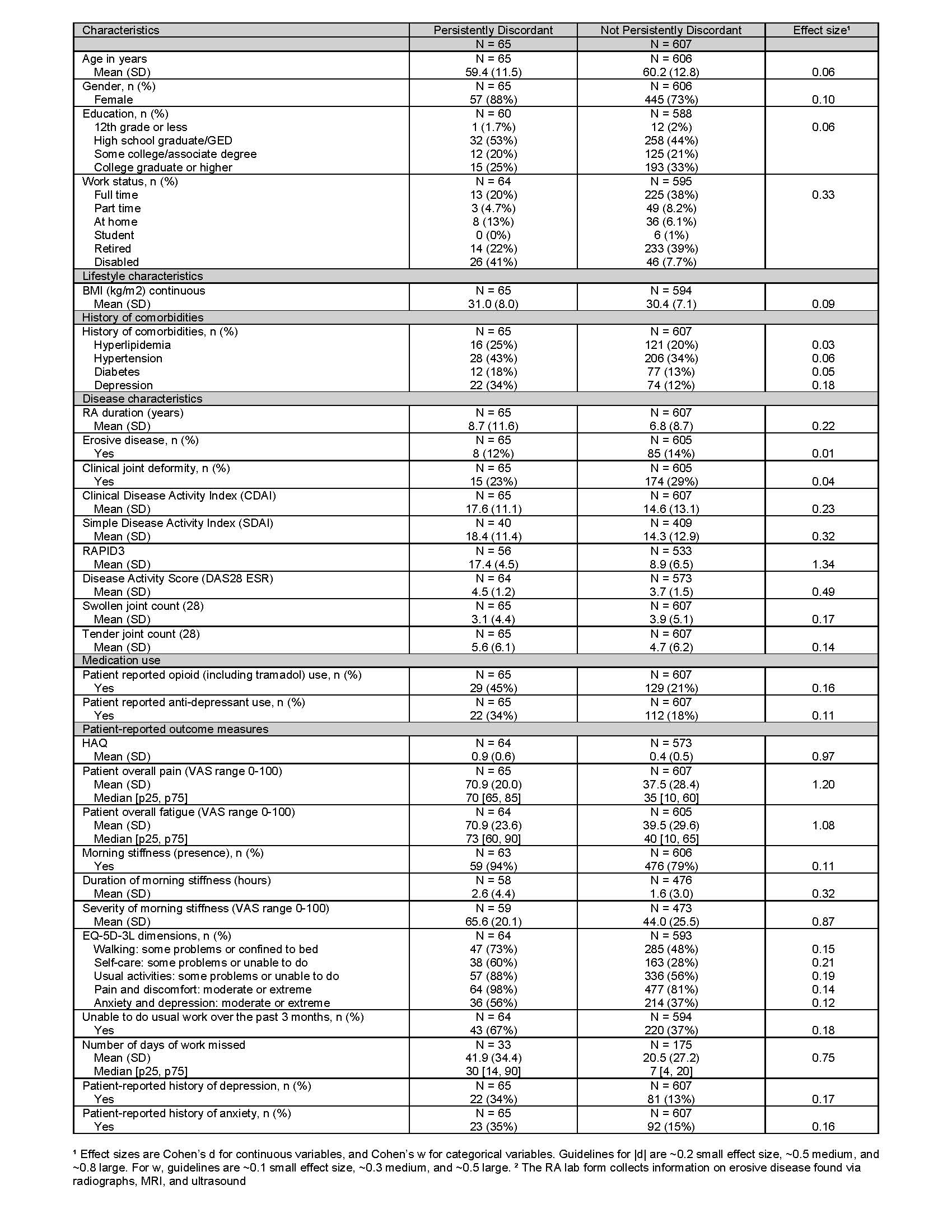 Table 2: Patient Demographics and Clinical Characteristics of Patients by Persistent Discordance Status
Table 2: Patient Demographics and Clinical Characteristics of Patients by Persistent Discordance Status
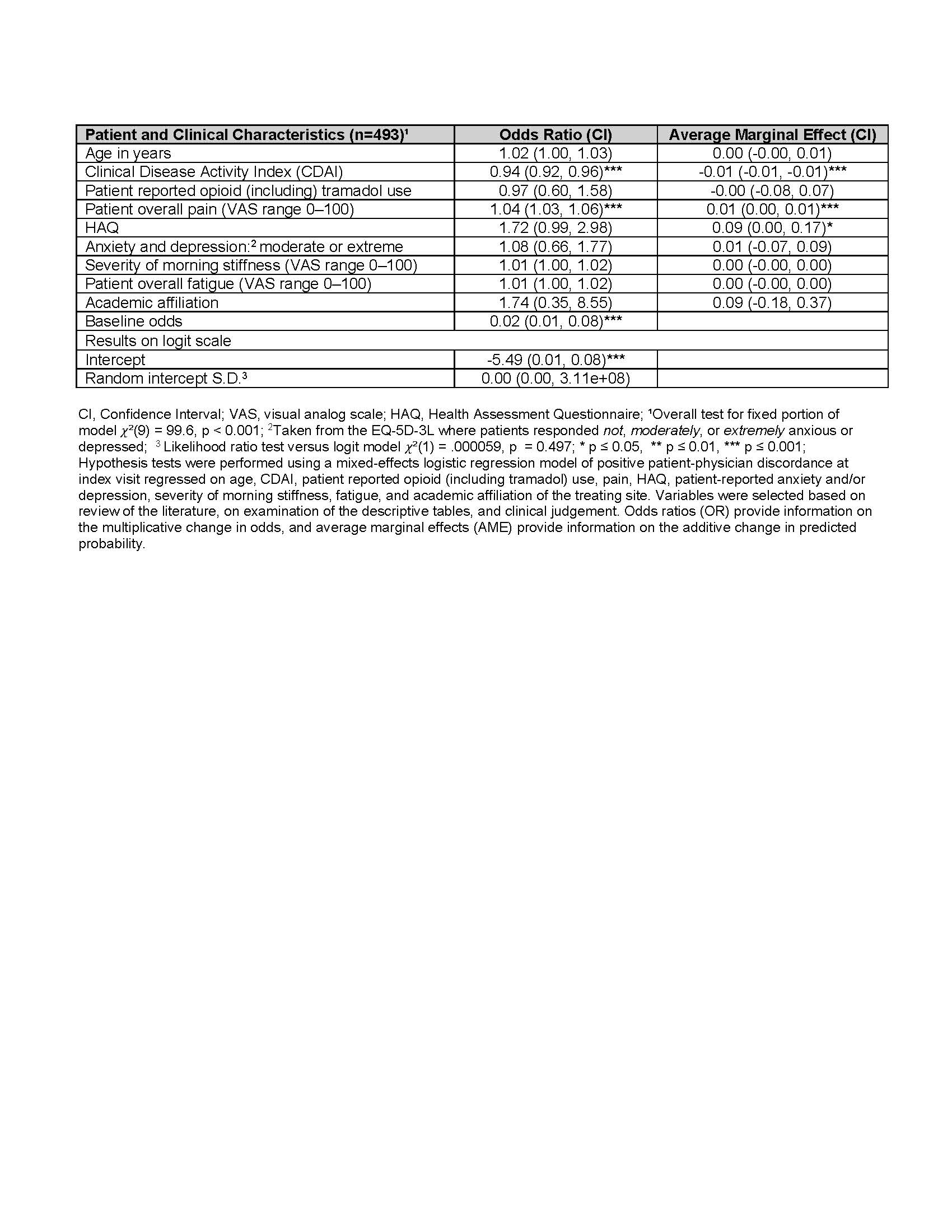 Table 3: Mixed-Effects Logistic Regression of Factors Associated with Positive Discordance (Referent to Concordance)
Table 3: Mixed-Effects Logistic Regression of Factors Associated with Positive Discordance (Referent to Concordance)
To cite this abstract in AMA style:
Curtis J, Medeiros R, Lee I, Mackey R, Haubrich R, Hu H, Greenberg J, Wu A. Prevalence and Factors Associated with Patient-Physician Discordance Among RA Patients Initiating Advanced Therapy [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/prevalence-and-factors-associated-with-patient-physician-discordance-among-ra-patients-initiating-advanced-therapy/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/prevalence-and-factors-associated-with-patient-physician-discordance-among-ra-patients-initiating-advanced-therapy/
