Session Information
Date: Tuesday, November 7, 2017
Title: Osteoarthritis – Clinical Aspects Poster II: Observational and Epidemiological Studies
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: Metabolic changes or low-grade inflammation related to cardiovascular disease (CVD) and diabetes have been hypothesized to contribute to the development of OA. Prior studies have demonstrated an association between diabetes and OA, and recognized OA as a risk factor for incident CVD. However, it remains unclear whether these associations are truly causal as they have not been confirmed in longitudinal cohort studies and may be explained by shared risk factors. The aim of the current study was therefore to examine the associations of pre-existing CVD and diabetes with incident knee OA.
Methods: The study sample consisted of Multicenter Osteoarthritis (MOST) Study participants. We used a self-administered modified Charlson comorbidity questionnaire to assess pre-existing CVD (heart attack, stroke, transient ischemic attack, heart or leg bypass surgery, treatment for heart failure) and diabetes in the participants at baseline. We assessed radiographic (ROA) and symptomatic (SxOA) knee OA at baseline and at 60-months follow-up. We defined ROA as Kellgren-Lawrence grade ≥ 2 on the knee radiograph, and SxOA as ROA and frequent knee pain in the same knee. While we primarily aimed to evaluate the effect of CVD and diabetes on development of knee OA, we recognize that such comorbidities are often chronic and their effects on OA may have already occurred in these older study subjects prior to their study entry. This could result in depletion of susceptibles in a study of their effects on incident knee OA. Therefore, we evaluated both the cross-sectional and longitudinal relation of CVD and diabetes to prevalent and incident ROA and SxOA using logistic regression. We adjusted the models for age, sex, race, body mass index (BMI), history of knee injury/surgery, physical activity, and correlation between knees within each participant.
Results: We included 5929 knees of 3014 participants in the baseline cross-sectional analyses (mean±SD age 62.5±8.1, mean BMI 30.8±6.0, 60% Caucasian) and 2317 knees of 1181 participants free of knee OA at baseline in the longitudinal analyses (mean±SD age 60.7±7.7, mean±SD BMI 29.1±4.7, 59% Caucasian). In cross-sectional analyses, CVD and diabetes were not associated with ROA and SxOA (Table). In longitudinal analyses, we also found no association of CVD or diabetes with incident ROA or SxOA (Table).
Conclusion: Self-reported CVD and diabetes were not associated with prevalent or incident knee ROA or SxOA after adjustment for potential confounders. Although some of our analyses had limited precision, our results suggest that that these common comorbidities do not appear to contribute to development of knee OA. Specific factors that may contribute to a metabolic OA phenotype require further evaluation.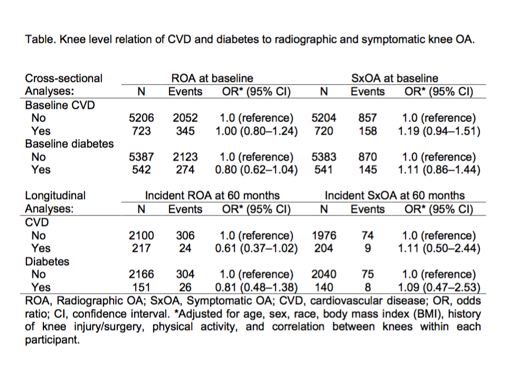
To cite this abstract in AMA style:
Kuusalo L, Felson DT, Brown C, Lewis CE, Torner J, Neogi T. Metabolic Osteoarthritis: Relation of Cardiovascular Disease and Diabetes to Knee Osteoarthritis [abstract]. Arthritis Rheumatol. 2017; 69 (suppl 10). https://acrabstracts.org/abstract/metabolic-osteoarthritis-relation-of-cardiovascular-disease-and-diabetes-to-knee-osteoarthritis/. Accessed .« Back to 2017 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/metabolic-osteoarthritis-relation-of-cardiovascular-disease-and-diabetes-to-knee-osteoarthritis/
