Session Information
Date: Tuesday, November 14, 2023
Title: (2387–2424) Vasculitis – Non-ANCA-Associated & Related Disorders Poster III
Session Type: Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: In the last few years, several cut-off points for the intima-media thickness (IMT) of temporal arteries (TA) and large vessels (LV) have been proposed for the ultrasound (US) diagnosis of giant cell arteritis (GCA). It has usually been recommended to use the average measure of the higher IMT, but there is currently a lack of consensus on this. We have observed some changes in the IMT measurements depending of if they are performed in systole or diastole. To confirm if there are differences in the IMT measurement taken in systole or diastole and if they are clinically relevant.
Methods: Observational study that included recorded videos of the US examination performed in consecutive patients referred to our GCA fast track clinic with suspicion of GCA. The gold standard diagnosis was the clinical diagnosis of the doctor after at least 6 months of follow-up. All the videos of every explored vessel (TA with their common trunk -CT- and their frontal -FR- and parietal -PAR-branches, subclavian -SC- and axillary -AA- arteries) were reviewed and the IMT of each of them was measured in systole and diastole peaks. We define an US result as positive with cut-off values of IMT ≥ 0.34 mm for FR and PAR, ≥ 0.42 mm for CT, and ≥ 1 mm for AA and SC. Demographic data were also collected. Reliability was tested by two independent readers in 40 patients using the of intraclass correlation coefficient mixed model absolute agreement (ICC).
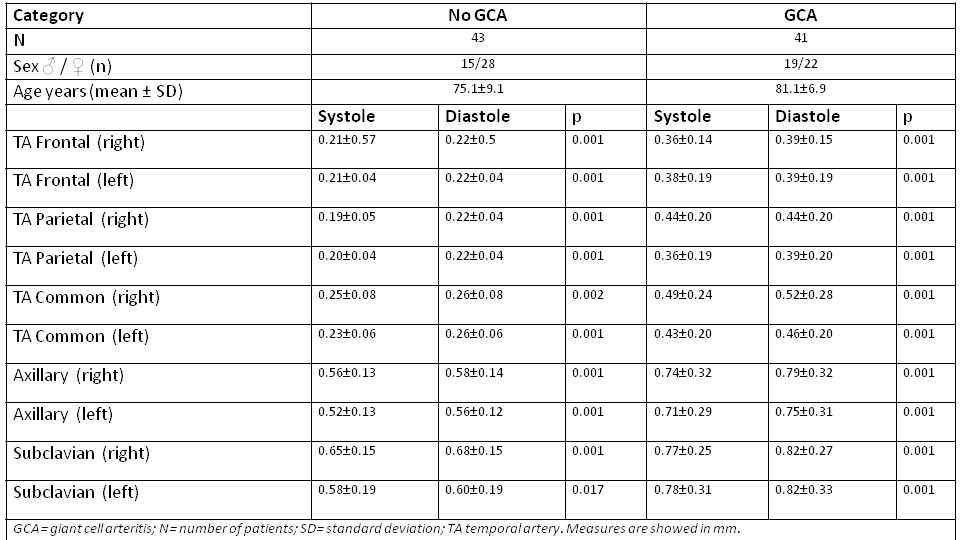
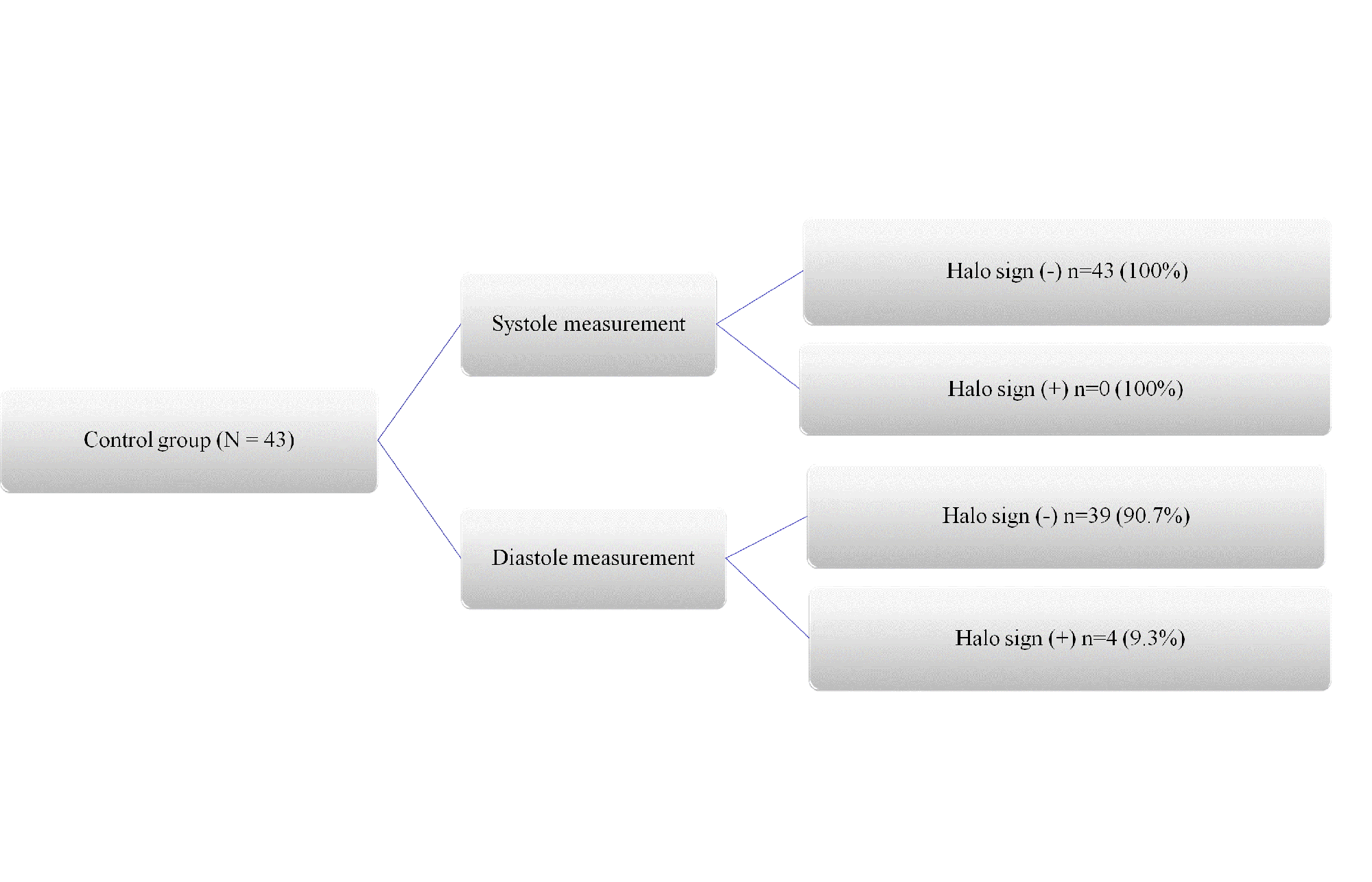
Results: We have included 84 cases, 41 with GCA and 43 without GCA (controls). The mean values of age and sex, as well as the IMT in systole and diastole of each vessel are shown in Table 1. There were not significant differences in sex but patients without GCA were younger (p< 0.01). US IMT measurements in systolic and diastolic times showed statistically significant differences in all the explored vessels, both in patients with GCA and in the control non GCA group (Table 1). All the IMT measured in diastole showed higher and statistically significant values than those measured in systole, with a mean increment of measurement of 5.7% and 6.83 % in TA and 5.02% and 4.95% in LV, respectively in the GCA and control group. These results can have clinical relevance since if we used diastolic measurements, instead of systolic measurements, 4/43 (9.3%) cases in controls had halo sign in one isolated vessel (1 case in right FR, 1 in right CT, 1 in right SC, 1 in left SC) (Figure 1). However, in GCA patients, the number of patients with halo sign did not change, but the number of pathological vessels increased in 15 branches when the measurement was performed in diastole (2 in right FR, 3 in right PAR, 1 in right CT, 3 in left FR, 4 in left CT and 2 in right AA)(Fig 1), so it could influence the assessment of the disease with OGUS or other scores. The result of the interrater analysis, between two readers, revealed an ICC between 0.845 and 0.992 for the different arteries.
Conclusion: There are significant differences between the IMT measured in systolic and diastolic peaks, as in GCA as in normal controls, with higher values in diastole. The differences are relatively small but may increase the number of false positives in 9.3% cases in controls, and the number of affected vessels in the GCA group. This should be considered in the diagnosis and assessment of GCA.
To cite this abstract in AMA style:
Brugarolas E, Fernandez-Fernandez E, Monjo I, De Miguel E. Systole and Diastole Ultrasound Wall Thickness Shows Significant Differences That Affect the Diagnosis and Assessment of Giant Cell Arteritis [abstract]. Arthritis Rheumatol. 2023; 75 (suppl 9). https://acrabstracts.org/abstract/systole-and-diastole-ultrasound-wall-thickness-shows-significant-differences-that-affect-the-diagnosis-and-assessment-of-giant-cell-arteritis/. Accessed .« Back to ACR Convergence 2023
ACR Meeting Abstracts - https://acrabstracts.org/abstract/systole-and-diastole-ultrasound-wall-thickness-shows-significant-differences-that-affect-the-diagnosis-and-assessment-of-giant-cell-arteritis/