Session Information
Date: Sunday, November 13, 2016
Title: Rheumatoid Arthritis – Human Etiology and Pathogenesis - Poster I
Session Type: ACR Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: In rheumatoid arthritis (RA), bone erosions are caused mainly by osteoclasts. Osteoclasts are derived from monocytes and macrophages (MoMa). MoMa consists of different subtypes such as M1 and M2. Until now, little has been known regarding the relation of characteristic of RA with MoMa subtypes. We attempted to investigate relationship among MoMa subtypes (M1 or M2), ability of osteoclast differentiation, phagocytic ability of osteoclasts, and clinical characteristics in RA patients.
Methods: This study included 40 RA patients and 19 healthy donors. We collected baseline clinical variables including duration of disease, DAS28, positivity of rheumatoid factor (RF) and anti-cyclic citrullinated peptide antibody (ACPA), and treatments. Peripheral blood mononuclear cells (PBMC) were isolated from RA patients and healthy donors, then we investigated the number of M1/M2 cells by fluorescence-activated cell sorting. We defined M1 as CD14, CD68 and CCR2 positive cells and M2 as CD14, CX3CR1 and CD163 positive cells. We also obtained CD14 positive cells in PBMCs from RA patients and healthy donors using CD14 beads to investigate osteoclast differentiation in vitro with stimulation by macrophage colony stimulating factor (MCSF) and receptor activator of NF-ƒÈB ligand (RANKL). Osteoclast differentiation was evidenced by tartrate-resistant acid phosphatase (TRAP) staining, then we counted number of osteoclasts. We also performed pit formation assay of osteoclasts to assess phagocytic ability of osteoclasts.
Results: Twenty seven patients (68%) had positive RF. Twenty two patients (55%) were ACPA positive. Median M1 rate in CD14 positive cells was 18.5% (6.7%-39.9%, IQR). Median M2 rate in CD14 positive cells was 33.3% (13.2%-65.9%, IQR). Median M1/M2 ratio was 0.59 (0.31-1.11, IQR). There were no differences between RA patients and healthy donors, and between RA patients with high disease activity and low disease activity regarding M1/M2 ratio or number of osteoclasts in vitro, respectively. ACPA positive patients had higher M1/M2 ratio in vivo (0.87 vs. 0.41, p=0.028) (Figure 1A) and more number of osteoclasts in vitro (Figure 1B) than ACPA negative patients (97 per well vs. 37 per well, p=0.003). Furthermore, there was positive correlation between M1/M2 ratio and the number of differentiated osteoclasts in vitro in RA patients (ƒÏ=0.81, p<0.01) (Figure 1C). Overall, number of osteoclasts in vitro correlated with area of pit formation. There was no relationship among treatments (including methotrexate, prednisolone and biologics), M1/M2 ratio and number of osteoclasts in vitro.
Conclusion: The presence of ACPA positively correlated with the circulating osteoclast precursors in RA patients which may attributed to M1 subtypes. Our present data may explain the preferential development of bone destruction in ACPA-positive RA patients. 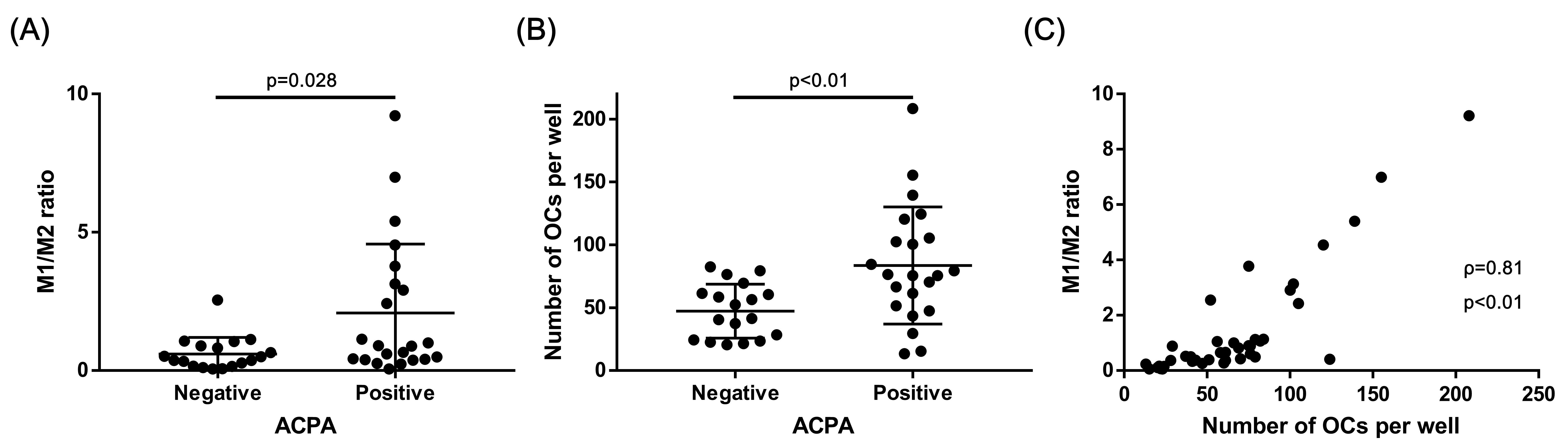
To cite this abstract in AMA style:
Fukui S, Iwamoto N, Shimizu T, Umeda M, Nishino A, Horai Y, Koga T, Kawashiri SY, Ichinose K, Hirai Y, Tamai M, Nakamura H, Origuchi T, Kawakami A. Preferential Distribution of M1 Monocytes in Anti-Cyclic Citrullinated Peptide Antibody Positive Patients with Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/preferential-distribution-of-m1-monocytes-in-anti-cyclic-citrullinated-peptide-antibody-positive-patients-with-rheumatoid-arthritis/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/preferential-distribution-of-m1-monocytes-in-anti-cyclic-citrullinated-peptide-antibody-positive-patients-with-rheumatoid-arthritis/
