Session Information
Session Type: ACR Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose: Identifying individuals as early as possible in the development of an autoimmune disease may lead to important opportunities. This study utilizes an established population-based registry to evaluate the burden of individuals who do not meet criteria for SLE but may be at higher risk of being diagnosed later.
Methods: The Georgia Lupus Registry (GLR) is designed to more accurately estimate the incidence and prevalence of SLE in Atlanta, Georgia. The state allowed investigators and trained abstractors to access protected health information without patient consent. Sources of potential cases included hospitals (20), rheumatologists (35), nephrology groups (10), dermatology groups (20), commercial labs, and population databases. Databases were queried for the International Classification of Diseases, Ninth Revision, (ICD-9) code 710.0 (SLE), as well as 695.4 (discoid lupus), 710.8 (other specified connective tissue disease), and 710.9 (unspecified connective tissue disease), as well as serologies and pathology results suggestive of SLE. Antiphospholipid antibody syndrome was searched for if a consistent code was used at a particular facility. Those with less than 4 American College of Rheumatology (ACR) criteria for SLE and without a final physician diagnosis of a specific connective tissue disease were analyzed. Rates were determined for incidence (2002-2004) and prevalence (2002) and age adjusted using the 2000 US population. Age adjusted estimates and 95% confidence intervals were calculated by the direct method using R (routine ageadjust.direct).
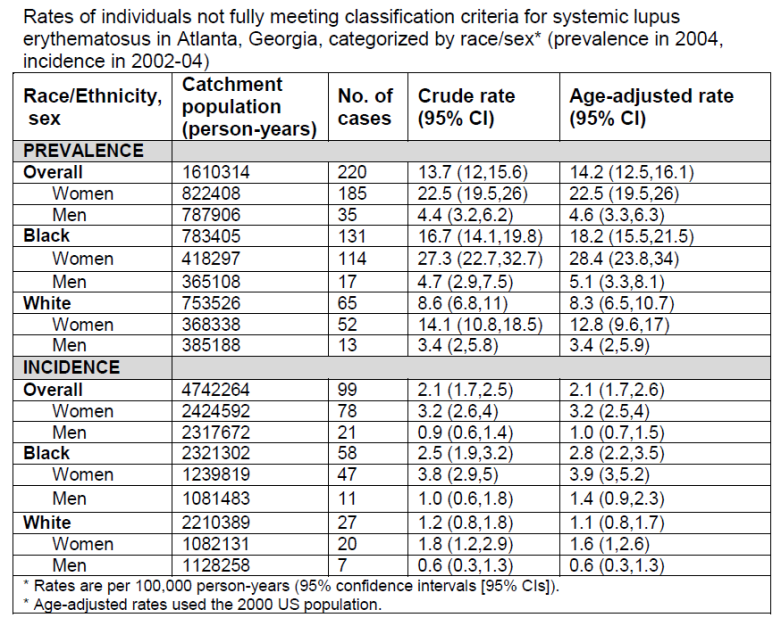
Results: 220 individuals were prevalent in 2004 with an overall age-adjusted rate of 14.2 per 100,000 person-years. 99 individuals were incident in 2002-04 with a rate of 2.1. Similar to SLE, the highest rates were in women and blacks. The rate ratio of prevalent women to men was 4.9 and was 2.2 in blacks to whites, lower than seen in SLE. (Table 1) The most frequent ACR criteria manifestations were ANA (56.4% and 57.6% in prevalent and incident individuals, respectively), hematologic disorder (39.1%, 35.4%), and arthritis (30%, 32.3%). There were no statistically significant differences between blacks and whites.
Conclusion: This is the first population-based evaluation of those not fully meeting ACR criteria for SLE in the US. The prevalence and incidence rates were 15% and 30%, respectively, of that which were seen in those validated as having SLE from the same general population. This suggests a significant population at higher risk of being diagnosed with SLE in the future can be identified. Studies are ongoing to determine the outcomes of these patients.
To cite this abstract in AMA style:
Saxena P, Bao G, Drenkard C, Lim SS. The Epidemiology of Individuals Not Fully Meeting Classification Criteria for Systemic Lupus Erythematosus (SLE): The Georgia Lupus Registry [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/the-epidemiology-of-individuals-not-fully-meeting-classification-criteria-for-systemic-lupus-erythematosus-sle-the-georgia-lupus-registry/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/the-epidemiology-of-individuals-not-fully-meeting-classification-criteria-for-systemic-lupus-erythematosus-sle-the-georgia-lupus-registry/