Session Information
Date: Tuesday, November 12, 2019
Title: 5T092: RA – Treatments IV: Novel Therapy & Predicting Response (2768–2773)
Session Type: ACR Abstract Session
Session Time: 2:30PM-4:00PM
Background/Purpose: RA patients often inquire about dietary interventions to improve disease control, as they perceive quick changes in pain and/or swelling after consumption of certain foods. Of particular interest is the influence of diet on modifying circulating pro/anti-inflammatory oxylipins and how this relationship affects pain/inflammation. Here, we determine the effect of a 2-week anti-inflammatory diet on clinical and biological outcomes in RA patients.
Methods: Patients with a diagnosis of RA and at least 3 tender and 3 swollen joints in physical exam and no change on medication in previous 2-3 months, who declined escalation therapy, were offered a 2-week anti-inflammatory diet and recruited in our study. This diet comprises of ingredients that increase omega-3/6 ratio, anti-inflammatory species such as turmeric, anti-oxidants, and prebiotics and probiotics. It also eliminates pro-inflammatory ingredients such as lactose, gluten and red meat. In their first visit (day -14), we established their clinical and biological baseline. In their second visit (at day 0) we collected clinical parameters. Patients were given instruction of how to follow the diet and were asked to follow a daily diet log. In their third visit (at day 14), we evaluated study feasibility outcomes, diet adherence and clinical parameters. We also collected blood in all three visits. Trend in clinical changes were examined between day -14 and 0, and between 0 and 14 in a subgroup of these patients (n=10). Serum oxylipins were determined by mass spectrometry before and after diet. Data processing and statistical analysis were performed in SPSS.
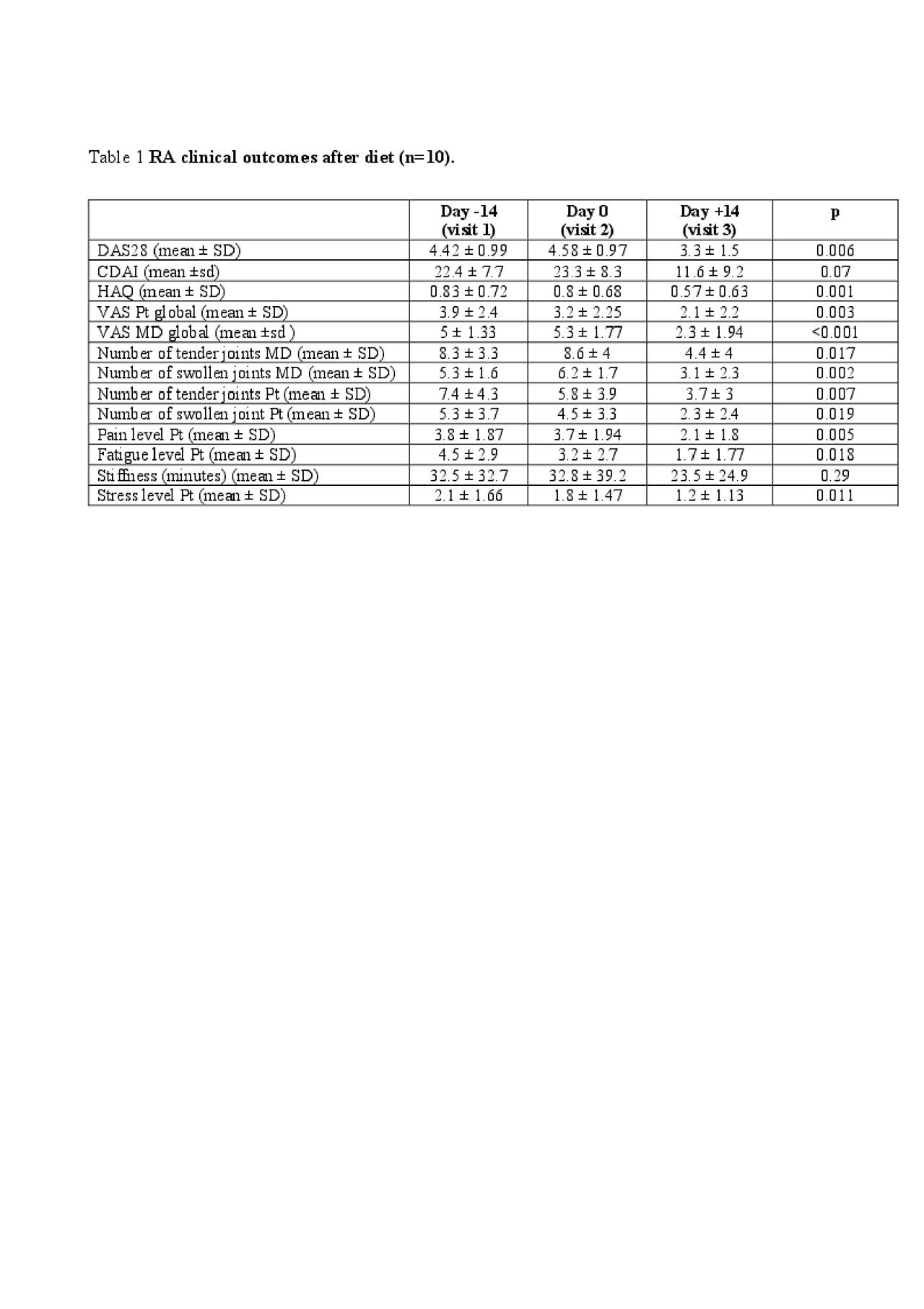
Results: In an ongoing clinical trial, 22 RA patients were recruited from 35 screened patients, and 17 of them (100% seropositive RA women, age average: 55, standard deviation (SD): 5) went through the complete trial. A diet index score (up to 200) showed a good diet adherence (-41.3 (70.9) vs 117.1 (52.1), p< 0.001, for before and after diet trial respectively). As shown in table 1, several clinical outcomes including evaluation of the number of tender (TJC) and swollen joints (SJC), Health Assessment Questionnaire (HAQ), and assessments of pain, fatigue, global disease severity by patients and by physicians, and composite measures of peripheral arthritis such as Disease Assessment Score (DAS)28-CRP and Clinical Disease Activity Index (CDAI) were significantly lower after the 2-week anti-inflammatory diet (table 1). DAS28-CRP after the 2-weeks of anti-inflammatory diet also correlated with the diet index score at visit 3 (p=0.02). Of interest, several pro and anti-inflammatory linoleic acid-derived oxylipins including 13-HODE, 9,10 diHOME and 9,10 EpOME significantly changed after the diet and correlated with index score at visit 3 (p=0.02).
Conclusion: Modulating diet has the possibility to complement medication and improve quality of life for RA patients. Here we showed that RA patients are motivated and followed the diet with good adherence. Diet index scores after the trial correlated with clinical scores and changes in pro- and anti-inflammatory oxylipins suggesting that these mediators could play a role in the clinical effect of this diet in RA patients.
To cite this abstract in AMA style:
cedola f, Coras R, Fernandez-Bustamante M, Agusti-Perez M, Al-Harthi M, Lee S, Singh A, Soo C, Nguyen K, Quehenberger O, Shekhtman T, Golshan S, Guma M. Clinical and Biological Changes in Rheumatoid Arthritis Patients Exposed to an Anti-inflammatory Diet [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/clinical-and-biological-changes-in-rheumatoid-arthritis-patients-exposed-to-an-anti-inflammatory-diet/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/clinical-and-biological-changes-in-rheumatoid-arthritis-patients-exposed-to-an-anti-inflammatory-diet/