Session Information
Date: Tuesday, November 12, 2019
Title: RA – Diagnosis, Manifestations, & Outcomes Poster III: Comorbidities
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Interstitial lung disease (ILD) is a common and severe complication of rheumatoid arthritis (RA). It has been associated with the presence of ACPA. Anti-carbamylated peptides/proteins (anti-CarP) is a new family of RA autoantibodies associated with poor outcomes including an increased mortality due to respiratory disease (1). We aimed to analyze the prevalence of distinct anti-CarP fine specificities in an established RA cohort and determined whether anti-CarP are associated with ILD.
Methods: Cross sectional study. Patients with RA according to ACR/EULAR 2010 criteria with a disease duration of ≤ 10 years, and those with an associated ILD independently of the disease duration were included. ILD was diagnosed with a high-resolution CT according the American Thoracic Society/European Respiratory Society 2013 criteria, diagnosis confirmed by a multi-disciplinary committee. Demographic, clinical and radiological features were analyzed. Auto-antibody status (RF and ACPA) were also assessed. Three anti-CarP IgG autoantibodies were determined (anti-CarP fetal calf serum (FCS), anti-CarP fibrinogen (anti-Fib) and anti-CarP fibrine/filagrine homocitrulinated peptide (anti-CFFHP)) by home-made ELISA tests using as antigens either carbamylated proteins or a synthetic chimeric fibrin-filaggrin homocitrullinated peptide. Cut-off values were determined using ROC curves, with a specificity of 96% compared with a healthy population.
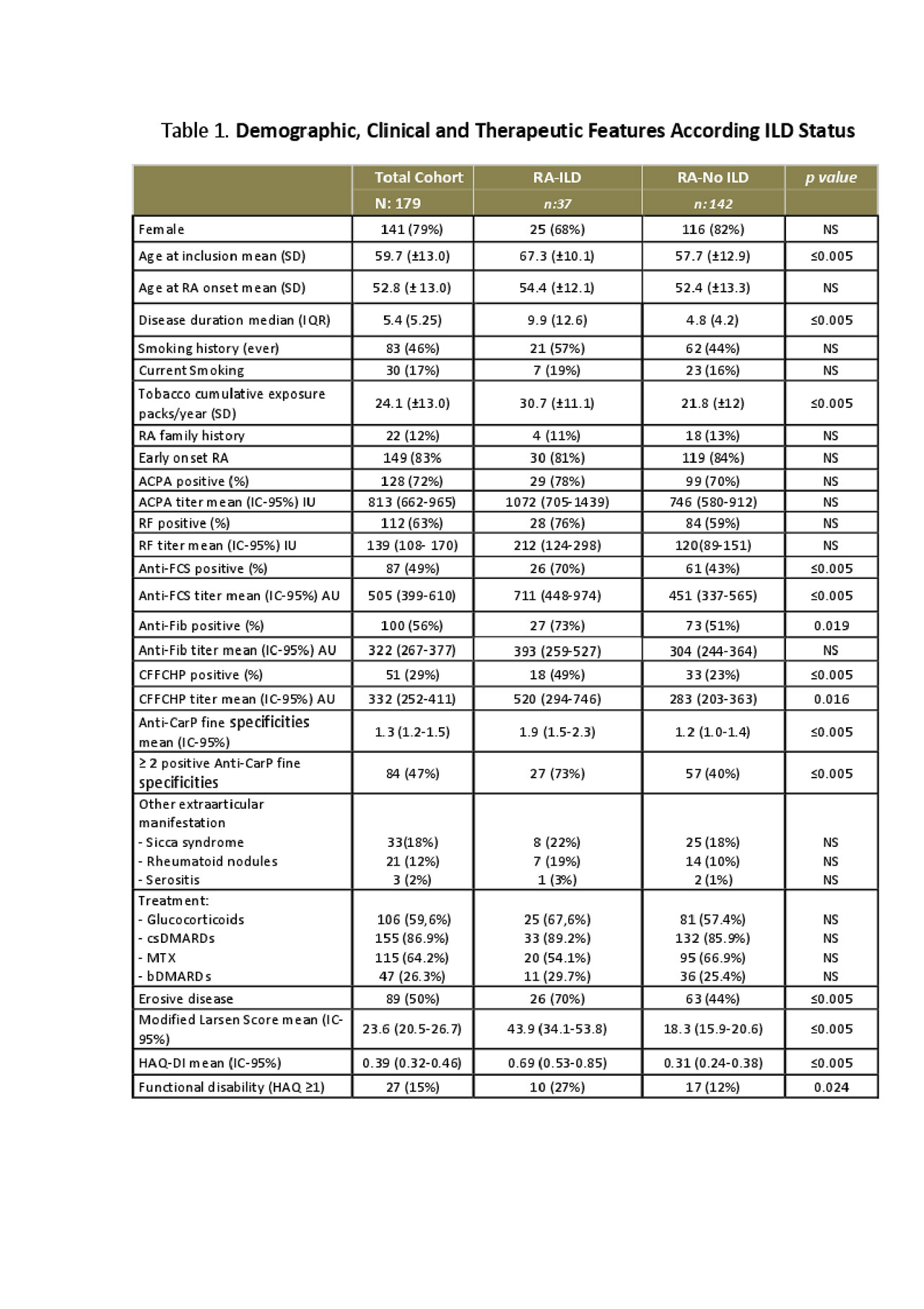
Results: 179 patients were included, 21% had an ILD. The mean age at ILD diagnosis was 64.2 (±9.7) years, the mean time from RA diagnosis until ILD diagnosis was 9.3 (IQR: 11.4) years. A significantly greater tobacco exposure (30.7 ±11.1 vs 21.8 ±12) and higher frequency of erosive disease (70% vs 44%) and disability (HAQ-DI >1: 27% vs 12%) was observed in patients with ILD. Total cohort demographic, clinical and radiological features are presented in Table 1.
Anti-CarPs prevalence in the total cohort was 49%, 56%, and 29% for anti-FCS, anti-Fib and anti-CFFHP peptide respectively. Positive Anti-FCS anti-Fib and anti-CFFHP peptide were found in 22%, 29% and 8% of ACPA negative patients respectively.
All anti-CarP fine specificities were significantly more prevalent in patients with ILD (anti-FCS 70% vs 43%; anti-Fib 73% vs 51%; anti-CFFHP 49% vs 23%), and significantly higher titers of Anti-FCS and anti-CFFCHP were observed in these patients.
A logistic regression model adjusted for age, disease duration, sex, smoking, erosive disease, RF and ACPA demonstrated that Anti-FCS (OR: 3.49; CI 95%: 1.16-10.50) and anti-CFFHP (OR: 4.82; CI 95%: 1.56-14.9) were independently associated with ILD.
Conclusion: In our cohort, the presence of anti-CarP ranges between 29-56% according to the antigenic specificity used. These autoantibodies were associated with ILD. Anti-CarP could be considered a more specific biomarker of ILD in patients with RA rather than ACPA.
Reference
1. Vidal-Bralo L. Anti-carbamylated protein autoantibodies associated with mortality in Spanish rheumatoid arthritis patients. PLOS ONE. 2017;12(7):e0180144.
To cite this abstract in AMA style:
Castellanos-Moreira R, Rodriguez-Garcia S, Ruiz-Esquide V, Hernández-González F, Sánchez M, Ramírez J, Benegas M, Lucena-Pozo C, Agustí C, Boada M, Viñas O, Ruiz E, Prieto-González S, Gomez-Puerta J, Sellares J, Cañete J, Haro I, Sanmarti R. Interstitial Lung Disease Is Associated with Distinct Fine Specificities of Anti-Carbamylated Peptide/Protein Antibodies in Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/interstitial-lung-disease-is-associated-with-distinct-fine-specificities-of-anti-carbamylated-peptide-protein-antibodies-in-rheumatoid-arthritis/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/interstitial-lung-disease-is-associated-with-distinct-fine-specificities-of-anti-carbamylated-peptide-protein-antibodies-in-rheumatoid-arthritis/