Session Information
Session Type: ACR Abstract Session
Session Time: 11:00AM-12:30PM
Background/Purpose: Nephritis is a severe manifestation of systemic lupus erythematosus (SLE) that develops in 30 to 50 percent of the patients. At the time of diagnosis, it is not possible to predict which patients will develop nephritis.
CL-K1 (collectin kidney-1, collectin-11) is a soluble C-type lectin, with collagenous stalks like C1q, that through recognition of suitably spaced patterns of mannose glycans or negatively charged molecules can activate the complement system. It is found in low concentrations in the circulation in heteromeric complexes with collectin-10 (CL-L1). CL-K1 plays a role in the clearance of apoptotic cells through engagement of DNA displayed on the cell surface. Whereas other complement activating lectins, i.e., MBL, is produced only be hepatocytes, CL-K1 is widely distributed in several tissues in the bodyand it seems to distinguish itself by its capacity for production locally in different tissues.
We hypothesized that complement proteins like CL-K1, could play a role in modifying the local response to deposited DNA containing immunocomplexes, that cause inflammation and tissue damage in SLE, and hence play a protective role in the disease.
Methods: Patients included in the study fulfilled the 1997 ACR revised criteria for the classification of SLE. The cohort was included at two Danish university hospitals and has previously been described (1). A total of 372 SLE patients were included out of which 121 had biopsy verified nephritis. Disease onset was defined as the date of fulfillment of the 1997 ACR revised criteria for the classification of SLE. Lupus nephritis was defined by biopsy verified glomerulonephritis classified after the WHO classification system. Serum concentrations of complement proteins were measured in samples available from all included patients using in-house-developed time resolved immune fluorometric assays (TRIFMA).
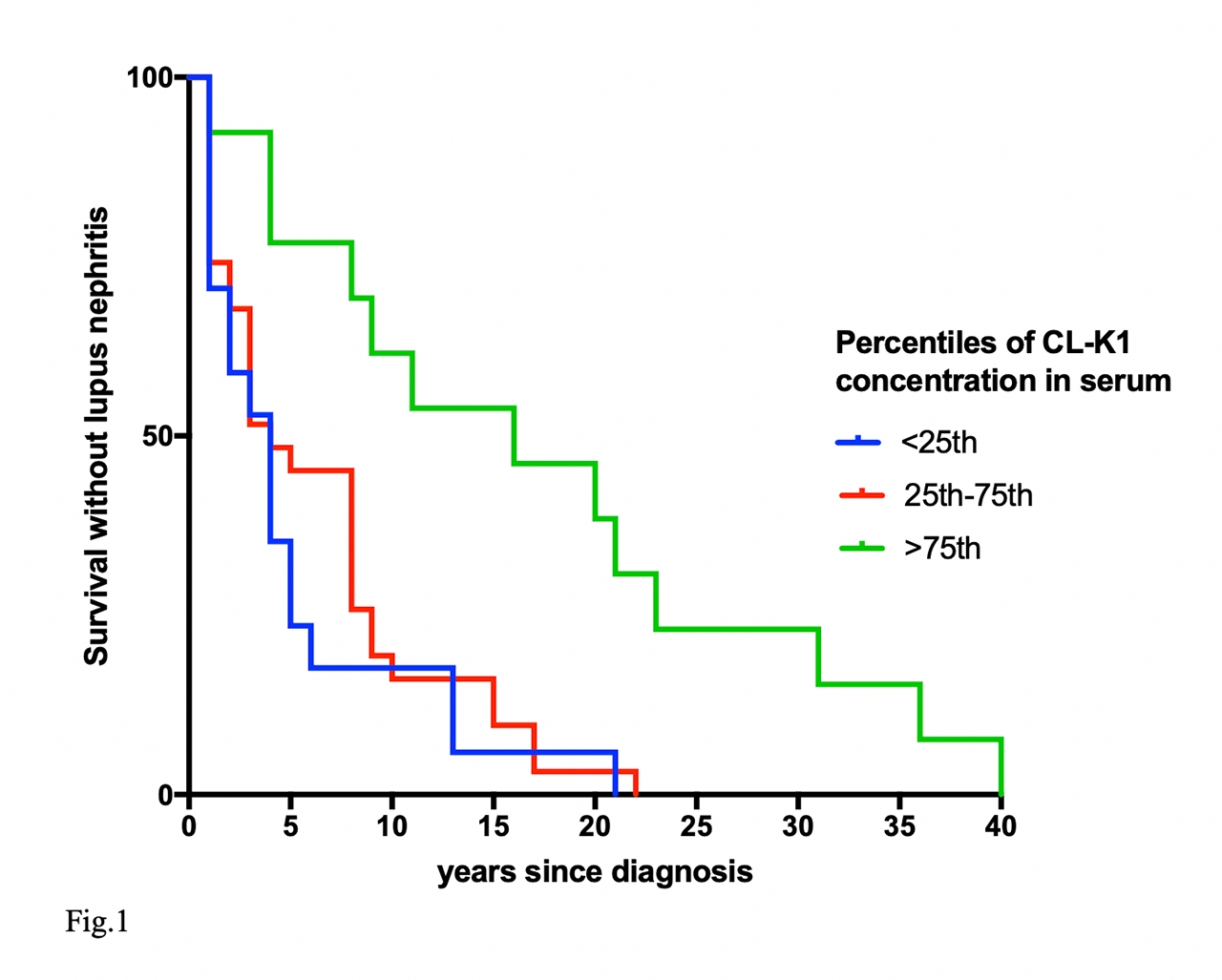
Results: SLE patients with nephritis were clinically different from patients without this manifestation. They were on average younger at diagnosis (median: 27 vs 35, p< 0.05), a larger percentage was positive for anti-double-stranded-DNA (93 vs 85 %, p >0.05), and all patients with nephritis were positive for ANA (anti-nuclear antibody). Patients with nephritis had a lower concentration in serum of CL-K1 compared with patients without nephritis (p< 0.05). No difference was found for CL-L1. Amongst the SLE patients with nephritis, the patients with high concentrations in serum of CL-K1 had a significantly longer time from diagnosis to the onset of lupus nephritis (fig.1).
Conclusion: High serum concentrations of the complement protein CL-K1 were associated with delayed onset of lupus nephritis in a Danish cohort of 372 SLE patients. CL-K1 could play a protective role against the kidney inflammation and damage seen in lupus nephritis.
Ref.1.Troldborg A et al. J Rheumatol. 2018;45(8):1136-1144
To cite this abstract in AMA style:
Troldborg A, Voss A, Hansen S, Jensenius J, Stengaard-Pedersen K, Thiel S. Complement Protein CL-K1 at High Concentrations Protects Against the Development of Lupus Nephritis [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/complement-protein-cl-k1-at-high-concentrations-protects-against-the-development-of-lupus-nephritis/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/complement-protein-cl-k1-at-high-concentrations-protects-against-the-development-of-lupus-nephritis/