Session Information
Date: Monday, November 9, 2020
Title: Pediatric Rheumatology – Clinical II: Outcomes & Care Delivery (1983–1987)
Session Type: Abstract Session
Session Time: 10:00AM-10:50AM
Background/Purpose: Patients with pediatric systemic lupus erythematosus (pSLE) receive only a fraction of recommended care. Moreover, variation in care delivery likely contributes to pervasive racial and ethnic disparities in pSLE outcomes. We aimed to begin improving pSLE and mixed connective tissue disease (MCTD) care delivery by defining and assessing variation in performance of a pediatric lupus care index (p-LuCI).
Methods: This was a cross-sectional study of pSLE quality measure performance in the context of an improvement project conducted in the Division of Rheumatology at a large tertiary-care pediatric hospital. Providers included nine attending pediatric rheumatologists and 4 fellow trainees. The project team identified four key drivers of high-quality pSLE care potentially linked to improved outcomes: 1) accurate tracking of pSLE characteristics and treatments, 2) point-of-care outcome assessment, 3) comorbidity assessment and prevention, and 4) timely follow up. To address key drivers, we defined 13 metrics that were bundled into the p-LuCI (Table 1). The p-LuCI was scored from 0-1 based on the number of metrics completed divided by the number of eligible metrics. We combined discrete data from a pSLE visit template along with prescribing and appointment data to capture index components in an automated pSLE report.
We included patients clinically diagnosed with pSLE and MCTD with at least one visit in the Division of Rheumatology within the prior 15 months. After bivariate analyses, independent p-LuCI predictors were identified using multivariable linear regression with clustering by provider. Provider-level variation was defined as +/- 2 SD from the p-LuCI mean.
Results: We included 111 patients (99 SLE, 12 MCTD) with a mean age of 16.9 + 3.0 years. 88 (79%) were female, 39 (35%) were black, and 12 (11%) were Hispanic. 10 (9%) had families who were not English-speaking. Of 33 patients with nephritis, 16 (48%) had prior visits in a multi-disciplinary Rheumatology/Nephrology Clinic.
The mean p-LuCI was 0.56 + 0.25. p-LuCI component performance is shown in Table 1. Patients with higher p-LuCI values were more likely to receive care across nine of 13 metrics. The predictors of p-LuCI performance are shown in Table 2. Independent predictors of higher p-LuCI values were Hispanic ethnicity, chronic steroid exposure, history of nephritis, higher provider pSLE/MCTD volume, and fellow provider assignment. Among providers with > 5 patients under care, p-LuCI values ranged from 0.19 to 0.77. One provider each was significantly above and below the cohort mean (Figure).
Conclusion: We demonstrated that pSLE patients received 56% of p-LuCI measures with significant variation at the provider level. In addition, we identified demographic, disease-specific, and provider characteristics associated with higher performance. Future p-LuCI components should include reproductive counseling, transition preparation, and mental health screening. Multicenter studies are needed to assess the impact of efforts to decrease p-LuCI variation and increase performance on disease activity and damage accrual, disparities in health care utilization, and patient/caregiver satisfaction.
 Table 1. Pediatric systemic lupus erythematosus care index component performance.
Table 1. Pediatric systemic lupus erythematosus care index component performance.
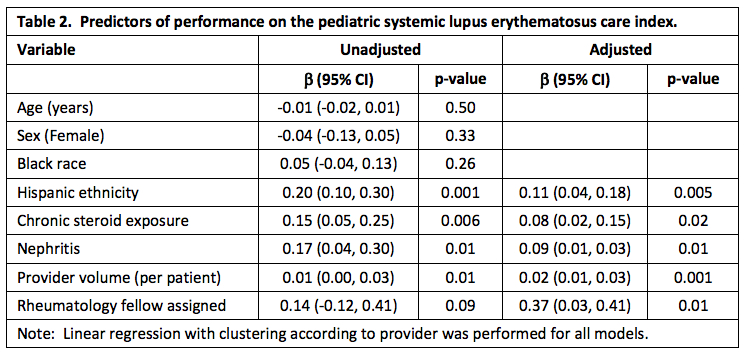 Table 2. Predictors of performance on the pediatric systemic lupus erythematosus care index.
Table 2. Predictors of performance on the pediatric systemic lupus erythematosus care index.
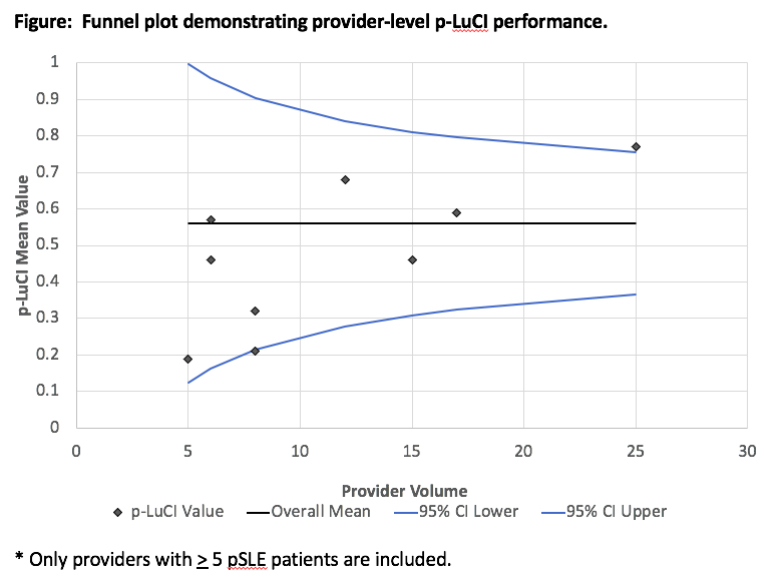 Figure. Funnel plot demonstrating provider-level p-LuCI performance.
Figure. Funnel plot demonstrating provider-level p-LuCI performance.
To cite this abstract in AMA style:
Burnham J, Peterson R, Ukaigwe J, Cecere L, Knight A, Chang J. Determinants of Variation in Pediatric Systemic Lupus Erythematosus Care Delivery [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/determinants-of-variation-in-pediatric-systemic-lupus-erythematosus-care-delivery/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/determinants-of-variation-in-pediatric-systemic-lupus-erythematosus-care-delivery/
