Session Information
Date: Sunday, November 8, 2020
Title: Epidemiology & Public Health II: Risk Factors & Outcomes (1467–1471)
Session Type: Abstract Session
Session Time: 4:00PM-4:50PM
Background/Purpose: Patients with rheumatic diseases are at increased risk of infection due to immune dysregulation and the use of immunosuppression. It is unknown whether they are also at increased risk of SARS-CoV-2 infection or of COVID-19-related complications. Using real-world data from the COVID-19 Global Rheumatology Alliance (C19-GRA) Patient Experience Survey, we describe the demographic and clinical characteristics of adult respondents and investigate risk factors related to COVID-19 infection.
Methods: We distributed a patient-reported outcomes survey for adults and parents of children with rheumatic diseases, regardless of COVID-19 status, to all six WHO regions and available in nine languages. The survey was disseminated through patient support organizations and on social media. Patients answered questions regarding their demographics, rheumatic disease diagnosis, medications, as well as COVID-19 diagnosis and its complications. We evaluate the demographics of adults within this study and describe the clinical characteristics of COVID-19 infection from April 3-May 8, 2020.
Results: A total of 9,393 adults completed the survey during the study period (Figure 1). Respondents represented all six WHO regions; most were female (90.0%) with a mean age of 46.1 (SD 12.8) (Table 1). Common diagnoses included rheumatoid arthritis (38.6%), systemic lupus erythematosus (SLE) (30.7%), and Sjogren’s syndrome (13.7%). The majority of patients were taking conventional synthetic DMARDs (70.9%), while 34.7% and 30.8% were on steroids and biologic DMARDs, respectively. Comorbidities included pain syndromes (23.2%), hypertension (22.8%), and pulmonary diseases (21.4%).
Out of the patients surveyed, 519 (5.5%) endorsed having COVID-19 (Table 2). Frequently-reported COVID-19 symptoms included malaise/fatigue (87.1%), cough (78.6%), and headache (78.0%). Only 65 patients (12.5%) required hospitalization. When compared to the population without COVID-19, those with COVID-19 more often had diagnoses of SLE (38.3% vs. 30.2%, p< 0.001) and pulmonary comorbidities (36.0% vs. 20.5%, p< 0.001).
Conclusion: These results demonstrate the feasibility of conducting an international patient-reported outcomes survey to address the impact of the COVID-19 pandemic among patients with rheumatic diseases. Only 5.5% of patients with rheumatic diseases developed COVID-19 and the majority did not require hospitalization, even though most were on immunosuppressive drugs. Patients with SLE and pulmonary comorbidities were overrepresented among those with COVID-19. Future subgroup analyses will explore the relationships between disease states and diagnosis of COVID-19.
Disclaimer: The views expressed here are those of the authors and participating members of the COVID-19 Global Rheumatology Alliance and do not necessarily represent the views of the American College of Rheumatology, the European League Against Rheumatism (EULAR), or any other organization.
 Figure 1. Survey respondents during the study period April 3 – May 8, 2020.
Figure 1. Survey respondents during the study period April 3 – May 8, 2020.
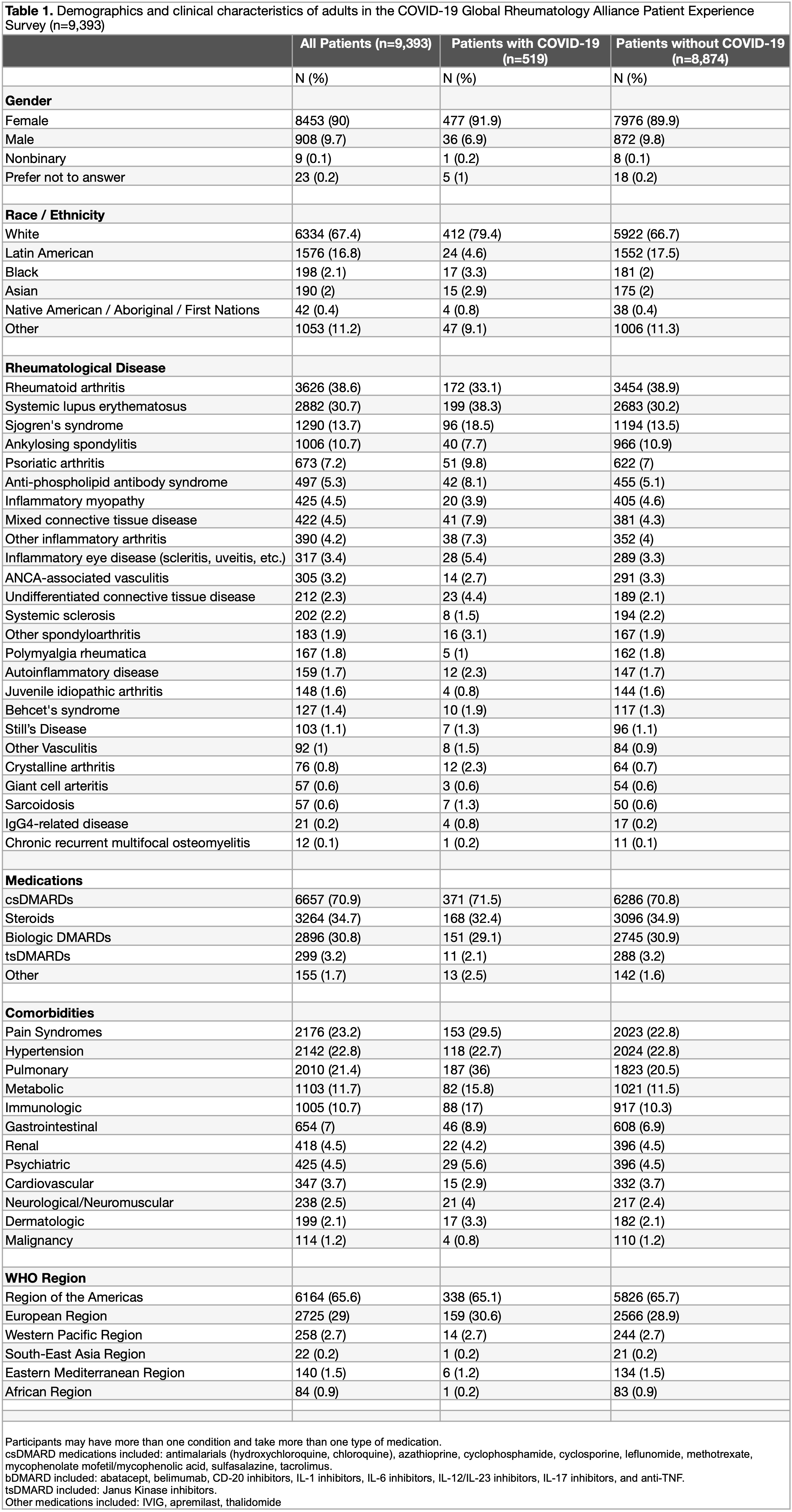 Table 1. Demographics and clinical characteristics of adults in the COVID-19 Global Rheumatology Alliance Patient Experience Survey (n=9,393).
Table 1. Demographics and clinical characteristics of adults in the COVID-19 Global Rheumatology Alliance Patient Experience Survey (n=9,393).
 Table 2. Symptoms and hospitalization status of adults with COVID-19 (n=519).
Table 2. Symptoms and hospitalization status of adults with COVID-19 (n=519).
To cite this abstract in AMA style:
Hausmann J, Kennedy K, Surangiwala S, Larche M, Levine M, Liew J, Wallace Z, Sirotich E. Characteristics of Adult Patients with Rheumatic Diseases During the COVID-19 Pandemic: Data from an International Patient Survey [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/characteristics-of-adult-patients-with-rheumatic-diseases-during-the-covid-19-pandemic-data-from-an-international-patient-survey/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/characteristics-of-adult-patients-with-rheumatic-diseases-during-the-covid-19-pandemic-data-from-an-international-patient-survey/
