Session Information
Date: Wednesday, October 24, 2018
Title: 6W009 ACR Abstract: RA–Etiology & Pathogenesis II (2898–2903)
Session Type: ACR Concurrent Abstract Session
Session Time: 9:00AM-10:30AM
Background/Purpose: The inability to identify relevant arthritogenic CD4 T cells in patients and in murine disease models has limited our understanding of disease initiating events in rheumatoid arthritis (RA). To overcome this limitation, we took advantage of the dynamic expression pattern of Nur77 (Nr4a1)—a sensitive and specific marker of TCR signaling that is insensitive to cytokine stimulation—to identify antigen-activated CD4 T cells in human RA and the SKG mouse model of autoimmune arthritis.
Methods: We used intracellular flow cytometry to identify T cells that express Nur77 protein in synovial tissue and blood from patients with seropositive RA or osteoarthritis (OA), as well as in the SKG arthritis model. A fluorescent reporter (eGFP) of Nur77 expression was backcrossed into SKG mice (SKGNur) to identify and study arthritogenic T cells in this model. Functional and signaling differences between CD4 T cells that expressed the highest and lowest amounts of eGFP (GFPhi and GFPlo, respectively) were compared using in vitro assays, adoptive transfer, and gene expression assays. We searched general public repository databases for available transcriptome data from human RA synovium (13 studies met inclusion criteria comprising over 300 synovial samples) to examine candidate gene expression profiles.
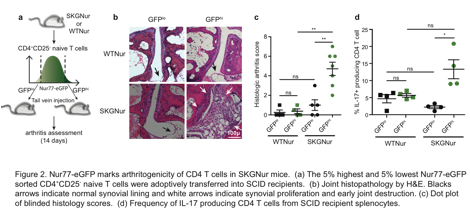
Results: Nur77 expression was specifically enriched in a subset of synovial CD4 T cells from patients with RA (Fig 1). This suggested the presence of antigen-activated T cells in RA synovial tissue. This was confirmed in the SKG mouse. Higher levels of Nur77-eGFP (GFPhi) in SKGNur CD4 T cells marked their autoreactivity and arthritogenic potential and their ability to more readily differentiate into IL-17 producing cells (Fig 2). T cells exhibiting this heightened autoreactivity still had diminished TCR signaling, perhaps due to upregulation of inhibitory receptors. Moreover, the enhanced autoreactivity was associated with upregulation of IL-6 cytokine signaling machinery, but a reduced amount of expression of suppressor of cytokine signaling 3 (SOCS3)—a key negative regulator of IL-6 signaling. As a result, the more autoreactive GFPhi CD4 T cell population from SKGNur mice was uniquely hyper-responsive to IL-6. Consistent with findings from SKGNur mice, SOCS3 expression was similarly downregulated in RA synovium.
Conclusion: This suggests that, despite impaired TCR signaling, autoreactive T cells exposed to chronic antigen stimulation exhibit heightened sensitivity to IL-6 receptor signaling which contributes to their arthritogenicity in SKG mice, and perhaps in patients with RA.
To cite this abstract in AMA style:
Ashouri J, Hsu LY, Rychkov D, Sirota M, Lattanza L, Hansen E, Zikherman J, Weiss A. Impaired TCR Signaling Paves the Way for Cytokine Hyper-Responsiveness in Arthritogenic T Cells [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/impaired-tcr-signaling-paves-the-way-for-cytokine-hyper-responsiveness-in-arthritogenic-t-cells/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/impaired-tcr-signaling-paves-the-way-for-cytokine-hyper-responsiveness-in-arthritogenic-t-cells/