Session Information
Session Type: Poster Session D
Session Time: 8:30AM-10:30AM
Background/Purpose: There is a need to understand which patients with rheumatologic diseases may be at highest risk for poor COVID-19 related outcomes so that both physicians and patients can make informed decisions regarding disease management and pandemic-related precautions. Routine assessment of patient index data 3 (RAPID3) is a quick tool to assess disease activity that has been validated in numerous rheumatologic conditions. Here, we evaluate the association between RAPID3 and other comorbidities with COVID-19 related outcomes in a cohort of rheumatology patients treated at an urban academic medical center.
Methods: The department of rheumatology COVID-19 data repository is an IRB approved registry consisting of patients at an academic center with both a COVID-19 diagnosis and a rheumatologic condition. Data collected included demographics, comorbidities, and disease activity as measured by the RAPID3. Chi-square and paired t-tests and logistic regression models were used to analyze associations between demographics, comorbidities, disease activity and COVID-19 hospitalization rates and recovery.
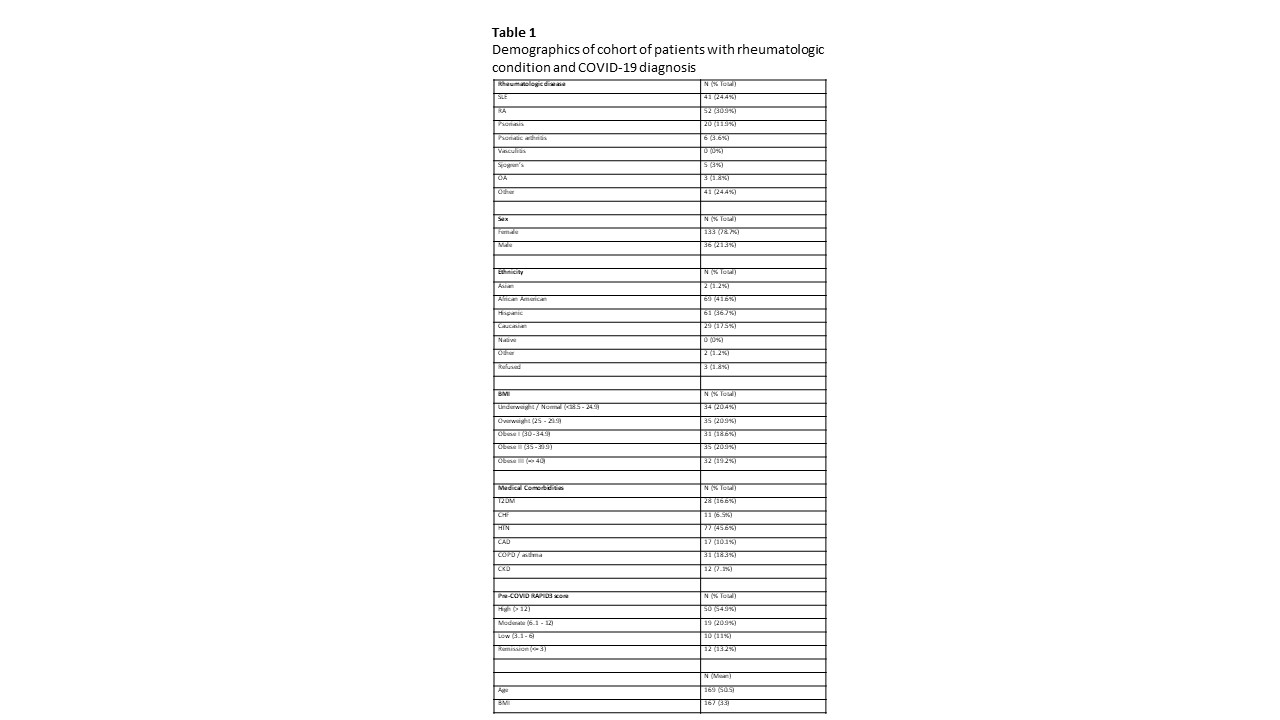
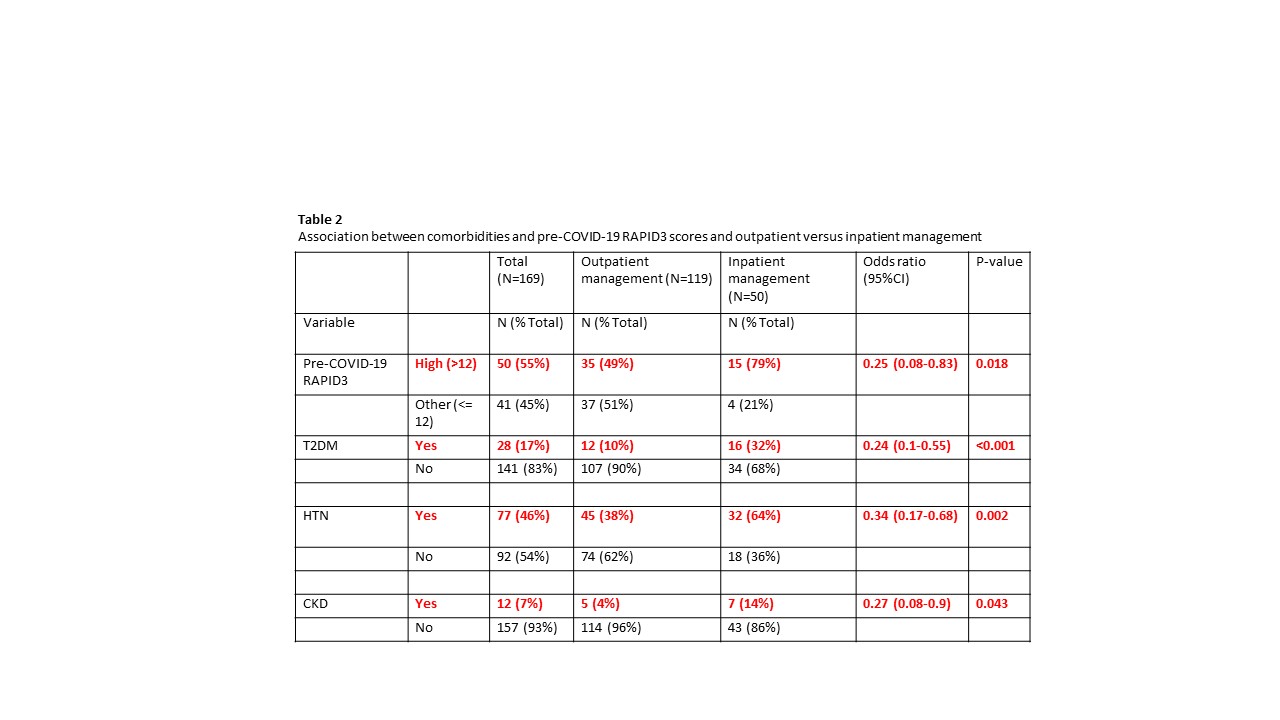
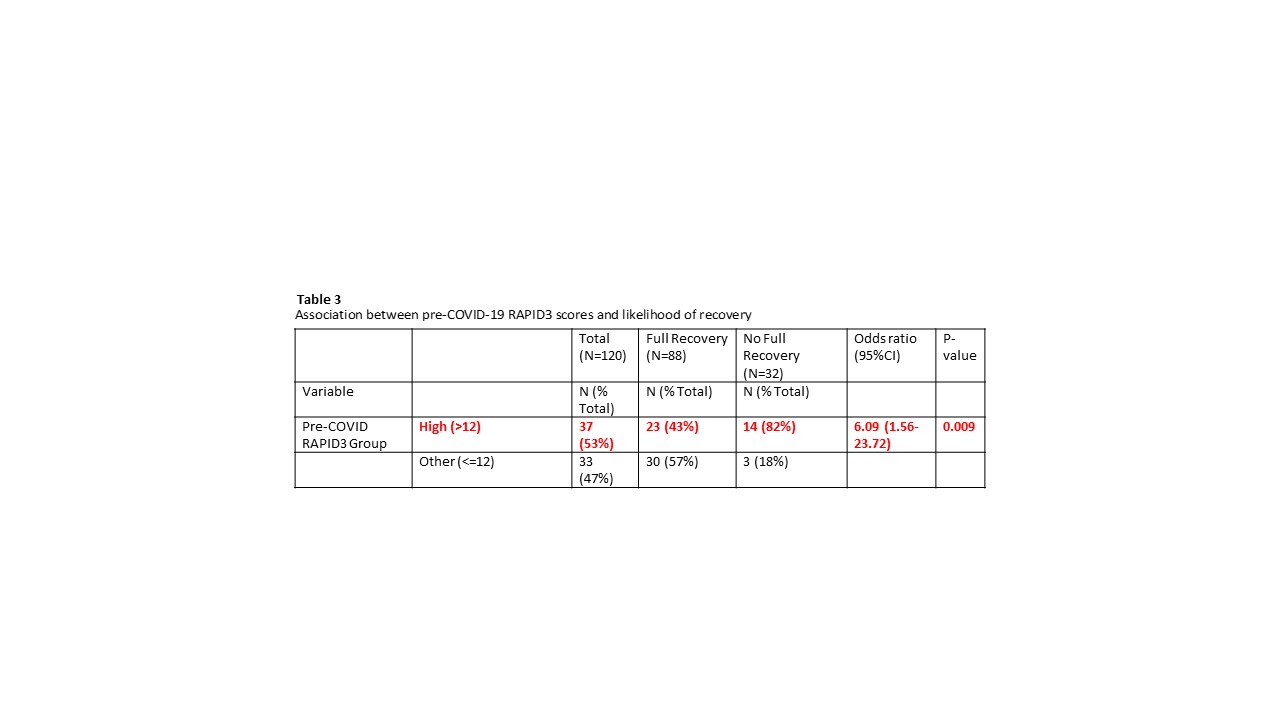
Results: 169 patients with a laboratory confirmed diagnosis of COVID-19 were included. Demographics are summarized in Table 1. The majority of patients had high or moderate pre-COVID-19 RAPID3 scores. In our analysis, increased age, T2DM, HTN, chronic kidney disease (CKD), and high pre-COVID-19 RAPID3 score were associated with higher odds of COVID-19 infection requiring hospitalization (Table 2). High pre-COVID-19 RAPID3 scores were also associated with lower odds of full recovery (Table 3).
HTN and CKD were associated with higher odds of intensive care (ICU) admission (HTN OR 5.8, CI 1.6-21.1, p 0.007; CKD OR 5.8, CI 1.5-22.1, p 0.02) and intubation (HTN OR 10.9, CI 1.3-89.3, p 0.01; CKD OR 7.8, CI 1.6-36.9, p 0.02). HTN was also associated with an increase in length of stay (14.9 days vs 6.6 days, p 0.01).
Conclusion: In this cohort of rheumatology patients, high pre-COVID-19 disease activity, as assessed by RAPID3 scores, was associated with increased odds of COVID-19 infection requiring hospitalization and decreased odds of full recovery. To our knowledge, this is the first study to use an exclusively patient-reported outcome tool to demonstrate the relationship between disease activity and COVID-19 outcomes in patients with rheumatic disease.
Similar to other studies, age, HTN, T2DM, and CKD were associated with severe COVID-19 outcomes. In contrast to previously described cohorts, this group is younger, predominantly female, and consists of a high proportion of Hispanic and Black patients.
To cite this abstract in AMA style:
Orentas M, Khandelwal S, Grant M, Zhang Y, Shakoor N, Hassan S. High Disease Activity, as Assessed by RAPID3, Increases Risk of Hospitalization and Predicts Lower Chance of Recovery from COVID-19 in a Cohort of Tertiary Care Rheumatology Patients [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/high-disease-activity-as-assessed-by-rapid3-increases-risk-of-hospitalization-and-predicts-lower-chance-of-recovery-from-covid-19-in-a-cohort-of-tertiary-care-rheumatology-patients/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/high-disease-activity-as-assessed-by-rapid3-increases-risk-of-hospitalization-and-predicts-lower-chance-of-recovery-from-covid-19-in-a-cohort-of-tertiary-care-rheumatology-patients/