Session Information
The 2020 Pediatric Rheumatology Symposium, originally scheduled for April 29 – May 2, was postponed due to COVID-19; therefore, abstracts were not presented as scheduled.
Date: Friday, May 1, 2020
Title: Poster Session 2
Session Type: ACR Abstract Session
Session Time: 5:00PM-6:00PM
Background/Purpose: Investigators have made significant progress piecing together pathogenic mechanisms of juvenile dermatomyositis (DM). However, this remains an incomplete puzzle, and optimal approaches to diagnosing, staging, and treating disease are yet to be determined. The ability to collect and store biospecimens and utilize advances in systems biology has enhanced biomarker discovery and brings closer the goal of completing the puzzle. In this pilot study, we analyze the serum metabolic profiles of patients with probable and definite juvenile DM prior to initiation of immunosuppressive treatment versus healthy control subjects to characterize the metabolic consequences of the pathogenic mechanisms involved in cellular and tissue injury in juvenile DM. Additionally, longitudinal analysis of untreated juvenile DM serum profiles versus profiles after treatment initiation was performed to determine whether the profile/putative biomarker informed treatment response.
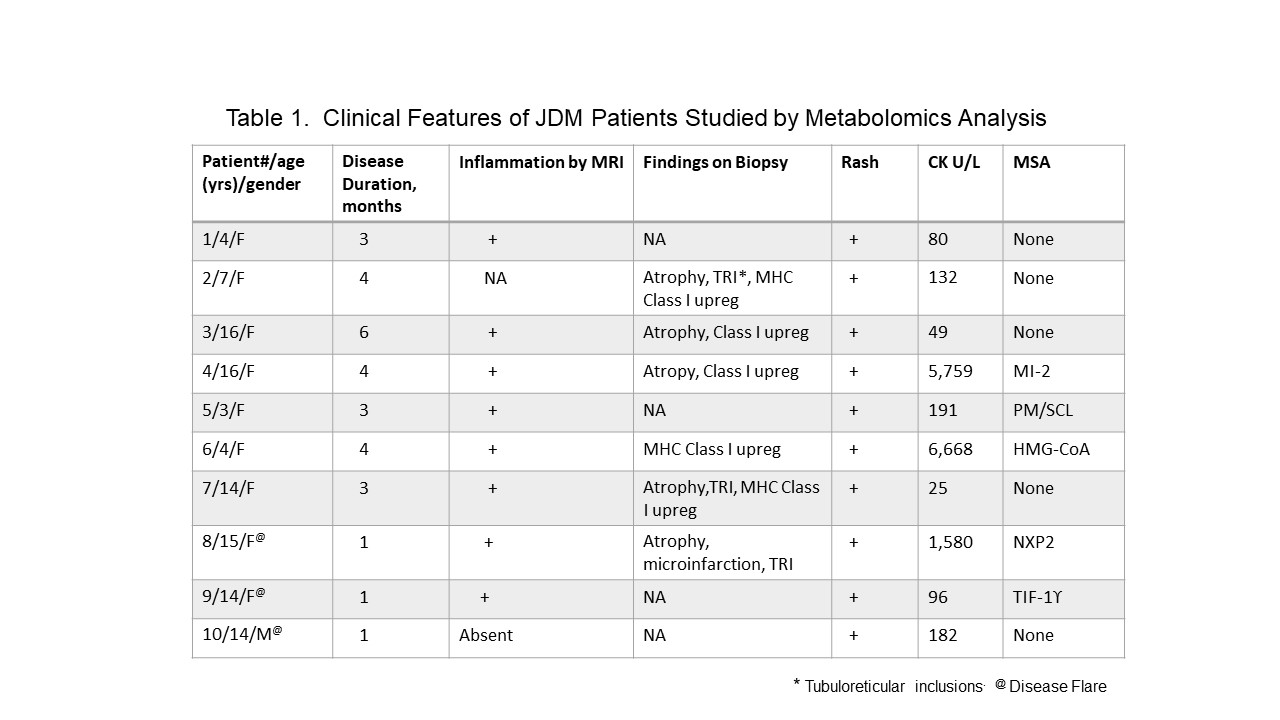
Methods: Metabolomic profiles were analyzed in serum samples from 10 patients with probable (N=4) or definite (N=6) juvenile DM. These 10 included 7 patients with newly diagnosed disease and 3 patients with a flare of previously diagnosed and treated disease after a medication-free remission greater than 8 months. These patients constituted the treatment naïve (TN) group. Clinical features of this group are shown in Table 1. Their profiles were compared to profiles of 9 gender- and age-matched subjects without inflammatory musculoskeletal disease or history of chronic disease, healthy controls (HC). Following initiation of immunosuppression, longitudinal serum profiles were obtained from 7 of the 10 patients for comparison with pre-treatment profiles. A targeted mass spectrometry-based platform was used to measure serum metabolites including acyl-carnitines (ACs), and ceramides (Cer). Principal components analysis (PCA) was used on log-transformed, standardized metabolite measurements separately to reduce the dimensionality of our data to a limited number of factors prior to t-tests for group comparisons.
Results: We identified 1 interpretable AC factor in our baseline analysis where the ACs loaded on factor 1 by 0.89 standard deviations greater TN compared to HC (p=0.49, Figure 1). For Cer factor 2, TN loaded greater than HC at p< 0.01. Baseline analysis of individual ACs and Cer from TN, identified significant associations (elevations) of serum ACs (predominantly long-chain ACs [LCACs]) and Cer when compared to HC serum (Table 2). Using PCA, a component score of these individual ACs and Cer was generated to see if there was a decline in values upon longitudinal analysis following conventional treatment of juvenile DM. Seven of 10 patients in the TN group had treatment samples available at time of analysis. There was a significant treatment effect for both the AC and Cer component with a mean decrease of -1.43 (p=0.03) and -0.924 (p< 0.01), respectively (Table 2).
Conclusion: This study has identified ACs and Cer as potential serum biomarkers of disease activity and response to treatment in patients with juvenile DM. The significant association of these metabolites with juvenile DM indicate a role for these lipids in the pathogenesis of juvenile DM.
To cite this abstract in AMA style:
Dvergsten J, Ilkayeva O, Landerman L, Muehlbauer M, Pisetsky D, Reed A, Huffman K. Metabolic Profiling in Juvenile Dermatomyositis [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 4). https://acrabstracts.org/abstract/metabolic-profiling-in-juvenile-dermatomyositis/. Accessed .« Back to 2020 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/metabolic-profiling-in-juvenile-dermatomyositis/