Session Information
Date: Tuesday, November 12, 2019
Title: Patient Outcomes, Preferences, & Attitudes Poster II: Patient Preferences, Beliefs, & Experiences
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Rheumatoid arthritis (RA) exerts multifaceted burden through medical expenditures, productivity losses, disability, and intangible costs of pain, fatigue, and loss of functional capacity. Patient preference measures how they value a health outcome and it can be elicited by the trade-offs they place on different levels of the health outcomes. The study objective was to evaluate patients’ preferences for pain/fatigue, functional capacity, disability and joint replacement surgery, employment losses, and out-of-pocket cost using a discrete choice experiment (DCE).
Methods: A DCE was conducted in a prospective cohort of adult (18+ years) RA patients on methotrexate treatment, identified from the member population of Kaiser Permanente Southern California health plan. The web-based DCE survey varied the following 5 conjoint attributes with 3 levels in each: (1) Joint pain, swelling and tiredness (None, Moderate, Severe) (2) Limitations in daily activities (None, Moderate, Severe) (3) Chances of being disabled and require joint replacement surgery (Low (5%); Medium (40%), High (90%)) (4) Number of days missed work due to RA (1 day/month, 8 days/month, 24 days/month) (5) Out of pocket treatment cost ($20/Month, $500/Month, $2,500/Month). After initial pilot testing, graphical representation of levels was used to convey magnitude to patients. The choice profiles for each respondent were randomly sampled from the full-choice design ensuring level balance and near-orthogonality within each respondent’s profile. After completing 2 training tasks (not analyzed), each respondent completed 12 random choice tasks that provided trade-offs to varying levels of the 5 outcomes. Hierarchical Bayesian models were used to evaluate individual patient preferences accounting for inter-patient heterogeneity.
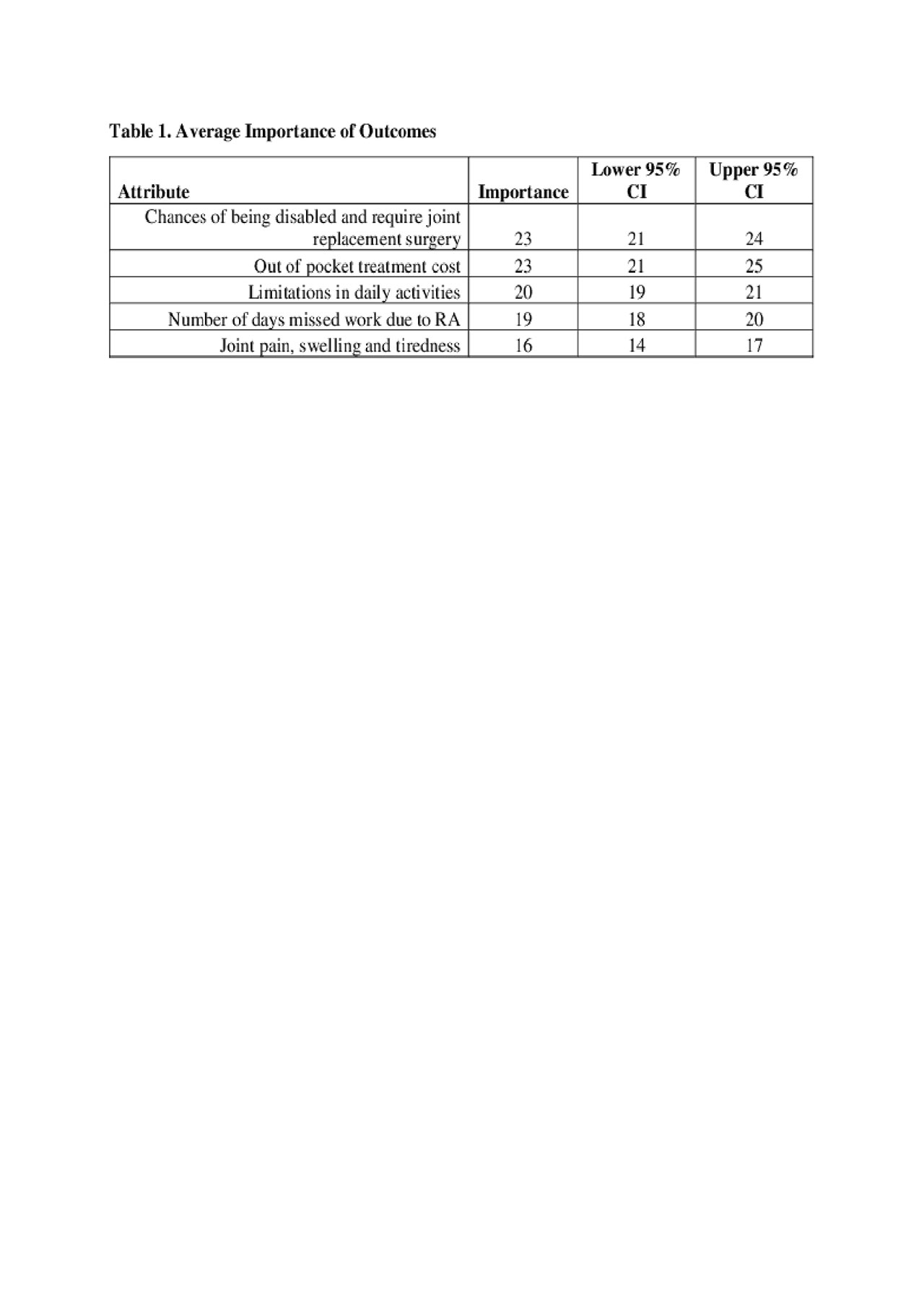
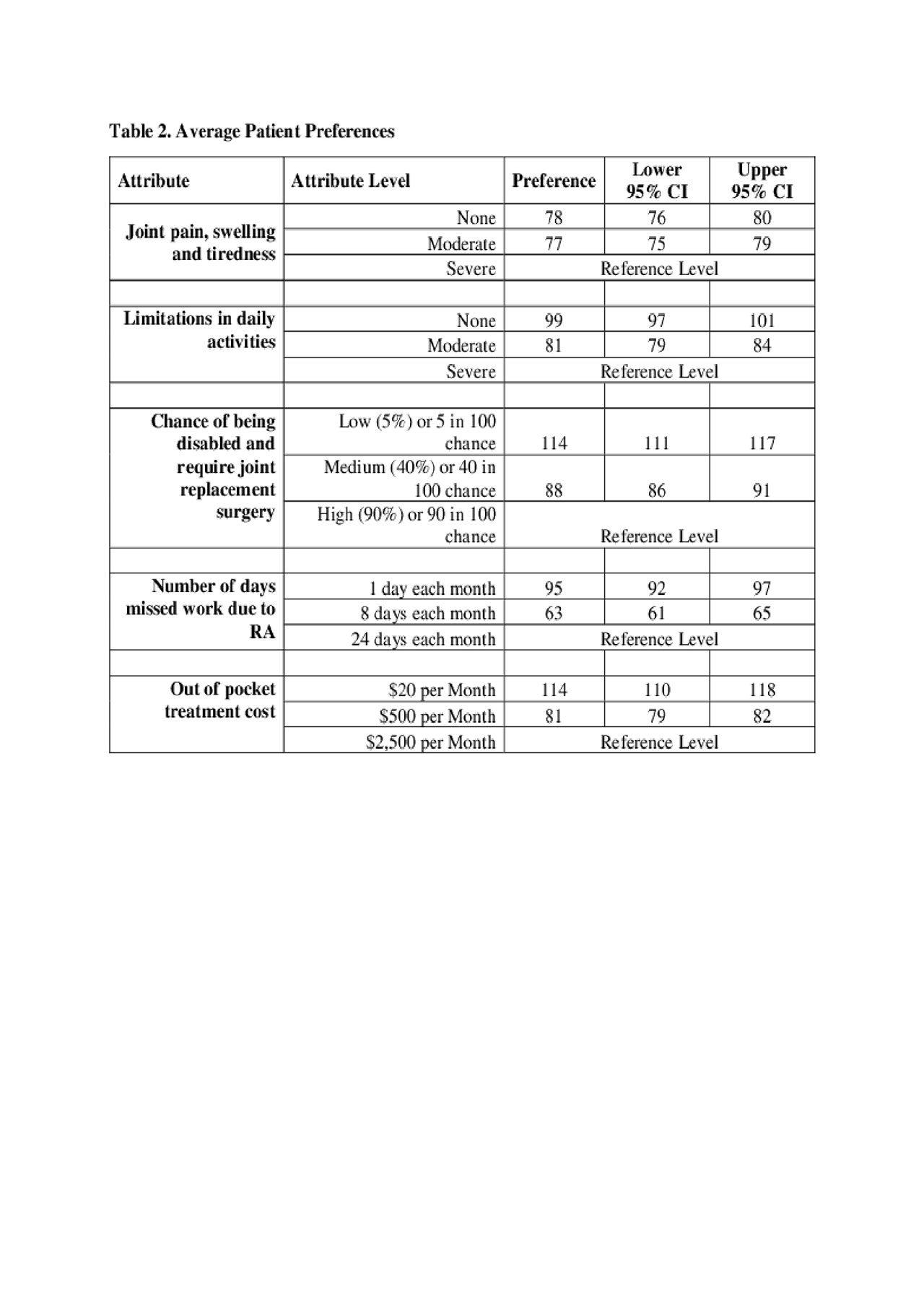
Results: The DCE completion rate was 53% (237/448) and the mean age of the sample was 53 (±16) years with the majority (84%) of female. Of the 5 attributes, chance of disability and joint replacement surgery was tied with out-of-pocket treatment cost as the most important attributes (Table 1) and loss in functional capacity was deemed more important compared to missing work and pain/tiredness. The average preference was 114 (95% CI 111-117) higher for low (5%) vs. high (90%) chance of being disabled and require joint replacement surgery (Table 2). In contrast, the average preference of moderate vs. no joint pain, swelling and tiredness was just one-unit difference (Table 2).
Conclusion: Treat-to-target approach based on swelling/tenderness/pain activity indices can be made more effective by shared decision making to incorporate patient preferences which value functional capacity and treatment cost higher. Better understanding of patient preferences can inform gaps in the existing evidence-base to inform practice guidelines.
To cite this abstract in AMA style:
Kawatkar A. Evaluation of Rheumatoid Arthritis Patients’ Preferences Using Discrete Choice Experiment [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/evaluation-of-rheumatoid-arthritis-patients-preferences-using-discrete-choice-experiment/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/evaluation-of-rheumatoid-arthritis-patients-preferences-using-discrete-choice-experiment/