Session Information
Date: Tuesday, November 9, 2021
Title: Systemic Sclerosis & Related Disorders – Clinical Poster III (1836–1861)
Session Type: Poster Session D
Session Time: 8:30AM-10:30AM
Background/Purpose: Systemic sclerosis (SSc) is a rare autoimmune disease categorized on the basis of skin involvement as either limited or diffuse cutaneous SSc, the latter of which manifests in more severe skin and internal organ involvement. SSc disproportionately affects women and, similar to other chronic diseases, health disparities have been noted in SSc with African American (AA) patients experiencing poor outcomes more frequently than patients from other ethnic/racial groups. We utilized a longitudinal cohort of well-characterized SSc patients to compare disease characteristics between AAs and non-AAs and look at gender and social determinants of health.
Methods: Data were collected as part of an ongoing IRB-approved longitudinal registry of SSc patients, including demographics, clinical disease manifestations and medical history. Patients were seen over a 16-year period at a single academic center. Retrospective chart review was performed to confirm age of onset, SSc disease type, and selected criteria for SSc to assess severity of disease. Pearson’s chi-squared and Fisher’s Exact testing for categorical measures, two-sample t-tests for continuous measures, and univariate logistic regression modeling was used.
Results: A total of 372 patients with SSc (79.6% female, 37.9% AA) were identified. AA patients developed SSc at a significantly younger age compared to the non-AA patient subset (41.8±14.3 yrs., 48.9±13.5yrs., respectively, p< 0.0001). Females developed SSc at a younger age than males (45.4±13.9 yrs., 50.2±11.3 yrs, p< 0.01) as shown in Figure 1. Comparing outcomes for diffuse cutaneous SSc, renal crisis, interstitial lung disease and restrictive lung disease were statistically significant in Figure 2A. Comparing AA to non-AA, there was statistically significant risk of all outcomes except renal crisis as shown in Figure 2B. Outcomes in AA versus non-AA and controlling for disease duration, mortality (p< 0.05), diffuse disease (p< 0.0001), pulmonary hypertension (p=0.01), and interstitial lung disease (p=0.01) still remained statistically significant. We looked at two social determinants private insurance and high school graduate with no statistical difference in gender but a statistical significance in race (Table 1). 43.75% of AA had private insurance compared to 66.83% of non-AA (p< 0.0001). 96.39% of non-AA graduated high school compared to 89.72% of AA (p< 0.05). We found males had statistically significant higher percentages of diffuse disease (73.21%), dysphagia (24.59%), and restrictive lung disease (55.81%) compared to females.
Conclusion: We found that AA SSc patients were younger at disease onset and more likely to have diffuse cutaneous disease, compared to non-AA SSc patients. AAs compared to non-AAs with SSc had higher mortality and multiple poor prognostic features, with the exception of renal crisis which was more frequent among non-AAs. Two determinants, private insurance and high school graduate, may be associated with these outcomes. These data support the conclusion that AA have more severe disease with a more unfavorable SSc prognosis. Further investigation into the multifactorial causes for this disparity is needed in order to identify strategies to reduce them.
 Figure 1.jpeg”Figure 1. Age of SSc Disease Onset
Figure 1.jpeg”Figure 1. Age of SSc Disease Onset
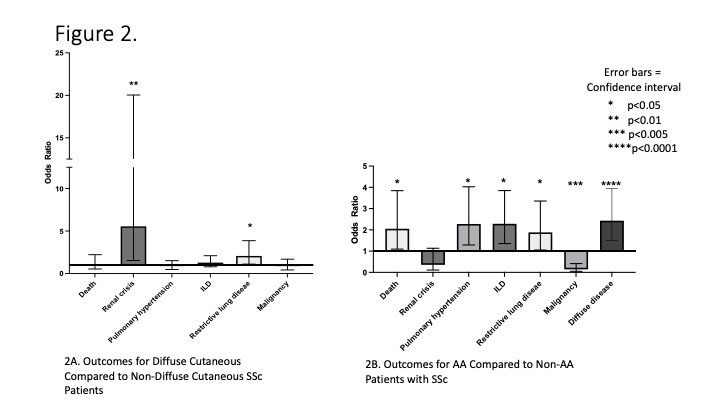 Figure 2.jpeg”Figure 2. Outcomes
Figure 2.jpeg”Figure 2. Outcomes
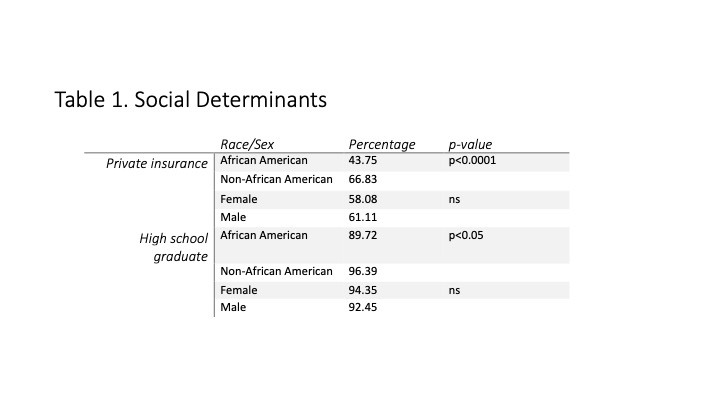 Table 1.jpeg”Table 1. Social Determinants
Table 1.jpeg”Table 1. Social Determinants
To cite this abstract in AMA style:
Compton S, Baker Frost D, Silver R, Kamen D. Disease Characteristics and Social Determinants in African Americans with Systemic Sclerosis: A Single Center Experience [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/disease-characteristics-and-social-determinants-in-african-americans-with-systemic-sclerosis-a-single-center-experience/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/disease-characteristics-and-social-determinants-in-african-americans-with-systemic-sclerosis-a-single-center-experience/
