Session Information
Session Type: ACR Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: Patients with rheumatoid arthritis frequently refuse to escalate care because they overweight the probability of adverse events. Effectively communicating risk information to patients is difficult. Several approaches have been developed to facilitate comparative risks; however, recent data suggest that current approaches have a limited impact on risk perceptions and willingness to take medication. The objective of this study was to examine whether an icon array (IA), an illustration of the gist of how medications regulate the immune system (a series of balance beams), or both influence willingness to start a medication.
Methods: Patients with a rheumatic disease were mailed a survey in which they were asked to imagine that their symptoms had worsened and that their physician was recommending a new medication. We varied the probability of an adverse event (pneumonia requiring hospitalization): 2% or 0.2%, and the risk presentation format: numbers, numbers + IA, numbers + balance beams (BB), or numbers + both. Route of administration, benefit, and cost were held constant. Each subject responded to a single, randomly-assigned scenario. We controlled for socioeconomic status (SES), using a variable including both difficulty paying for medications as well as education, in a full-factorial model testing willingness to take the medication (measured on a 5-point scale).
Results: Of 1453 surveys, 465 patients completed the survey. Overall, the mean (SD) age was 59.0 (14.8); 79.7% were female; 83.2% White and 39.1% were classified as having low SES. There were no statistical differences in patient characteristics across the risk presentation formats. Willingness to start the medication was predicted by the interaction between the risk presentation format and SES (F = 2.9, p = 0.03). Willingness by SES status is described in the Figure 1. Among low SES subjects, addition of an IA did not affect willingness compared to the numbers-only format. In contrast, addition of BB (mean difference = 0.47, p = 0.07), or both IA and BB increased willingness (mean difference = 0.48, p = 0.04). Among high SES subjects, addition of an IA or BB or both did not influence willingness compared to the numbers only format. However, both formats including an IA increased willingness compared to the BB format among high SES subjects (mean difference IA vs BB= 0.53, p =0.01; mean difference IA vs IA + BB = 0.48, p = 0.02).
Conclusion: SES affects how subjects respond to risk presentation formats. IA marginally increases willingness in high SES subjects, while BB increases willingness in low SES subjects; when both IA and BB are present, SES differences disappear. BB, when not accompanied by an IA, may decrease willingness in high SES subjects. These results demonstrate the differential effects of risk presentation formats, and highlight the need to identify mechanisms underlying their effects when implementing decision-support tools. 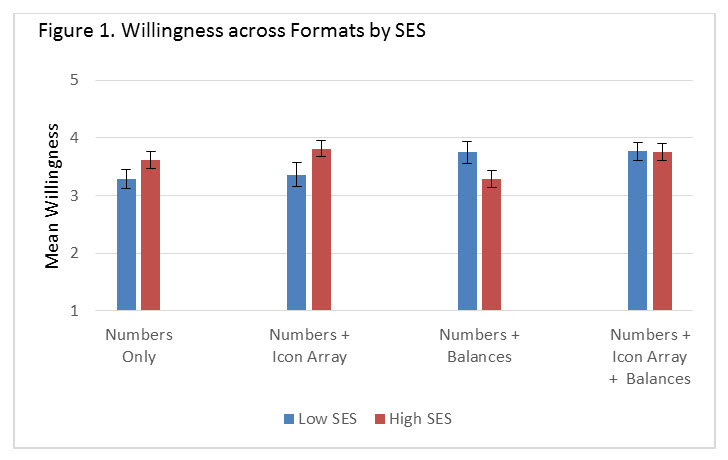
To cite this abstract in AMA style:
Cozmuta R, Wilhelms E, Reyna V, Nolte J, Fraenkel L. The Influence of Risk Presentation Format on Willingness to Start a Medication [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/the-influence-of-risk-presentation-format-on-willingness-to-start-a-medication/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/the-influence-of-risk-presentation-format-on-willingness-to-start-a-medication/
