Session Information
Date: Saturday, November 6, 2021
Title: RA – Diagnosis, Manifestations, & Outcomes Poster I: Cardiovascular Pulmonary Disease (0268–0295)
Session Type: Poster Session A
Session Time: 8:30AM-10:30AM
Background/Purpose: Statins and bDMARDs may decrease cardiovascular risk in RA by lowering coronary plaque formation, promoting regression and altering the composition of atherosclerotic lesions. Macrophage cholesterol loading capacity (CLC) of serum is a functional parameter reflecting both quality and quantity of lipoproteins and is potentially related to foam cell formation. We evaluated the associations between CLC, coronary plaque burden and cardiovascular (CVD) risk in patients with RA. We further explored the moderating effects of RA treatments on these relationships.
Methods: 107 patients with baseline coronary CT angiography for atherosclerosis evaluation and prospective follow-up for cardiovascular events over 6.0±2.4 years were studied. Coronary artery calcium score (CAC), number of segments with plaque and plaque composition were assessed. CLC was the macrophage cholesterol content, measured by fluorometric assay, after a 24 hour incubation with whole serum. Adjusted robust Cox regression evaluated main effects and interactions of CLC with bDMARD and statin treatment duration on event risk. Robust linear regression examined the interaction between CLC and bDMARD therapy on CAC burden. Robust negative binomial regressions evaluated interactions between CLC and bDMARD exposure on total and high-risk low-attenuation plaque (LAP) burden.
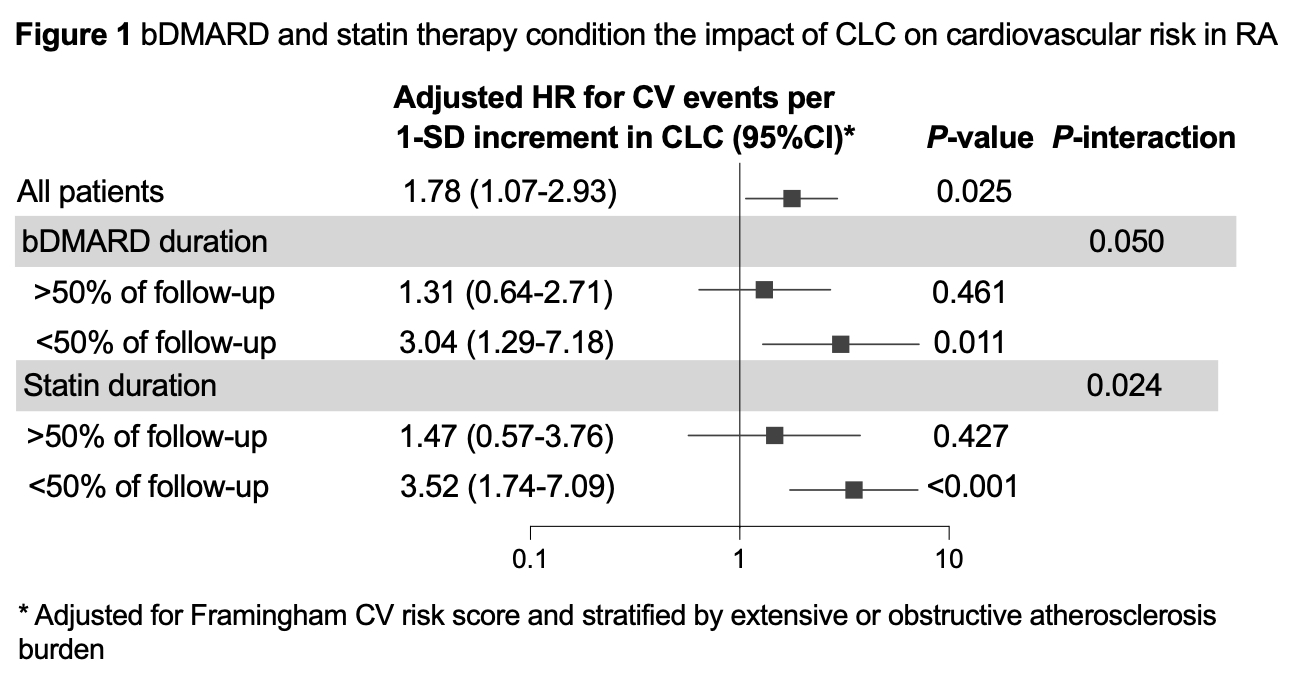
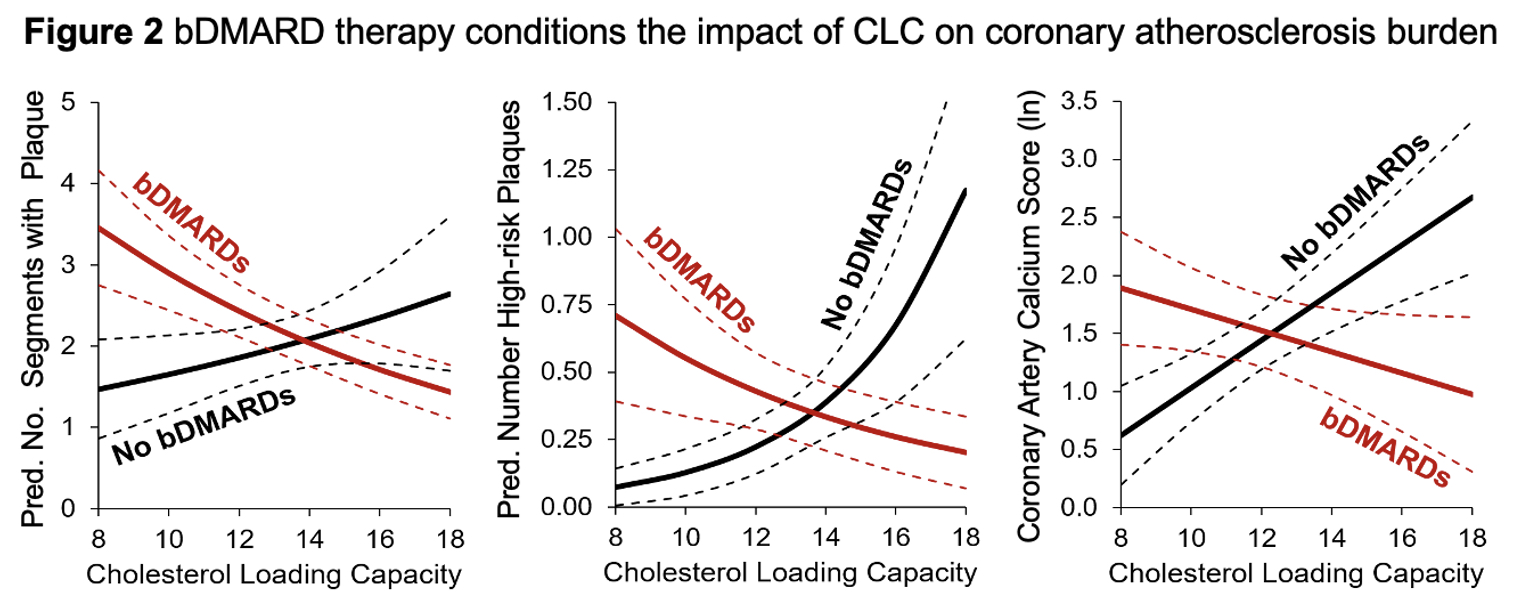
Results: CLC associated with incident CVD risk (per SD increment; adjusted hazard ratio [aHR] 1.78 [95% CI 1.07-2.93], P=0.025), after accounting for Framingham CVD score and baseline atherosclerosis burden. The effect was stronger in patients with less exposure to bDMARDs (< 50% of follow-up: aHR 3.04 [95% CI 1.29-7.18]; versus >50% of follow-up: aHR 1.31 [95% CI 0.64-2.71], Fig. 1) and statins (< 50% of follow-up: aHR 3.52 [95% CI 1.74-7.09]; versus >50% of follow-up: aHR 1.47 [95% CI 0.57-3.76], Fig. 1). In cross-sectional analyses adjusting for Framingham CVD score and DAS28-CRP, CLC (per 1-SD unit) was not related to number of segments with plaque (adjusted rate ratio [aRR] 0.91 [95% CI 0.74-1.13]), number of vulnerable plaques (aRR 1.03 [95% CI 0.64-1.66]) or ln-transformed CAC (β -0.01 [95% CI -0.15-0.14]). However, in analyses stratified by baseline bDMARD use, CLC (per 1-SD unit) was positively related to number of vulnerable plaques (aRR 2.30 [95% CI 1.16-4.57]) and ln-transformed CAC (β 0.27 [95% CI 0.03-0.50]) among bDMARD naïve individuals (Fig. 2). In addition, CLC inversely associated with number of segments with plaque (per SD increment; aRR 0.76 [95% CI 0.61-0.94]) only in bDMARD exposed patients (Fig. 2).Baseline statin use did not significantly modify the effect of CLC on baseline coronary plaque (data not shown).
Conclusion: We showed for the first time that enhanced cholesterol loading onto macrophages (CLC) in RA associated with greater cardiovascular risk; this risk was modified by statin and bDMARD use. CLC further associated with greater CAC score and LAP burden in bDMARD-naïve but not bDMARD-treated patients. The negative association of CLC with total plaque burden in bDMARD-treated patients may reflect lower plaque formation and reduction in atherogenic lipoprotein disposal through vessels.
To cite this abstract in AMA style:
Karpouzas G, Papotti B, ormseth s, Palumbo M, Hernandez E, Marchi C, Zimetti F, Budoff M, Bernini F, Ronda N. Impact of Macrophage Cholesterol Loading Capacity and Interactions with Treatments on Cardiovascular Risk and Coronary Atherosclerosis Burden in Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/impact-of-macrophage-cholesterol-loading-capacity-and-interactions-with-treatments-on-cardiovascular-risk-and-coronary-atherosclerosis-burden-in-rheumatoid-arthritis/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/impact-of-macrophage-cholesterol-loading-capacity-and-interactions-with-treatments-on-cardiovascular-risk-and-coronary-atherosclerosis-burden-in-rheumatoid-arthritis/