Session Information
Session Type: Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: In patients with end-stage bilateral knee osteoarthritis, treatment options include either a staged total knee arthroplasty (TKA) procedure, often with a few months in between surgeries, or a simultaneous bilateral TKA (BTKA) procedure during the same anesthetic session. The choice in treatment strategy largely depends on patient and surgeon preferences, and guidelines vary per institution. Our objective was to assess if variations in utilization and in-hospital complications in BTKA are associated with primary insurance.
Methods: Using the National Inpatient Sample (NIS)- Healthcare Cost and Utilization Project (HCUP) database (2007-2016) we sought to examine BTKA utilization and in-hospital complications comparing those with Medicare/Medicaid (CMS) vs those with private insurance (Pvt) in a retrospective analysis. All patients ≥ 50 years who underwent elective primary TKA were included. We computed differences in temporal trends in proportional utilization and in-hospital complications after BTKA comparing those with CMS vs Pvt insurance. Next, we performed multivariable logistic regression models to assess insurance differences in temporal trends adjusting for individual (age, sex, Elixhauser comorbidity index, and morbid obesity), hospital level (hospital volume, bed size, region and teaching status) and community level (median household income) variables. Discharge weights were used for nationwide estimates.
Results: An estimated 132,400 (49.5%) CMS patients and 135,046 (50.5%) privately insured patients underwent BTKA from 2007-2016. (Table 1) Amongst UTKA patients, 62.7% had CMS insurance and 37.3% had Pvt. While in both UTKA and BTKA, patients with private insurance were more likely to be younger and had a higher proportion of females. In univariate analysis, hospital mortality, length of stay and complications were significantly higher in those with CMS compared to private insurance (p < 0.001). After adjusting for covariates, CMS was associated with higher odds of in-hospital BTKA and UTKA complications compared to Pvt (Bilateral aOR: 1.10, 95% CI: 1.05–1.15, P = < 0.0001; Unilateral aOR: 1.32, 95% CI: 1.10–1.59, P = 0.003). BTKA in-hospital complications remained higher in CMS group throughout the study period (1.23% in Pvt vs 1.36% in CMS in 2007-08, whereas 0.54% in Pvt vs 1.14% in CMS in 2015-16), though the trend difference was not statistically significant (Figure 1). Proportional utilization of BTKA amongst private insurance was higher than CMS throughout the study period even after adjusting for covariates (7.18% in Pvt vs 4.59% in CMS in 2007-08, whereas 5.63% in Pvt vs 3.13% in CMS in 2015-16, P < .0001) (Figure 2).
Conclusion: In this nationwide study of BTKA patients from 2007 to 2016, we found that the utilization of BTKA is higher in those who are privately insured compared to those who have Medicare/Medicare insurance. Further privately insured patients have lower in-hospital complication rates compared to those with government insurance. There can be many factors explaining these findings such as working status and patient preference which may play a role in BTKA decisions and thus further research in this area need to be done to understand these differences.
 Table1: Baseline characteristics and outcomes by TKA type and Insurance
Table1: Baseline characteristics and outcomes by TKA type and Insurance
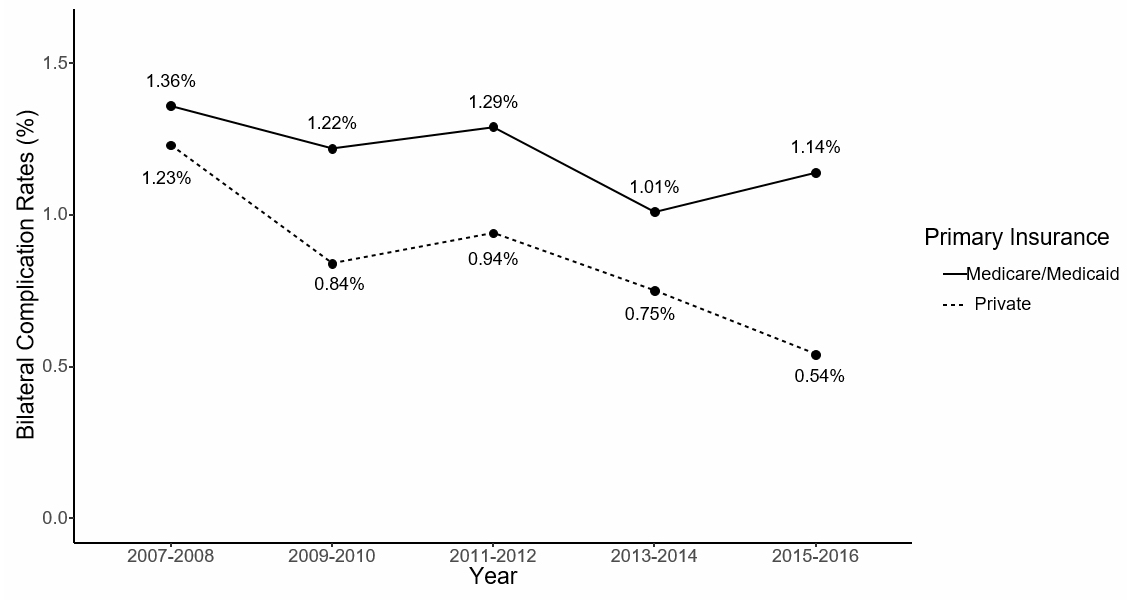 Figure 1: Bilateral Complications by Primary Insurance
Figure 1: Bilateral Complications by Primary Insurance
 Figure 2: Percentage of Bilateral TKAs by Primary Insurance
Figure 2: Percentage of Bilateral TKAs by Primary Insurance
To cite this abstract in AMA style:
Mehta B, Ho K, Bido J, Memtsoudis S, Parks M, Russell L, Goodman S, Ibrahim S. Association of Primary Insurance Status on Bilateral Knee Arthroplasty Utilization and Complications: A United States Nationwide Analysis [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/association-of-primary-insurance-status-on-bilateral-knee-arthroplasty-utilization-and-complications-a-united-states-nationwide-analysis/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/association-of-primary-insurance-status-on-bilateral-knee-arthroplasty-utilization-and-complications-a-united-states-nationwide-analysis/
