Session Information
Session Type: Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose: Computed tomography (CT) has a higher sensitivity for the detection of intraarticular mineralization in comparison with commonly used imaging techniques in knee osteoarthritis (OA) including radiographs and MRI. The role of intra-articular mineralization in knee OA has been unclear, contributed to by inadequate imaging assessment of this phenomenon. The aim of this study is to report the prevalence of CT-detected intra-articular mineralization in older adults with or at risk of knee OA.
Methods: We used data from the Multicenter Osteoarthritis (MOST) Study, a NIH-funded cohort of people with or at risk of knee OA. The existing cohort was recruited in 2003-2005 (age 50-79), with the current analysis focusing on the 12th-year visit as the baseline for this analysis as this was the first study visit at which bilateral dual energy knee CTs were obtained. In addition coinciding with the 12th year study visit in 2016-2017, a new cohort was recruited (age 45-69) who had Kellgren Lawrence (KL) grade < =2 in both knees, and either no knee pain or if they had knee pain, it could not be severe or constant. Participants also had bilateral PA knee radiographs obtained, scored for KL grade by a musculoskeletal radiologist blinded to the CTs. A separate musculoskeletal radiologist scored multiplanar CT images using an ordinal score (0-3) for degree of mineralization in each of the MOAKS subregions of cartilage and menisci, as well as ligaments, capsule, and vasculature. Prevalence of intra-articular mineralization was computed for the total sample, and stratified by age and KL grade.
Results: The existing cohort included 635 subjects (1270 knees) (57.3 % female, mean age 71.8, mean BMI 29.9). The new cohort included 1473 subjects (2946 knees) (56 % female, mean age 56.6, mean BMI 28.4). CT-detected intra-articular mineralization (of either cartilage, meniscus, and/or capsule) was 23.3% in the existing cohort and 4.9% in the new cohort. For the existing cohort, the prevalence in specific locations was: 16.7% articular cartilage (vs. 3.6% in the new cohort), 19.5% meniscus (vs. 3.5% in the new cohort), and 12% capsule (vs. 1.5% in the new cohort). Articular and meniscal mineralization increased with age and was most prevalent in KL grade 2, both for the existing and new cohorts (Figure). The prevalence of intra-articular mineralization among KL grade 3 and 4 was lower in comparison with KL grade 2 in the existing cohort, though this was unadjusted for age and could reflect less cartilage present at higher KL grades to allow for mineralization to be detected. Overall, the prevalence of vascular calcifications was 52.9% in the existing cohort (vs. 19.9% for the new cohort), which increased with age in both cohorts.
Conclusion: CT provides good visualization of intra-articular mineralization within the hyaline articular cartilage, meniscus, and soft tissue, which will provide novel opportunities to evaluate the longitudinal relation of intra-articular mineralization to adjacent articular tissue pathology and overall OA progression.
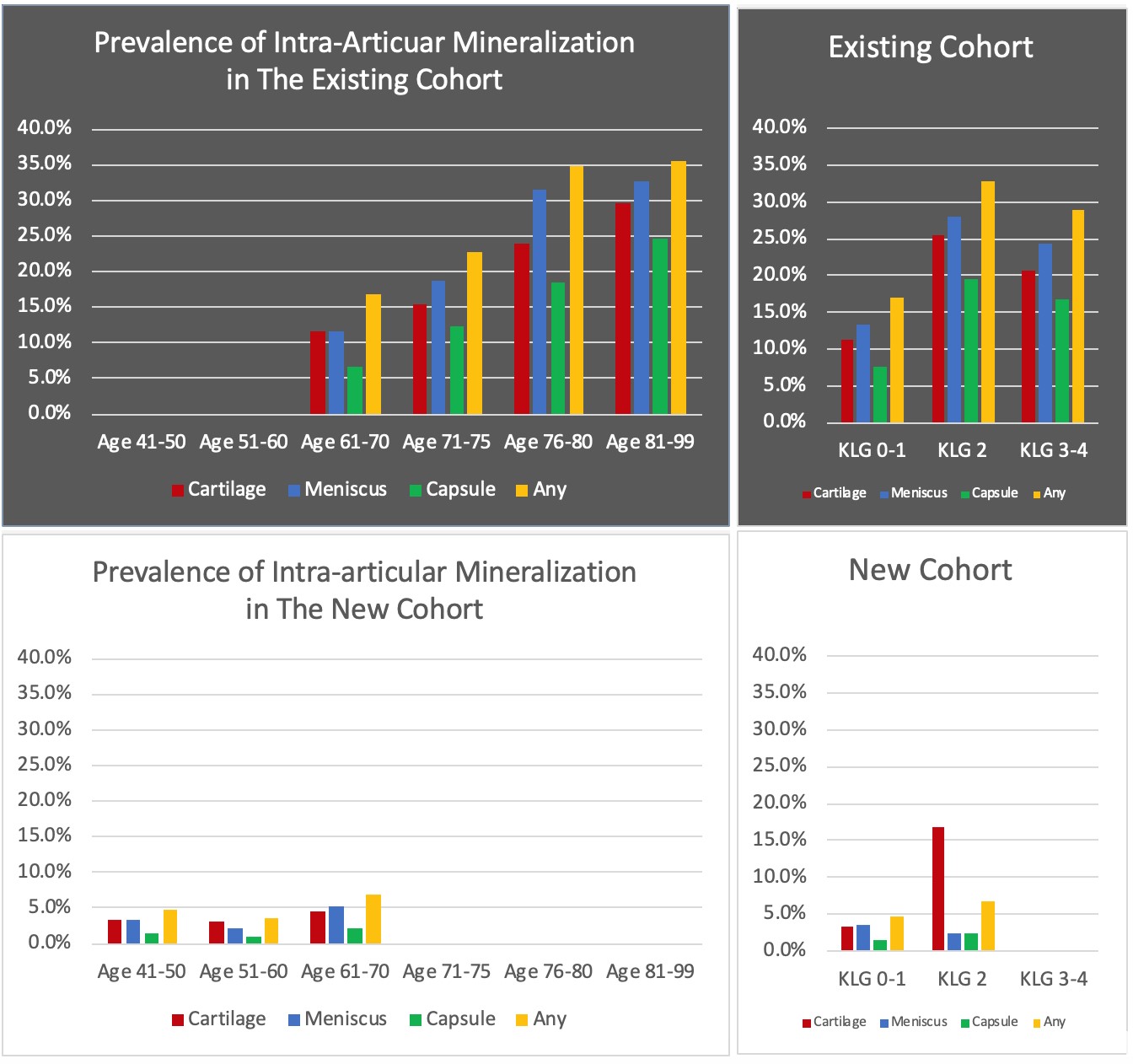 Prevalence of Intra-Articular Mineralization in the Existing and New Cohorts of the MOST Study
Prevalence of Intra-Articular Mineralization in the Existing and New Cohorts of the MOST Study
To cite this abstract in AMA style:
Jarraya M, Neogi T, Lynch J, Felson D, Aliabadi P, Nevitt M, Lewis C, Torner J, Guermazi A. Epidemiology of Intra-Articular Mineralization on Knee Dual-Energy Computed Tomography: The Multicenter Osteoarthritis Study [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/epidemiology-of-intra-articular-mineralization-on-knee-dual-energy-computed-tomography-the-multicenter-osteoarthritis-study/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/epidemiology-of-intra-articular-mineralization-on-knee-dual-energy-computed-tomography-the-multicenter-osteoarthritis-study/
