Session Information
Date: Tuesday, November 12, 2019
Title: Patient Outcomes, Preferences, & Attitudes Poster II: Patient Preferences, Beliefs, & Experiences
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Treatment of rheumatoid arthritis (RA) to remission optimally ensures control of symptoms, prevention of structural damage, optimization of function and quality of life. Adherence to medical treatment is, therefore, critical for a comprehensive and successful management of RA. We interrogated the influence of distinct domains of RA clinical impact (disease activity, functional limitation, mood disturbance), RA-specific knowledge and patients’ beliefs about medications on treatment adherence.
Methods: We evaluated 285 patients from a single center. In the proposed model, disease activity (DAS28CRP),mood disturbance (Patient Health Questionnaire-9 depression scale and SF-36 Mental Health domain), functional limitations (Health Assessment Questionnaire Disability Index and SF-36 Physical Function domain) and RA-specific knowledge (Patient Knowledge Questionnaire) were expected to predict beliefs about the necessity of RA medications and concerns about them (Beliefs about Medicines Questionnaire); in turn, those would impact adherence (Simplified Medication Adherence Questionnaire). Cross-sectional multi-group structural equation modeling evaluated the model separately in patients on bDMARDs on csDMARDs.
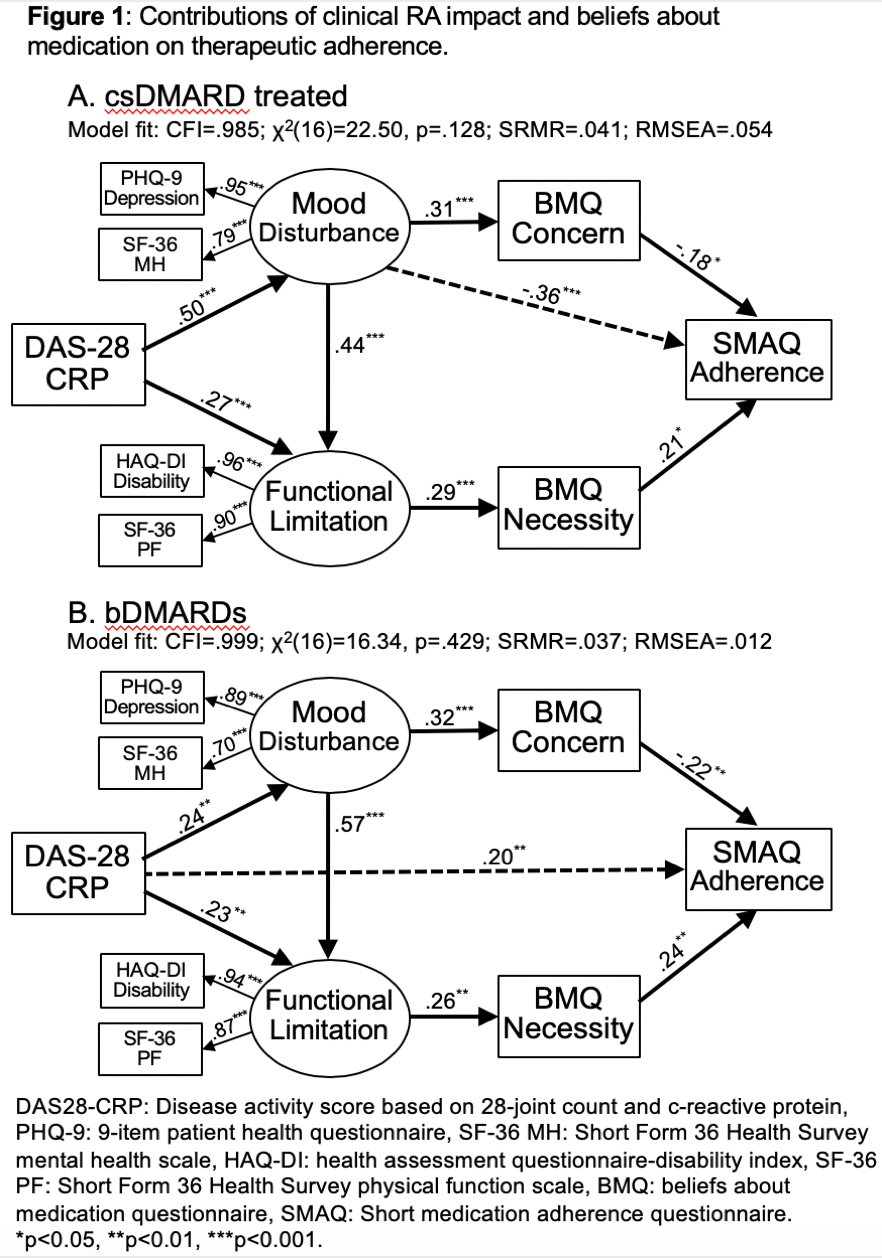
Results: RA-knowledge was not associated with medication beliefs or adherence and therefore dropped from the model. Addition of two supplementary paths (dashed lines) improved the model fit for both treatment groups (Figure 1). RA activity, functional limitations and mood disturbance influenced adherence via multiple, often competing pathways, directly or indirectly through a necessity/ concerns evaluation by the patient. RA activity directly promoted adherence in patients on bDMARDs (p< 0.01). In contrast, in patients on csDMARDs, RA activity had an indirect, net negative effect on adherence (p< 0.01), mainly through worsening mood disturbance (p< 0.01). Therefore, the experience of disease activity in patients on bDMARDs may be sufficiently impactful to independently promote medication adherence.In contrast, RA activity may be largely experienced as depressed mood in patients on csDMARDs, overwhelming their capacity to adhere. Mood disturbance adversely influenced adherence directly in patients on csDMARDs (p< 0.01); yet there was no significant direct or net indirect effect of mood disturbance on adherence to biologics. Functional limitations fostered adherence through enhanced awareness of medication necessity (p< 0.05).
Conclusion: Distinct domains of clinical RA impact influence treatment adherence directly or indirectly through a necessity/ concerns framework. Mood disturbance and medication concerns may represent complementary yet salient intervention targets of RA management promoting adherence; the former may be more relevant in patients on csDMARDs whereas the latter in those on bDMARDs.
To cite this abstract in AMA style:
Karpouzas G, Hernandez E, Ruiz L, Strand V, Ormseth S. Role of Clinical Impact, Disease-specific Knowledge and Beliefs About Medication on Therapeutic Adherence in Rheumatoid Arthritis: An Integrative Structural Equation Modeling Approach [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/role-of-clinical-impact-disease-specific-knowledge-and-beliefs-about-medication-on-therapeutic-adherence-in-rheumatoid-arthritis-an-integrative-structural-equation-modeling-approach/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/role-of-clinical-impact-disease-specific-knowledge-and-beliefs-about-medication-on-therapeutic-adherence-in-rheumatoid-arthritis-an-integrative-structural-equation-modeling-approach/