Session Information
Date: Monday, November 9, 2020
Title: Pediatric Rheumatology – Clinical Poster III: SLE, Vasculitis, & JDM
Session Type: Poster Session D
Session Time: 9:00AM-11:00AM
Background/Purpose: Prior studies indicate that schizophrenia and systemic lupus erythematosus (SLE) share genetic risk loci. Despite overlapping phenotypic features such as psychosis, little is known of the link between genetic susceptibility for schizophrenia and neuropsychiatric SLE (NPSLE). We aimed to examine the association between a polygenic risk score (PRS) for schizophrenia and NPSLE as well as NPSLE feature subtypes in childhood-onset SLE (cSLE) patients.
Methods: Study participants from the cSLE Lupus Clinic at the Hospital for Sick Children, met ≥ 4 of the ACR and/or SLICC SLE classification criteria. Patients were genotyped on the multiethnic Illumina MEGA array. Un-genotyped single nucleotide polymorphisms (SNPs) were imputed. Principal components (PCs) were calculated using the 1000 Genomes Project (1KGP) and the Haplotype Reference Consortium as referents and ancestry was genetically inferred. We calculated an additive schizophrenia risk-weighted PRS using genome-wide significant SNPs (P< 5x10-8) from the largest published schizophrenia GWAS to date. The following SNPs were excluded: insertion/deletions, sex chromosomes, MHC region, minor allele frequency < 5%, imputation quality < 0.8 and SNPs within 500kb of and in r2 ≥ 0.1 with more significant markers. Demographic and clinical data were extracted from the Lupus database. NPSLE events were defined using ACR case definitions. We defined two outcomes compared to absence of NPSLE features: 1) any NPSLE features and 2) subtypes of NPSLE features: psychosis, headaches and/or mood disorders, other NPSLE. NPSLE features were independently validated by two pediatric rheumatologists. We tested the association of the schizophrenia PRS and NPSLE using logistic and multinomial regressions, adjusted for sex, age at SLE diagnosis, follow-up duration, the first five PCs, the presence of antiphospholipid antibodies, and non-HLA SLE PRS.
Results: Our cohort included 471 participants with cSLE. Median age at SLE diagnosis was 13.8 years (IQR,11.3-15.6), 82% were female and 31% were European. In total, 42% of all participants had ≥1 NPSLE feature: 59 (13%) had psychosis, 87 (18%) had headaches and/or mood disorders and 50 (11%) had other NPSLE features. Median follow-up was 5.0 years (IQR,3.2-7.8). The GWAS PRS included 83 SNPs. A higher schizophrenia PRS was not significantly associated with having any NPSLE features versus having no NPSLE features (OR=1.18, 95%CI 0.73-1.94, p=0.49). A higher schizophrenia PRS was not significantly associated with having psychosis (OR=0.92, 95%CI 0.44-1.94, p=0.84), headaches and/or mood disorders (OR=1.05, 95%CI 0.56-1.98, p=0.88) or other NPSLE features (OR=1.96, 95%CI 0.86-4.46, p=0.11) compared to having no NPSLE features (Figure).
Conclusion: We did not observe a statistically significant association between PRS for schizophrenia and NPSLE features in cSLE. We found a trend toward significance with higher schizophrenia PRS being associated with a higher odds of non-psychosis NPSLE features, which warrants further validation. Next steps include creating a PRS adding SNPs moderately associated with schizophrenia and testing the association with NPSLE.
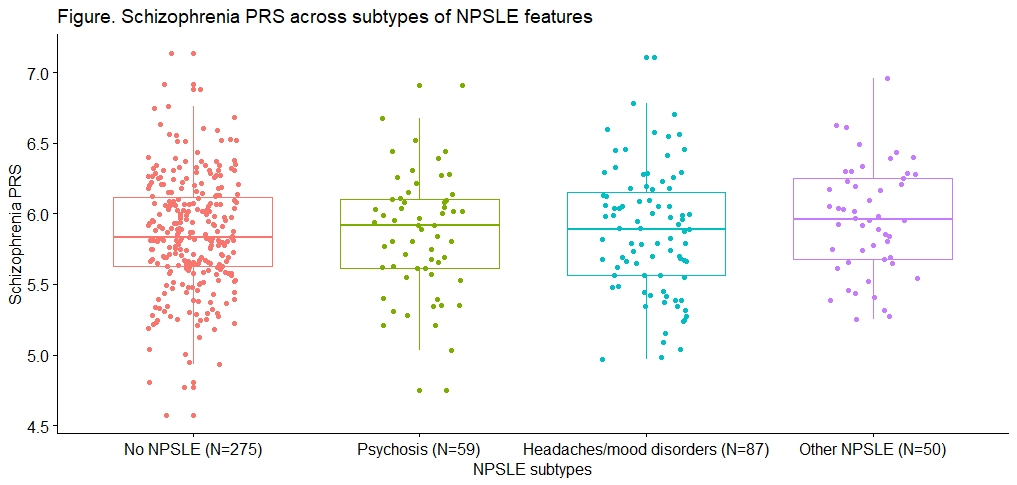 NPSLE, neuropsychiatric systemic lupus erythematosus; PRS, polygenic risk scores.
NPSLE, neuropsychiatric systemic lupus erythematosus; PRS, polygenic risk scores.
To cite this abstract in AMA style:
Ulloa Baez A, Liao F, Carlomagno R, Diaz T, Dominguez D, Levy D, Ng L, Silverman E, Knight A, Hiraki L. Schizophrenia Genetics and Neuropsychiatric Features in Childhood-Onset Systemic Lupus Erythematosus [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/schizophrenia-genetics-and-neuropsychiatric-features-in-childhood-onset-systemic-lupus-erythematosus/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/schizophrenia-genetics-and-neuropsychiatric-features-in-childhood-onset-systemic-lupus-erythematosus/
