Session Information
Date: Tuesday, November 9, 2021
Title: Pediatric Rheumatology – Clinical Poster III: Miscellaneous Rheumatic Disease (1614–1644)
Session Type: Poster Session D
Session Time: 8:30AM-10:30AM
Background/Purpose: Adverse childhood experiences (ACEs) serve as stressors that can have negative, lasting effects on health and wellbeing. While there has been increasing evidence to suggest an etiologic role of ACEs in pediatric chronic pain and rheumatic disease, our understanding of how ACEs may shape a child’s clinical presentation remains limited. We aimed to determine 1) the association between the presence of ACEs and clinical manifestations of pediatric chronic pain and 2) explore the interaction of ACEs and pediatric rheumatic disease among youth with chronic pain on health-related outcomes.
Methods: This was a retrospective cross-sectional cohort study of patients 3-18 years old with chronic pain seen in a pediatric rheumatology pain clinic between August 2018 and July 2020 and previously enrolled in a patient registry. Abstracted clinical data included demographics, past medical, psychological, and social histories, as well as patient reported outcome (PRO) measures including: functional disability inventory (FDI; 0-60), verbal pain report (0-10), symptom severity score (SSS; 0-12) and widespread pain index (WPI; 0-19). We stratified our sample into three groups: no ACEs, one ACE and ≥2 ACEs. We assessed clinical signs and symptoms associated with the presence of ACEs using Chi-square or Wilcoxon-rank tests. The association between ACEs and functional impairment was tested using simple and multivariable linear regression.
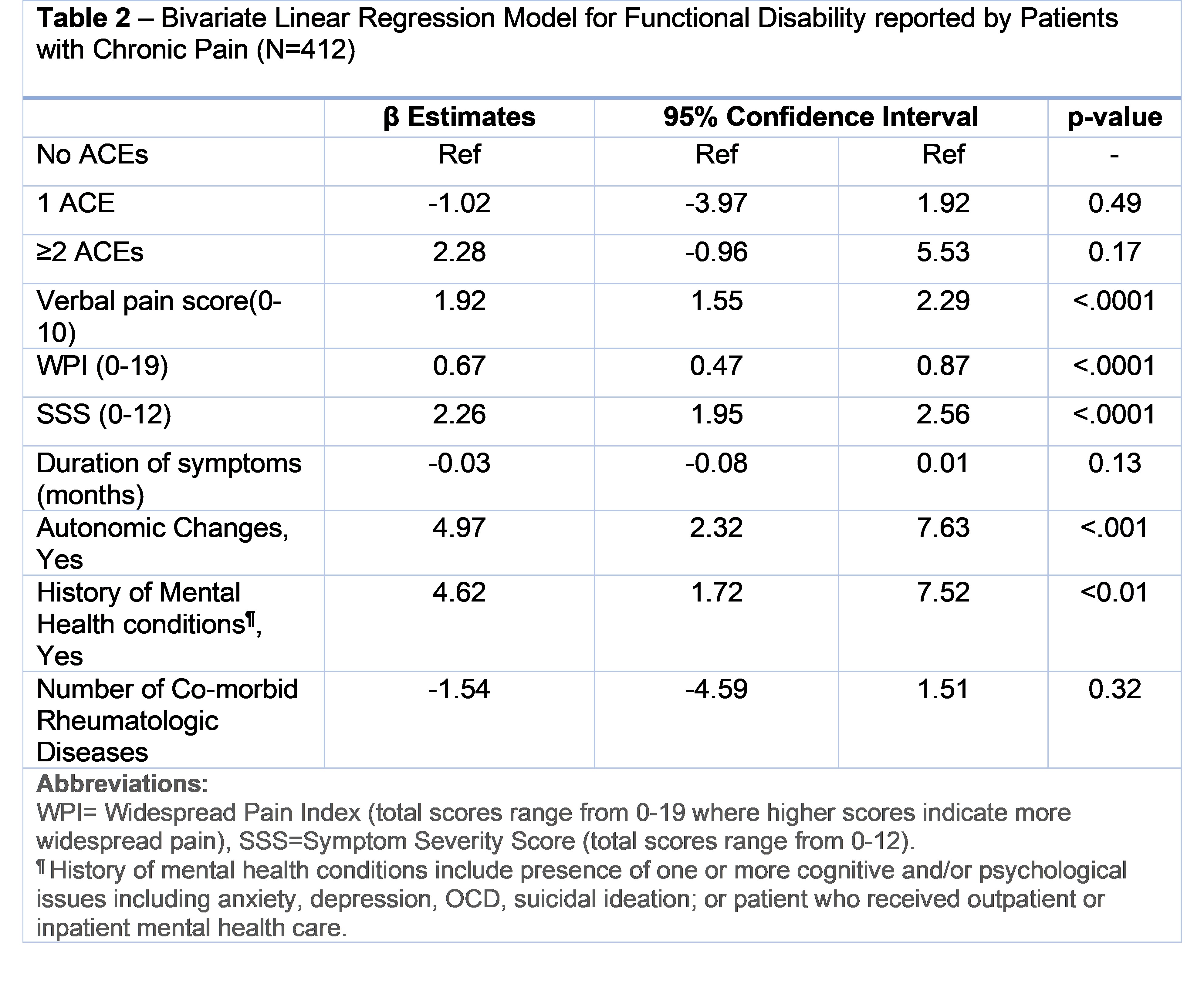
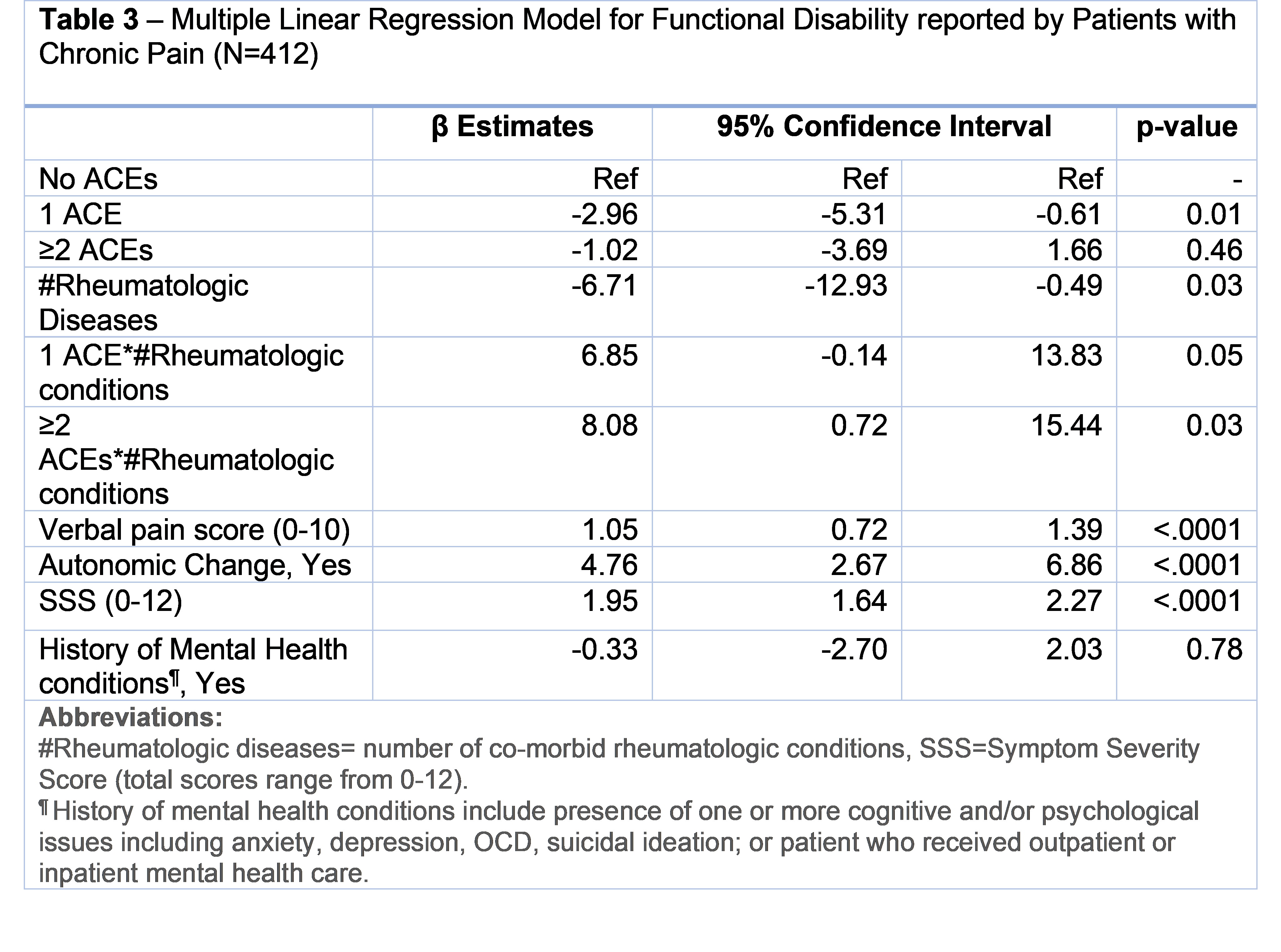
Results: A total of 412 patients were included in the study. More than 75% of patients reported at least one ACE. The most frequently reported ACEs included history of mental illness in a first degree relative (56%) and parental divorce or separation (20%). Those with ≥2 ACEs had more somatic symptoms, worse physical function, and a higher proportion of comorbid mental health conditions than those with no or one ACE (Table 1). Bivariate linear regression indicated positive linear association of patient physical disability (FDI) with WPI, SSS, and verbal pain (all p< 0.05; Table 2). Moreover, presence of mental health conditions and autonomic changes were associated with increased FDI scores in patients. Dose dependent interaction between ACEs and co-morbid rheumatologic conditions was found. As compared to the no ACE group, those with one or more than two ACEs were found to have an additional increase in FDI score by 8.5 and 11 points, respectively, for each additional rheumatologic condition. In multivariable regression (Table 3), higher verbal pain score, symptom severity score and presence of autonomic changes were independently associated with estimated average increase in FDI score by 1.05, 1.95 and 4.76 respectively (all p< 0.01). The interaction demonstrating worsened functional impairment from rheumatologic disease for those with ACEs was again observed.
Conclusion: Children with chronic pain and/or rheumatologic diseases who are exposed to ACEs are at increased risk of worse disability, greater symptom severity, and a higher burden of co-morbid mental health conditions. Our findings indicate an ongoing need for systemic evaluation of ACEs exposure in children with chronic pain and/or rheumatic disease and incorporation of trauma-based care.
To cite this abstract in AMA style:
Sonagra M, Jones J, McGill M, Gmuca S. Burden of Adverse Childhood Experiences in Pediatric Chronic Pain and Rheumatic Disease [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/burden-of-adverse-childhood-experiences-in-pediatric-chronic-pain-and-rheumatic-disease/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/burden-of-adverse-childhood-experiences-in-pediatric-chronic-pain-and-rheumatic-disease/