Session Information
Date: Sunday, November 8, 2020
Title: Patient Outcomes, Preferences, & Attitudes Poster II: Miscellaneous Rheumatic Diseases
Session Type: Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: Patients with autoimmune rheumatic diseases may be particularly concerned about COVID-19. We aimed to assess concerns and associated health behaviors of patients with autoimmune rheumatic diseases during the COVID-19 pandemic and evaluate geographic differences within the United States.
Methods: Members of the ArthritisPower research registry and CreakyJoints patient community were invited to complete a baseline survey online with plans for follow-up surveys every 2 weeks for 8 weeks and then at 6 and 12 months. Reponses to the baseline surveys in adults from the United States with self-reported physician diagnoses of rheumatoid arthritis (RA), psoriatic arthritis (PsA), ankylosing spondylitis (AS), and systemic lupus erythematosus (SLE) were analyzed. Differences in patient concerns, avoidance of office visits and testing, use of telehealth, and interruptions in medications were assessed, comparing patients with different autoimmune conditions, immunosuppression use, and residing in different geographies, using zip code-based measures of income, education, rural residence, and COVID-19 activity. Patient concerns (5-point Likert scale) were compared with Kruskal-Wallis tests and other outcomes with univariate logistic regression.
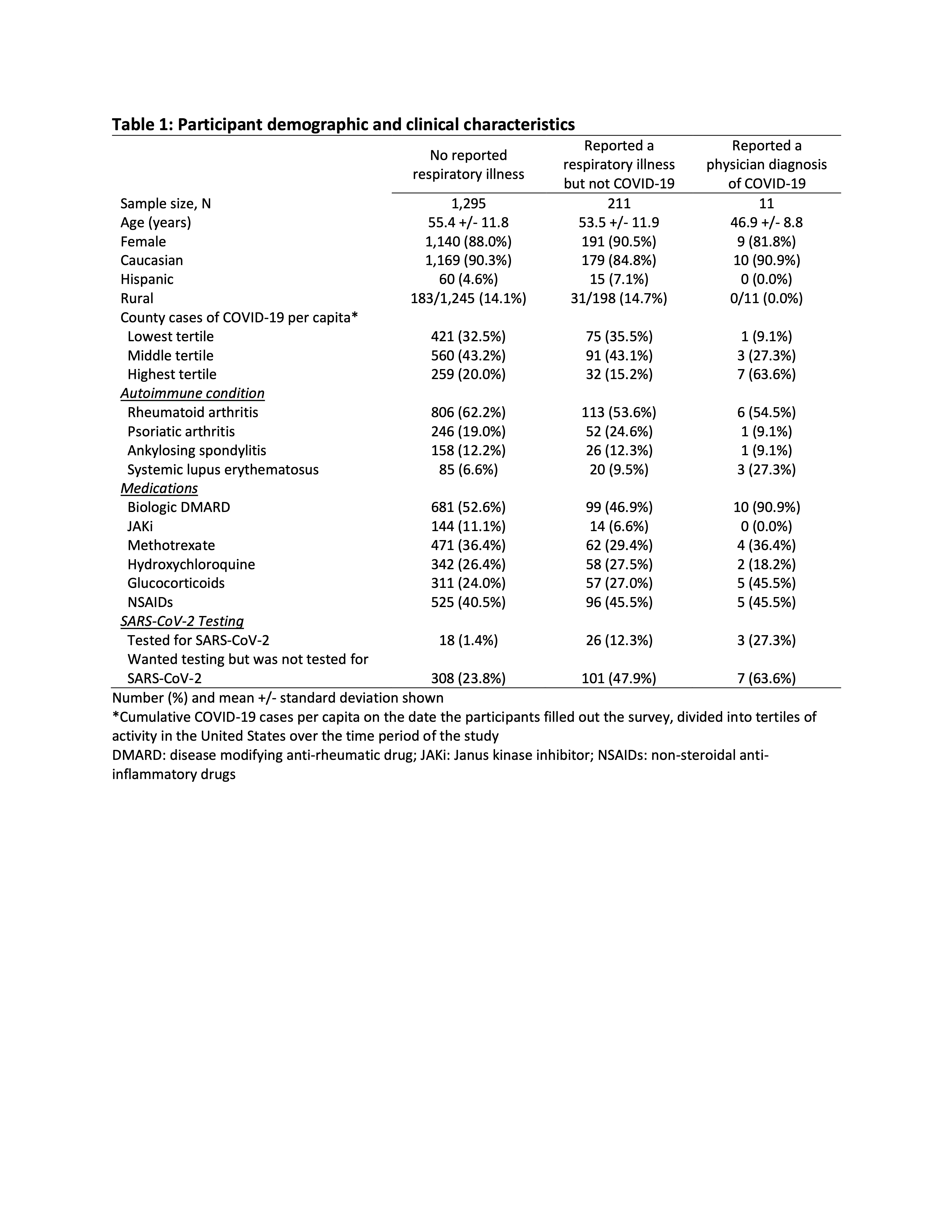
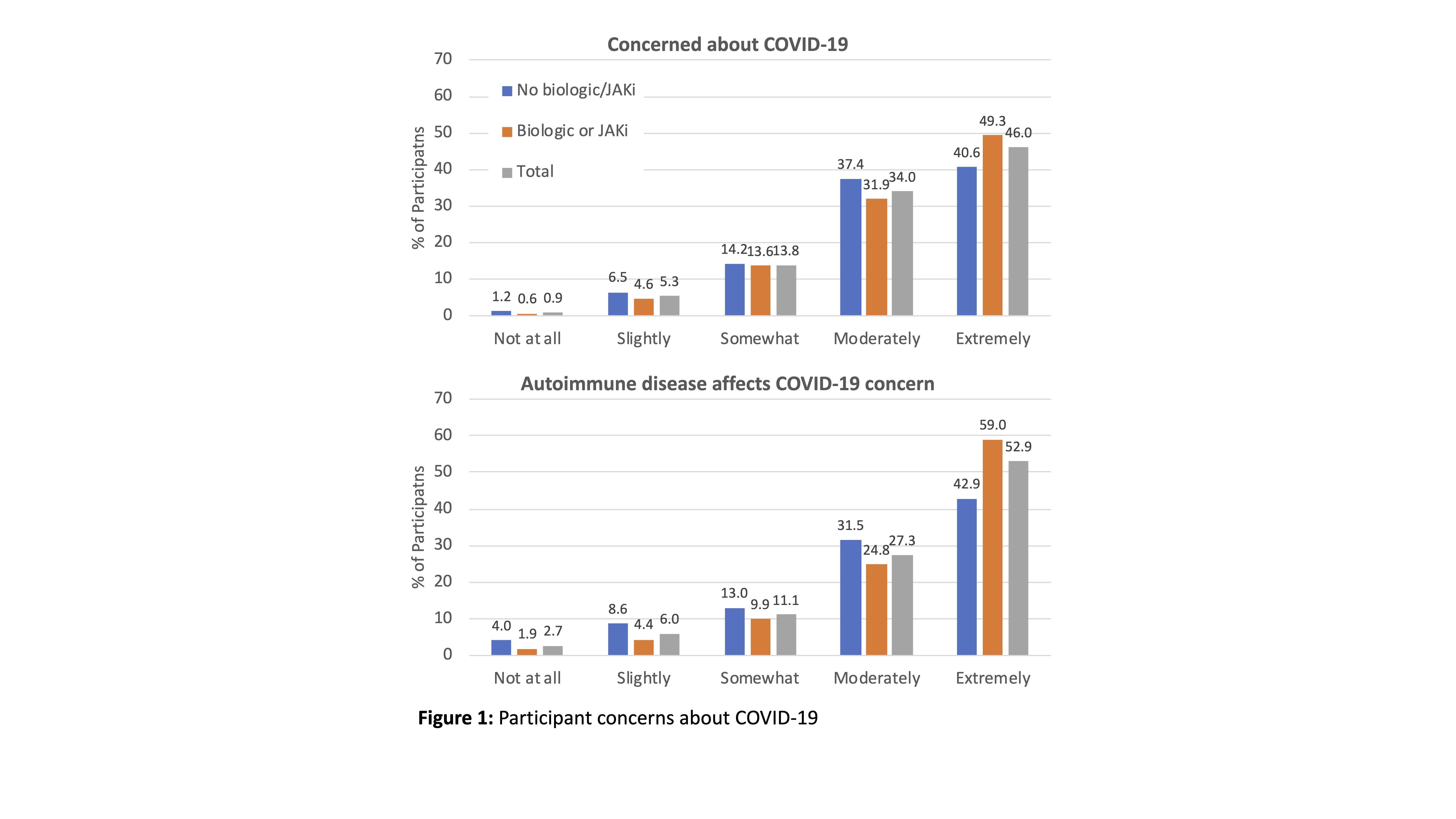
Results: Among 1517 participants (925 RA, 299 PsA, 185 AS, 108 SLE) the mean age was 55.1, 88.3% were female, and 89.5% white (Table 1). 243 participants (13.9%) reported a respiratory illness but were not diagnosed with COVID-19, 47.9% of whom wanted to be tested but were not. 11 patients reported a physician diagnosis of COVID-19. Participants reported substantial concerns about COVID-19 and that their autoimmune disease affected these concerns, with greater concerns among those on biologics/Janus kinase inhibitors (JAKi) (both p < 0.01) (Figure 1). There were no significant differences in concern geographically (census bureau divisions) or in urban versus rural areas. Use of telemedicine (29.5%) and avoidance of doctor’s office visits (56.6%), laboratory testing (42.3%), and other testing (36.0%) were more common in participants from urban areas and counties with more COVID-19 cases per capita (Table 2). Among participants on DMARDs who did not report a respiratory illness or COVID-19 diagnosis, 14.9% stopped one of their medications, more commonly those receiving biologics and with greater COVID-19 concerns (Table 2). Most medication interruptions (78.7%) were not recommended by a physician. Patients who reported that telemedicine was not available were more likely to stop medications (25.4% versus 13.1%, p < 0.01).
Conclusion: In the early months of the COVID-19 pandemic, patients with RA, PsA, AS, and SLE frequently avoided office visits and laboratory testing. Patient behavior was associated more with urban status and geographic variation in COVID-19 activity than with measures of socioeconomic status. Participants often stopped medications without the advice of a physician, and medication interruptions were more common in participants without access to telehealth.
To cite this abstract in AMA style:
George M, Venkatachalam S, Banerjee S, Baker J, Merkel P, Curtis D, Gavigan K, Danila M, Curtis J, Nowell W. Concerns and Behaviors of Patients with Common Autoimmune Rheumatic Diseases in the United States Early in the COVID-19 Pandemic [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/concerns-and-behaviors-of-patients-with-common-autoimmune-rheumatic-diseases-in-the-united-states-early-in-the-covid-19-pandemic/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/concerns-and-behaviors-of-patients-with-common-autoimmune-rheumatic-diseases-in-the-united-states-early-in-the-covid-19-pandemic/