Session Information
Date: Sunday, November 8, 2020
Title: Patient Outcomes, Preferences, & Attitudes Poster II: Miscellaneous Rheumatic Diseases
Session Type: Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: Both the process of being diagnosed with a chronic illness and the illness itself can be a traumatizing experience (1). The current study examined the diagnosis of a chronic illness, systemic sclerosis (SSc), as a potentially traumatic experience. We examined SSc patients’ perceptions of the process of getting diagnosed and their reactions to this diagnosis. Our research question was, “What do patients report experiencing regarding the process of being diagnosed with SSc?”
Methods: Patients with SSc were approached to participate by their rheumatologist (specializing in SSc) during an office visit. Sixty-four patients completed the study (42% diffuse, 45% limited, 13% unknown type of SSc). All patients included met ACR-Eular criteria for diagnosis of SSc. Most respondents were female (85%), white (95%), and had an average age of 61 years.
Patients completed open-ended questions (e.g., what prompted you to first go to the doctor, what occurred through the time you were diagnosed with SSc, how did you react to the diagnosis). Two researchers independently categorized responses. Discrepancies were resolved by discussion. Additionally, one researcher retrieved demographic and disease information from patients’ records.
Results: Seventeen percent of the sample received a potentially traumatic message from a health professional during the diagnostic process. For example, one patient reported learning there was no treatment for SSc and it would continue to get worse, one reported being told she was dying (before SSc was diagnosed), and another reported physicians involved in the diagnostic process were dismissive of independent and seemingly unrelated symptoms.
As can be seen in Table 1, fear was the most common patient reaction, especially fear of the future and fear of dying. Other reactions were feeling upset about not having a diagnosis (before SSc was diagnosed), feeling concern because of the disease progression they witnessed in others, feeling anticipatory grief, feeling sad or shock, and questioning their ability to cope.
Conclusion: Diagnosing and treating chronic illness can be a difficult process for both patients and practitioners (1). Consistent with past research, reactions to the diagnostic process showed patients did not self-label their reactions as depression (2). In the current study, few patients even reported sadness; fear was the overwhelmingly common reaction.
The current data emphasize the importance of physicians attending to the way information regarding SSc is conveyed to patients. Although a majority did not report receiving traumatic messages from a health care professional during the diagnostic process, over 1 in 6 patients did. Given the diagnostic process for SSc can be lengthy, patients may be feeling distressed for years. Health providers working with SSc patients should address patients’ emotions and the causes of them (e.g., internet, statement by health provider) and know that their conversations with patients can make a difference.
References:
- Fennell PA Managing chronic illness using the Four-Phase Treatment Approach. Wiley; 2003
- Newton EG, Thombs BD, Groleau D. The experience of emotional distress among women living with scleroderma. Qual Health Res 2012; 22: 1195-1206.
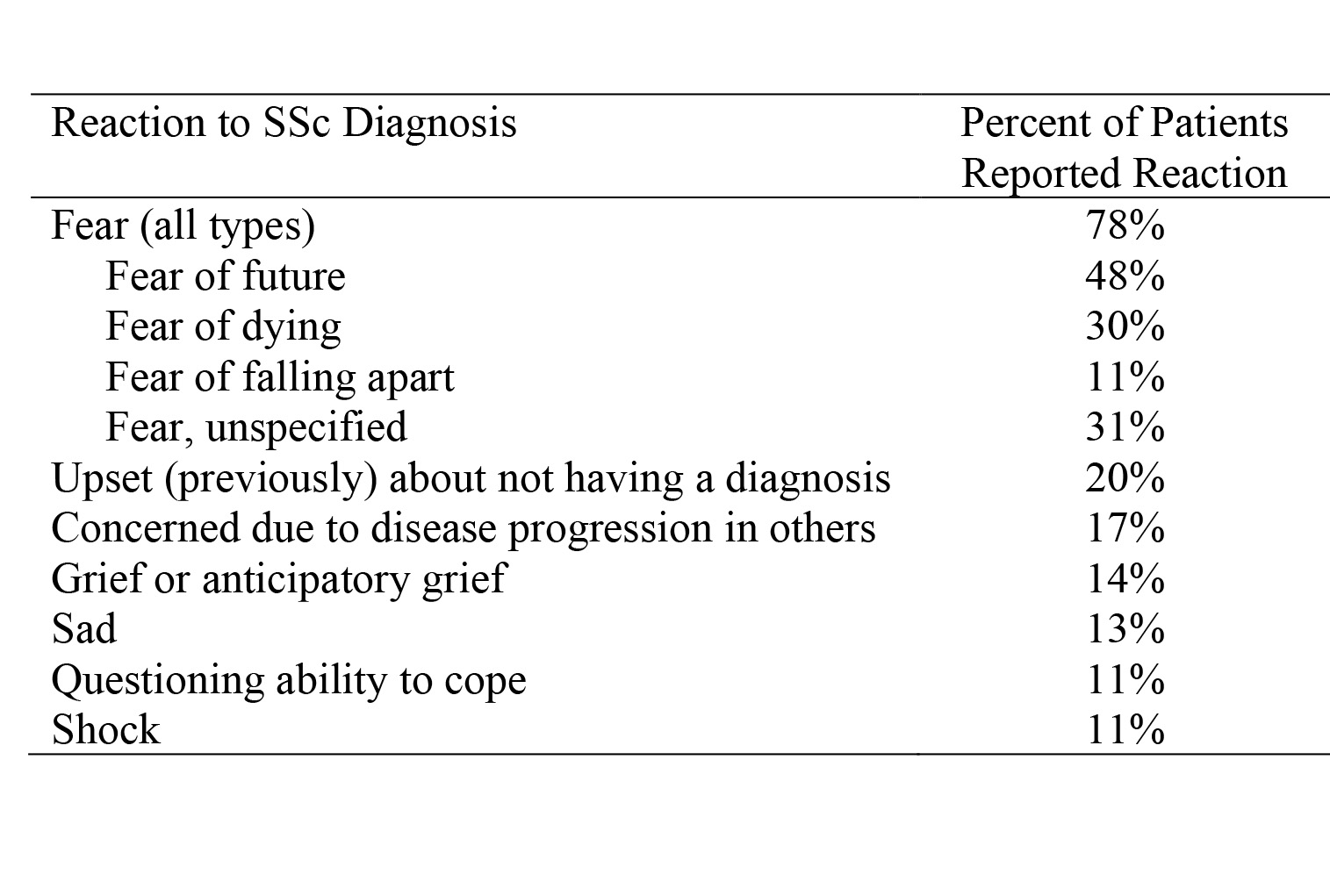 Table 1. Reactions to Being Diagnosed With SSc and Percent of Patients Who Reported Each Reaction
Table 1. Reactions to Being Diagnosed With SSc and Percent of Patients Who Reported Each Reaction
To cite this abstract in AMA style:
Patricia F, Shapiro L, Dorr N, Lukasiewicz R, Houser F, Taylor M. The Diagnosis of Systemic Sclerosis as a Traumatic Experience: Patients’ Reactions to the Diagnostic Process [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/the-diagnosis-of-systemic-sclerosis-as-a-traumatic-experience-patients-reactions-to-the-diagnostic-process/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/the-diagnosis-of-systemic-sclerosis-as-a-traumatic-experience-patients-reactions-to-the-diagnostic-process/
