Session Information
Session Type: Abstract Submissions (ACR)
Background/Purpose: Interstitial lung disease (ILD) is an outcome with high morbidity and mortality in rheumatoid arthritis (RA). Citrullinated proteins are observed in these lung tissues; however, the association of specific anti-citrullinated peptide antibodies (ACPA) with ILD in RA is unknown.
Methods: RA patients underwent multi-detector computed tomography (MDCT) of the chest with interpretation by a pulmonary radiologist for ILD features [ground glass opacification (GGO), reticulation (R), honeycombing (HC), and traction bronchiectasis (TB)]. A semi-quantitative ILD Score (ILDS; range 0-32) for ILD features was calculated. Concurrent serum samples were assessed for anti-CCP (CCP2) and levels of a panel of antibodies against 4 non-citrullinated proteins [fibrinogen A, HSP60, apolipoprotein (Apo) A1, and Apo E] and 17 citrullinated full-length proteins or peptides within these proteins (see table for list) using a custom Bio-Plex bead array. Individual candidate citrullinated antigens were conjugated to spectrally-distinct fluorescently dyed beads. Peptide-conjugated beads were incubated with diluted patient sera, autoantibody binding detected with a phycoerythrin-conjugated secondary antibody, and levels of autoantibody binding quantitated on a Luminex 200 System. High level ACPA was defined at ≥ the group 75th percentile. Pulmonary function testing (PFT) was performed in 156 patients a mean of 21±3 months later.
Results: Among 177 RA patients [60% female, 86% Caucasian, mean age 59±9 years, 11% current smokers], any ILD features (i.e. ILDS>0) was observed in 57 (32%). Among those with any ILD, the median ILDS was 3 (range 1-10). A predominant pattern of GGO was observed in 22 (39%) and R/HC/TB in 35 (61%). PFT restriction or impaired diffusion was observed in 36 (23%).
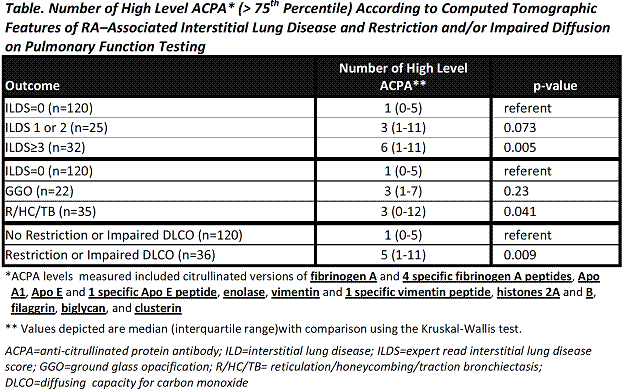
Levels of CCP2 and all specific ACPAs were 46-273% higher among RA patients with vs. those without ILD (all p-values<0.05), and higher levels correlated with higher ILDS. In contrast, levels of non-citrullinated protein antibodies were not higher in those with ILD. The median number of high level ACPA was significantly greater for those with an ILDS≥3 vs. those with an ILDS=0 (6 vs. 1; p=0.005, see Table). Each ACPA was associated, on average, with a 0.10 unit increase in ILDS (p=0.001), an association that remained significant after adjusting for features associated with ILD [age, gender, current and former smoking, DAS28, current prednisone and leflunomide use]. More high level ACPA were observed in R/HC/TB compared to ILDS=0, but the difference was less robust for GGO vs. ILDS=0 (Table). More high level ACPA were observed in those with PFT restriction or impaired diffusion compared to those without these PFT findings (Table).
Conclusion: Our findings of a broader ACPA repertoire in RA ILD suggest a role for ACPA in the pathogenesis of ILD and/or implicate inflamed lung parenchyma as a source of ACPA generation.
Disclosure:
J. T. Giles,
None;
S. Danoff,
None;
J. Sokolove,
None;
R. Winchester,
None;
D. A. Pappas,
None;
C. Cramb,
None;
G. Connors,
None;
S. S. Siegelman,
None;
W. H. Robinson,
None;
J. M. Bathon,
None.
« Back to 2012 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/an-expanded-repertoire-of-anti-citrullinated-peptide-antibodies-is-associated-with-interstitial-lung-disease-in-rheumatoid-arthritis/